## Avascular Necrosis: Fracture-Related Risk **Key Point:** Femoral neck fractures, particularly intracapsular (subcapital and transcervical), carry the highest risk of AVN due to the precarious blood supply to the femoral head. ### Vascular Anatomy of Femoral Head The femoral head receives blood supply from: 1. **Medial femoral circumflex artery (MFCA)** — primary source (80%) 2. **Lateral femoral circumflex artery (LFCA)** — secondary source 3. **Ligamentum teres artery** — minimal contribution (only in children) **Critical Point:** Intracapsular femoral neck fractures disrupt the ascending cervical branches of MFCA, leading to femoral head ischemia. ### Risk of AVN by Fracture Location | Fracture Location | AVN Risk | Reason | |---|---|---| | **Femoral neck (intracapsular)** | **20–50%** | Disrupts MFCA branches; risk increases with displacement and delay in treatment | | Femoral neck (extracapsular) | < 5% | Preserves blood supply | | Proximal humerus | 5–10% | Retrograde blood supply; risk with 4-part fractures | | Distal radius | < 1% | Rich collateral circulation | | Proximal tibia | < 1% | Excellent blood supply | **High-Yield:** The risk of AVN in femoral neck fractures correlates with: - **Displacement:** undisplaced < 10%; displaced > 30% - **Delay in reduction:** > 12 hours increases risk - **Age:** higher in adults > 50 years - **Fracture type:** subcapital > transcervical > intertrochanteric ### Mechanism of AVN in Femoral Neck Fractures 1. Fracture disrupts MFCA branches at femoral neck 2. Femoral head becomes dependent on retrograde flow via ligamentum teres (minimal in adults) 3. Prolonged ischemia → osteocyte death → collapse of articular surface 4. Typically manifests 6–24 months post-fracture **Mnemonic:** **SHAFT** — Sites of high AVN risk: - **S**capula (proximal pole) - **H**umerus (proximal) - **A**stragalus (talus) - **F**emoral head (femoral neck fracture) - **T**alus **Clinical Pearl:** Early diagnosis of AVN requires high clinical suspicion. MRI is the gold standard for detecting AVN before radiographic changes appear (T1-weighted images show band-like low signal). ### Prevention & Management - **Early reduction:** < 12 hours (reduces ischemic time) - **Internal fixation:** cannulated screws or plates to maintain reduction - **Monitoring:** serial radiographs at 6, 12, 18 months; MRI if symptoms develop - **Treatment of established AVN:** core decompression (early stage), arthroplasty (advanced stage) [cite:Rockwood & Green's Fractures in Adults Ch 51] 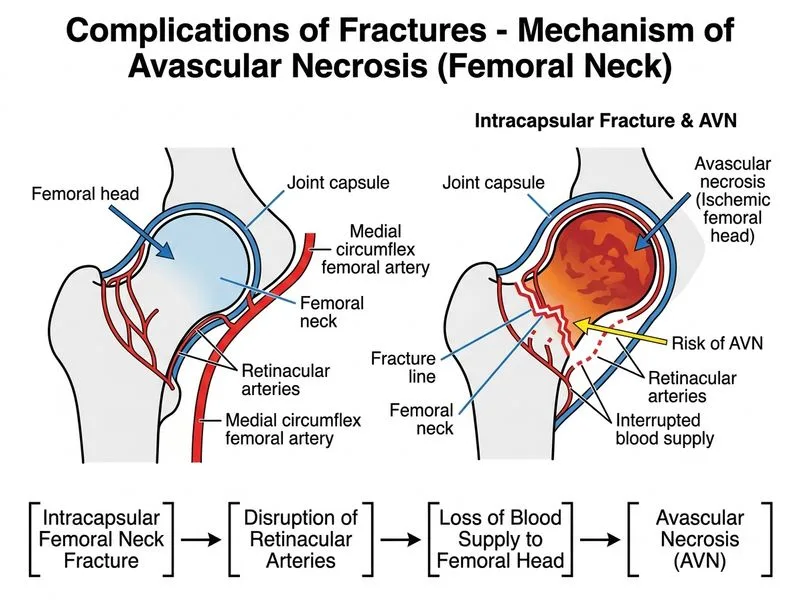
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.