## Nonunion vs. Delayed Union: Pathophysiology and Classification ### Diagnostic Criteria for Nonunion **Key Point:** Nonunion is defined as a fracture that has not healed after 6 months OR shows no radiographic evidence of healing for 3 consecutive months. This patient is at 8 weeks with: - No callus formation - Persistent fracture line - No bridging bone These findings indicate nonunion is already developing, not merely delayed union. ### Classification of Nonunion ```mermaid flowchart TD A[Nonunion]:::outcome --> B{Radiographic<br/>appearance?}:::decision B -->|Hypertrophic:<br/>bulbous callus| C[Adequate blood supply<br/>Poor mechanical stability]:::outcome B -->|Atrophic:<br/>no callus| D[Poor blood supply<br/>Poor bone quality]:::outcome C --> E[Causes: inadequate<br/>immobilization, motion]:::outcome D --> F[Causes: osteoporosis,<br/>age, comorbidities]:::outcome E --> G[Rx: rigid fixation]:::action F --> H[Rx: bone graft +<br/>rigid fixation]:::action ``` ### Why This Patient Has Atrophic Nonunion **High-Yield:** Atrophic nonunion occurs when bone quality is poor (osteoporosis) and/or blood supply is compromised. The surgical neck of the humerus has a precarious blood supply; combined with osteoporosis, this creates a hostile environment for healing: 1. **Osteoporosis** = reduced bone mineral density, impaired osteoblast function, and poor callus formation 2. **Surgical neck location** = vulnerable to vascular compromise (the anterior circumflex humeral artery is the main blood supply) 3. **Conservative treatment (sling)** = some micromotion, but in osteoporotic bone, this is insufficient to stimulate healing ### Atrophic vs. Hypertrophic Nonunion | Feature | Atrophic | Hypertrophic | |---------|----------|-------------| | **Callus formation** | Absent or minimal | Abundant, bulbous | | **Fracture line** | Clearly visible, sclerotic edges | Obscured by callus | | **Blood supply** | Poor | Adequate | | **Bone quality** | Poor (osteoporosis, age, comorbidity) | Usually good | | **Primary cause** | Vascular insufficiency, poor bone stock | Inadequate immobilization, motion | | **Treatment** | Bone graft + rigid fixation | Rigid fixation (compression plating) | | **Prognosis** | Slower healing; higher failure rate | Good with rigid fixation | ### Clinical Pearl **Osteoporosis is a major risk factor for nonunion**, particularly in elderly women. Fractures in osteoporotic bone heal more slowly and incompletely because: - Osteoblasts are dysfunctional - Callus formation is impaired - Bone resorption exceeds formation - Vascularity is often compromised ### Why Delayed Union Does Not Fit **Warning:** Delayed union is defined as healing that takes longer than expected (typically >3–4 months for most fractures) but eventually heals with appropriate treatment. This patient shows NO radiographic evidence of healing at 8 weeks — no callus, persistent fracture line. This is nonunion, not delayed union. ### Management of Atrophic Nonunion 1. **Rigid internal fixation** (compression plating, intramedullary nailing) 2. **Autologous bone graft** (gold standard) or allograft 3. **Biological enhancement** (BMP, PRP) in selected cases 4. **Address osteoporosis** (calcium, vitamin D, bisphosphonates) **Tip:** The surgical neck of the humerus is a notorious site for nonunion; proximal humerus fractures in elderly osteoporotic patients require careful attention to vascular supply and often benefit from early surgical fixation rather than conservative treatment. 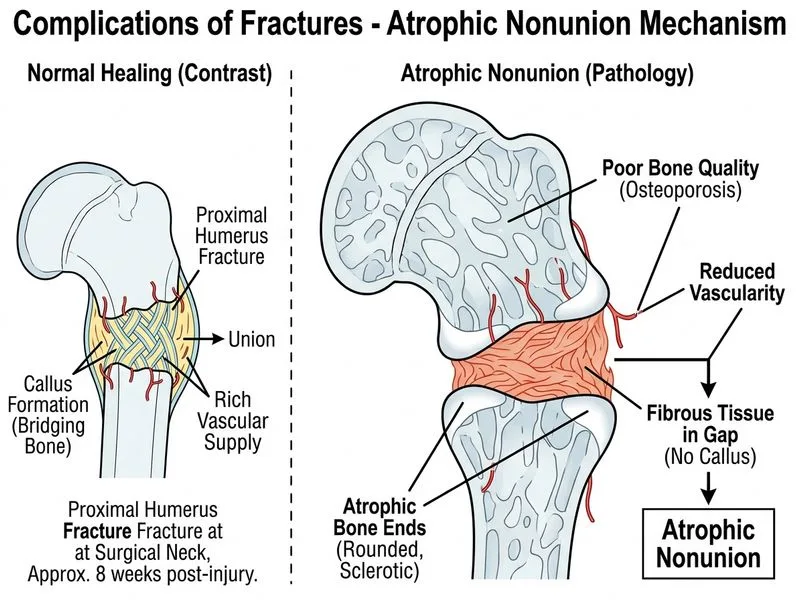
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.