## Open Fracture Infection — Early Recognition and Management ### Clinical Presentation of Infection The patient has signs of established infection at the fracture site: - Fever and systemic signs (tachycardia) - Purulent drainage (hallmark of bacterial colonization/infection) - Gram-positive cocci in clusters → **Staphylococcus aureus** (most common organism in open fractures) - Timeline: 8 hours post-injury + 2 days = day 2 presentation (early infection phase) **Key Point:** In an open fracture with clinical signs of infection (fever, purulent drainage, positive Gram stain), the diagnosis is established. Immediate surgical intervention is mandatory. ### Why Urgent Surgery Is Correct Open fracture infection is a surgical emergency. The goals are: 1. **Remove devitalized tissue and foreign material** (bacteria biofilm, contaminated bone fragments) 2. **Irrigate thoroughly** to reduce bacterial load 3. **Stabilize the fracture** (external fixation or internal fixation depending on grade) 4. **Prevent progression** to osteomyelitis, sepsis, or limb-threatening complications **High-Yield:** The **Gustilo-Anderson classification** guides management: - **Grade I (clean, <1 cm wound):** Primary closure possible; oral antibiotics may suffice - **Grade II (1–10 cm wound, moderate contamination):** Debridement + IV antibiotics - **Grade III (>10 cm, severe contamination, or vascular injury):** Urgent debridement, IV antibiotics, often external fixation This patient's comminuted fracture with purulent drainage suggests **Grade II or III**. ### Antibiotic Strategy - **Do NOT wait for culture results.** Start **empiric IV antibiotics immediately** (within 1 hour of diagnosis). - **First-line:** Cephalosporin (cefazolin or ceftriaxone) + gentamicin (covers Staph, Gram-negative rods, and anaerobes) - **If MRSA suspected or confirmed:** Add vancomycin or linezolid - **Gram stain shows Gram-positive cocci in clusters** → Staph aureus likely; cephalosporin + gentamicin covers this pending culture confirmation **Clinical Pearl:** Antibiotics PLUS surgery are both essential. Antibiotics alone cannot penetrate devitalized tissue or biofilm; surgery removes the source. ### Management Algorithm ```mermaid flowchart TD A[Open fracture with fever, purulent drainage, positive Gram stain]:::outcome --> B{Infection confirmed?}:::decision B -->|Yes: clinical signs + Gram stain| C[Start IV antibiotics immediately]:::action C --> D[Urgent surgical debridement & irrigation]:::urgent D --> E[Stabilize fracture]:::action E --> F[Send cultures, adjust antibiotics per results]:::action F --> G[Serial debridement if needed]:::action G --> H[Healing & rehabilitation]:::outcome ``` ### Why Other Options Fail - **Vancomycin alone + defer surgery:** Waiting for culture results delays source control. Devitalized tissue and biofilm are not penetrated by antibiotics; surgery is non-negotiable in the first 24–48 hours. - **Topical dressing + observation:** This is palliative only. Purulent drainage and fever indicate systemic infection; observation risks progression to osteomyelitis, sepsis, and amputation. - **MRI before surgery:** Imaging is not needed when the diagnosis is clinically clear (fever, purulent drainage, positive Gram stain). MRI delays urgent debridement and increases morbidity. **Warning:** Do NOT confuse "obtaining culture results" with "delaying surgery." Cultures are obtained **during surgery** (intraoperative samples from debrided tissue). Surgery proceeds immediately; antibiotics are adjusted once sensitivities are known. 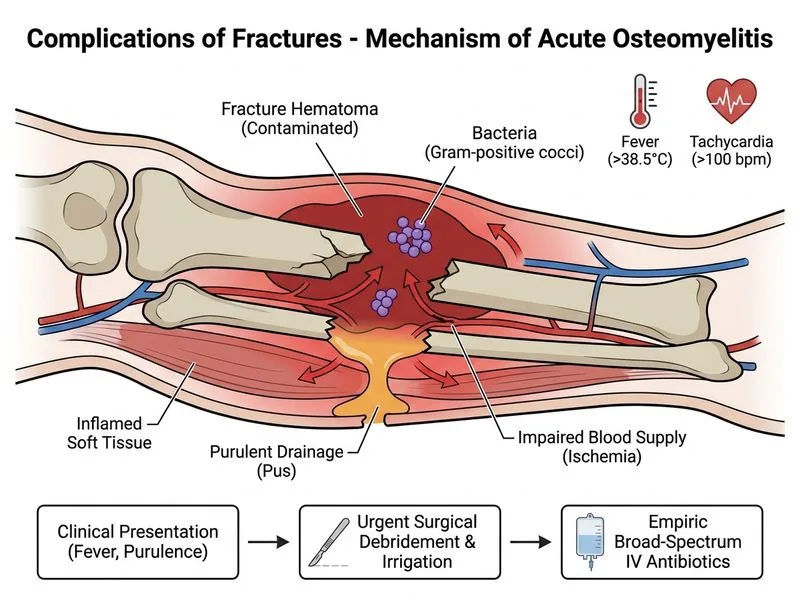
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.