## Diagnosis of Compartment Syndrome **Key Point:** Compartment syndrome is a surgical emergency requiring early diagnosis based on clinical suspicion and objective pressure measurement — not imaging. ### Why Compartment Pressure Measurement is Gold Standard Compartment syndrome results from increased interstitial pressure within a fascial compartment, compromising microvascular perfusion and tissue viability. The diagnosis rests on: 1. **Clinical suspicion** (pain out of proportion, pain on passive stretch, paresthesias, pallor, pulselessness is a late sign) 2. **Objective pressure confirmation** using a needle manometer or slit catheter inserted into the compartment **High-Yield:** The critical pressure threshold is when compartment pressure exceeds diastolic blood pressure by >30 mmHg (or absolute pressure >30 mmHg in normotensive patients). This is the indication for emergency fasciotomy. ### Why Other Investigations Fail | Investigation | Limitation | |---|---| | Plain radiograph | Shows only bone; cannot assess soft tissue pressure or muscle viability | | Doppler ultrasound | Assesses vascular flow but does not measure compartment pressure; pulses may remain intact early in CS | | MRI | Slow, not available emergently; delays definitive treatment | **Clinical Pearl:** Compartment syndrome is a **clinical diagnosis** confirmed by pressure measurement. Do NOT wait for imaging. Delay in fasciotomy beyond 6–8 hours leads to irreversible muscle necrosis and permanent disability. **Warning:** Absence of pulselessness does NOT rule out compartment syndrome — it is a late finding. Proceed to fasciotomy based on clinical suspicion + pressure confirmation. **Mnemonic:** **5 P's of compartment syndrome** — Pain (out of proportion), Pressure (elevated compartment pressure), Paresthesias, Pallor, Pulselessness (late). The first three are early; the last two are late. 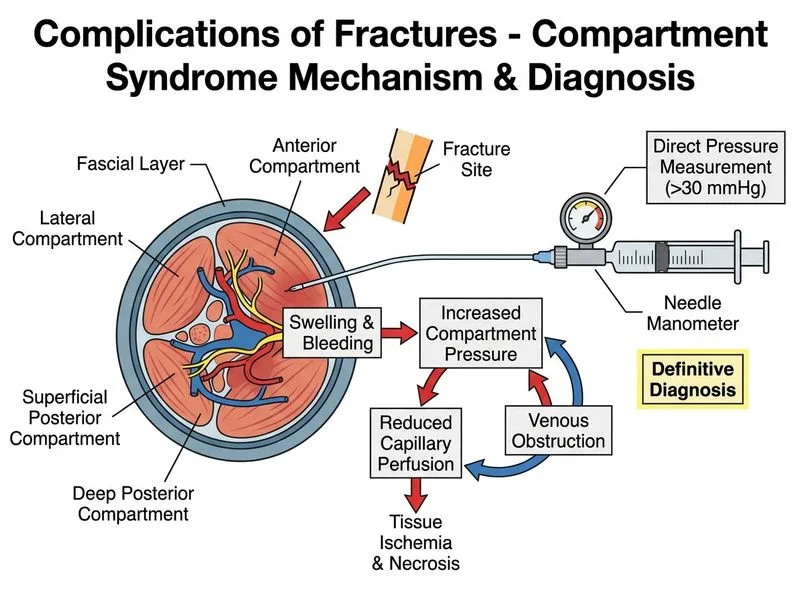
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.