## Diagnosis of Acute Compartment Syndrome **Key Point:** Compartment syndrome is a clinical diagnosis, but when clinical suspicion is high and examination findings are equivocal, compartment pressure measurement is the gold standard confirmatory test. ### Why Compartment Pressure Measurement? **High-Yield:** Compartment pressure measurement using needle manometry or slit catheter technique is the definitive investigation because: - Provides objective, quantifiable data - Allows comparison with diastolic blood pressure - Guides surgical decision-making (fasciotomy indicated when pressure ≥ 30 mmHg or within 30 mmHg of diastolic BP) - Can be done rapidly at bedside without delay ### Interpretation Criteria | Pressure Threshold | Clinical Action | | --- | --- | | < 10 mmHg | Normal, observe | | 10–20 mmHg | Borderline, repeat in 2–4 hours | | 20–30 mmHg | High suspicion, prepare for fasciotomy | | ≥ 30 mmHg OR within 30 mmHg of diastolic BP | Fasciotomy indicated | **Clinical Pearl:** In this case, the patient has the classic pentad of compartment syndrome: 1. Severe pain out of proportion 2. Pain on passive stretch (most sensitive sign) 3. Tense compartments 4. Preserved pulses (compartment syndrome can occur before vascular compromise) 5. Paresthesias may develop later ### Timing **Warning:** Do NOT delay fasciotomy while waiting for imaging. If clinical suspicion is high, proceed to fasciotomy based on clinical signs alone. Compartment pressure measurement should not delay treatment when diagnosis is clinically evident. **Mnemonic:** **5 P's of Compartment Syndrome** — Pain (out of proportion), Pressure (elevated), Paresthesias, Pallor, Pulselessness (late sign). [cite:Campbell's Operative Orthopaedics 13e Ch 56] 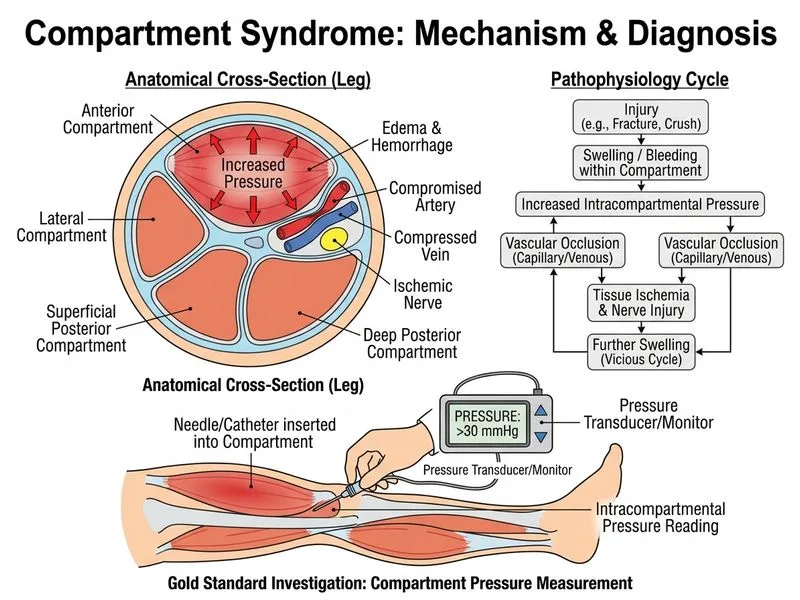
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.