## Distinguishing Acute Compartment Syndrome from DVT ### Key Clinical Discriminator **Key Point:** Pain out of proportion to clinical findings that worsens with passive stretch of muscles in the affected compartment is the hallmark and most specific clinical sign of acute compartment syndrome. ### Pathophysiology Basis In compartment syndrome, increased intracompartmental pressure compresses nerves and muscles, causing: 1. Severe pain that is disproportionate to visible swelling 2. Pain that increases dramatically with passive stretching of muscles within the compartment (stretch pain) 3. This occurs because passive stretch further increases pressure and ischemia In DVT, pain is typically: - Associated with visible swelling and edema - Not significantly worsened by passive stretch - Often accompanied by systemic signs (fever, elevated D-dimer) ### Comparison Table | Feature | Compartment Syndrome | DVT | | --- | --- | --- | | **Pain character** | Severe, out of proportion | Proportionate to swelling | | **Passive stretch pain** | **Marked increase** | Minimal change | | **Swelling** | Tense, firm compartment | Pitting edema | | **Skin changes** | Pallor, mottling, late blistering | Cyanosis, warmth | | **Onset** | Acute (hours) | Gradual (24–48 hrs) | | **Compartment pressure** | Elevated (>30 mmHg) | Normal | | **Imaging** | Clinical diagnosis; CT/MRI shows edema | Compression ultrasound positive | ### Clinical Pearl **Clinical Pearl:** The "5 P's" mnemonic (Pain, Pressure, Pallor, Paresthesia, Pulselessness) applies to compartment syndrome, but **pain with passive stretch** is the earliest and most sensitive clinical sign — often present before other signs develop. Pulselessness is a late finding indicating irreversible damage. ### High-Yield Fact **High-Yield:** Compartment syndrome is a surgical emergency. Diagnosis is clinical; do NOT delay fasciotomy waiting for imaging or pressure measurement. The combination of severe pain out of proportion + pain on passive stretch in a high-risk scenario (crush injury, tight cast, rhabdomyolysis) mandates immediate fasciotomy. ### Why Imaging Is Not the Discriminator While compartment syndrome can be confirmed by measuring intracompartmental pressure (>30 mmHg or within 30 mmHg of diastolic BP is concerning), clinical examination — specifically pain with passive stretch — remains the gold standard discriminator and should never be delayed for testing. 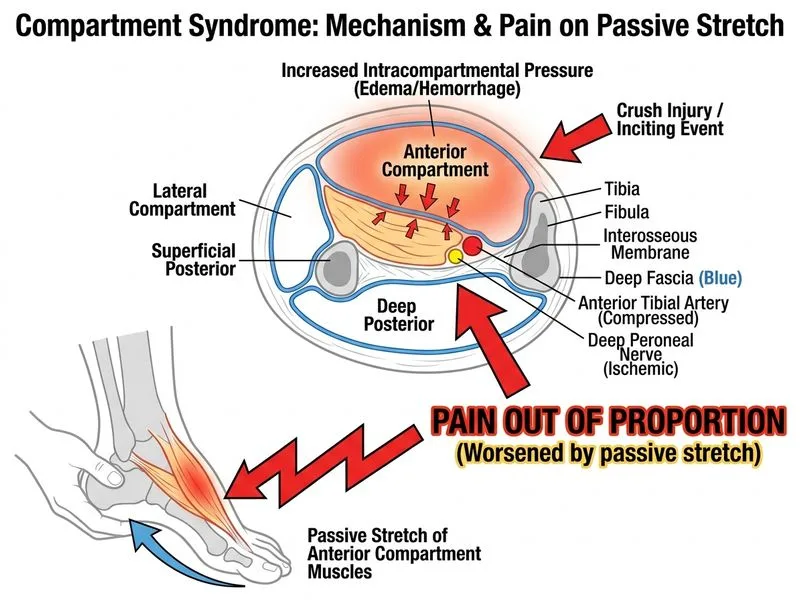
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.