## Diagnosis of Post-Traumatic Osteomyelitis **Key Point:** Post-traumatic osteomyelitis requires microbiological confirmation (culture and sensitivity) from bone tissue to guide targeted antibiotic therapy. Blood cultures are low-yield in chronic osteomyelitis. ### Why Bone Biopsy is Gold Standard Osteomyelitis complicating a fracture (especially after 2–3 weeks) is a **bone infection** requiring: 1. **Microbiological diagnosis** — culture of bone tissue to identify causative organism 2. **Sensitivity testing** — to guide appropriate antibiotic selection 3. **Histopathology** — to confirm inflammation and rule out other diagnoses (malignancy, necrosis) **High-Yield:** Bone biopsy (via open surgical approach or percutaneous needle biopsy under image guidance) is the **gold standard** for diagnosing osteomyelitis and obtaining material for culture and sensitivity. ### Comparison of Investigations | Investigation | Sensitivity | Specificity | Role | |---|---|---|---| | **Bone biopsy + culture** | 90–95% | 95–100% | Gold standard; guides therapy | | Blood culture | 30–50% in chronic OM | High | Low yield in post-traumatic OM | | Tc-99m bone scan | High (80–90%) | Low (50–60%) | Detects osteomyelitis but not specific; cannot guide antibiotics | | CT scan | Detects bone destruction | Not specific | Shows anatomical changes; does not identify organism | **Clinical Pearl:** In post-traumatic osteomyelitis, blood cultures are often negative because infection is localized to bone. Bone tissue culture is essential. **Warning:** Do NOT rely on blood culture alone in chronic or post-traumatic osteomyelitis — it will delay diagnosis and appropriate therapy. Bone biopsy is mandatory. **Mnemonic:** **BIOPSY for OMY** — Bone biopsy is the gold standard for Osteomyelitis diagnosis, yielding organism identification and sensitivity data. 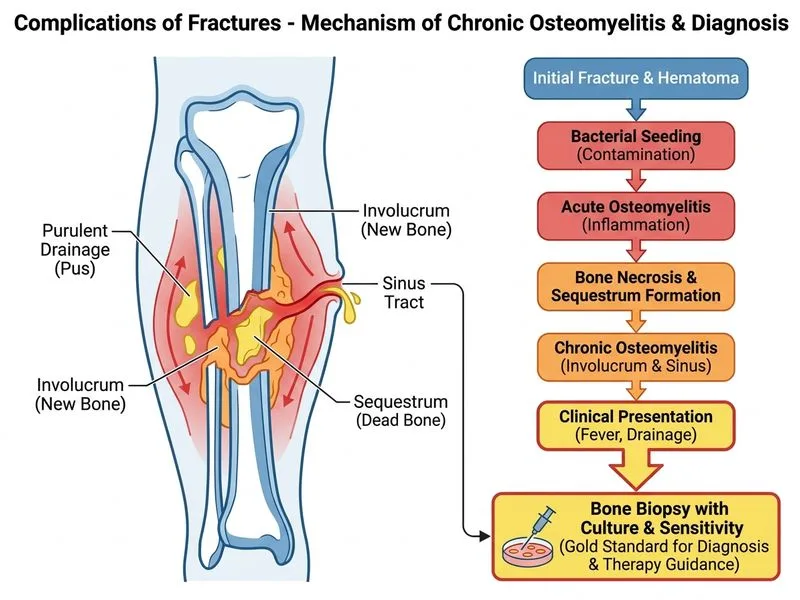
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.