## Clinical Presentation of Early Surgical Site Infection (SSI) This patient has **acute post-operative infection** (day 3 post-ORIF): - Fever within 72 hours of surgery - Purulent drainage (hallmark of bacterial infection) - Systemic signs: tachycardia, fever - Timeline: Early SSI (typically Gram-positive cocci or Gram-negative organisms from skin flora or environment) ## Pathophysiology of Post-Operative Fracture Infection **Key Point:** Early post-operative SSI (within 30 days) is typically caused by intraoperative contamination with skin flora (*Staphylococcus aureus*, *S. epidermidis*, *Streptococcus*, Gram-negative rods). **High-Yield:** In acute post-operative infection with systemic signs, **empiric antibiotics must be started immediately** — do NOT delay for culture results. Cultures are obtained *before* antibiotics to guide later de-escalation, but treatment cannot wait. ## Why Empiric Broad-Spectrum Antibiotics + Culture Is Correct 1. **Time-critical decision:** Every hour of untreated infection increases risk of biofilm formation on hardware, osteomyelitis, and sepsis. 2. **Empiric coverage is standard:** Broad-spectrum regimen (3rd-generation cephalosporin + vancomycin ± aminoglycoside) covers most likely pathogens (MSSA, MRSA, Gram-negative rods). 3. **Culture guides de-escalation:** Wound and blood cultures identify the organism and allow narrowing of antibiotics after 48–72 hours. 4. **Guideline standard:** Orthopedic infection guidelines (AAOS, ACCP) recommend empiric antibiotics within 1 hour of diagnosis of SSI. 5. **Wound exploration is NOT the immediate first step:** Antibiotics and cultures come first; surgical intervention (debridement, hardware removal) is decided after clinical response and imaging (e.g., X-ray for loosening, CT for abscess). ## Management Algorithm for Post-Operative SSI ```mermaid flowchart TD A[Post-op fever + purulent drainage]:::outcome --> B[Obtain wound culture & blood culture]:::action B --> C[Start empiric broad-spectrum antibiotics]:::action C --> D[Clinical response at 48-72 hours?]:::decision D -->|Improving| E[De-escalate based on culture]:::action D -->|Worsening| F[Imaging: X-ray, CT, or MRI]:::action F --> G[Signs of hardware loosening or abscess?]:::decision G -->|Yes| H[Surgical debridement ± hardware removal]:::action G -->|No| I[Continue antibiotics, repeat cultures]:::action ``` **Clinical Pearl:** The decision to remove hardware depends on: - **Stability of fracture:** If fracture is bridged and stable (early callus on X-ray), hardware can be removed. - **Organism virulence:** Highly virulent organisms (e.g., *Pseudomonas*, *S. aureus*) or biofilm-forming organisms may necessitate hardware removal. - **Clinical response:** If infection resolves with antibiotics alone, hardware may be retained. ## Why Other Options Are Incorrect | Option | Why It's Wrong | |--------|----------------| | Immediate hardware removal | Premature; hardware removal is considered if infection does NOT respond to antibiotics within 48–72 hours or if imaging shows loosening/abscess. Early removal compromises fracture stability. | | Await culture results before antibiotics | Delays critical treatment; cultures guide *de-escalation*, not initiation. Sepsis and biofilm formation progress rapidly. | | Cephalosporin monotherapy | Inadequate coverage for MRSA (if present) and Gram-negative rods. Vancomycin is essential for empiric coverage pending culture. | **Warning:** A common trap is to assume that hardware must be removed immediately in any post-operative infection. In reality, hardware removal is a *later* decision based on clinical response and imaging findings, not an immediate reflex. 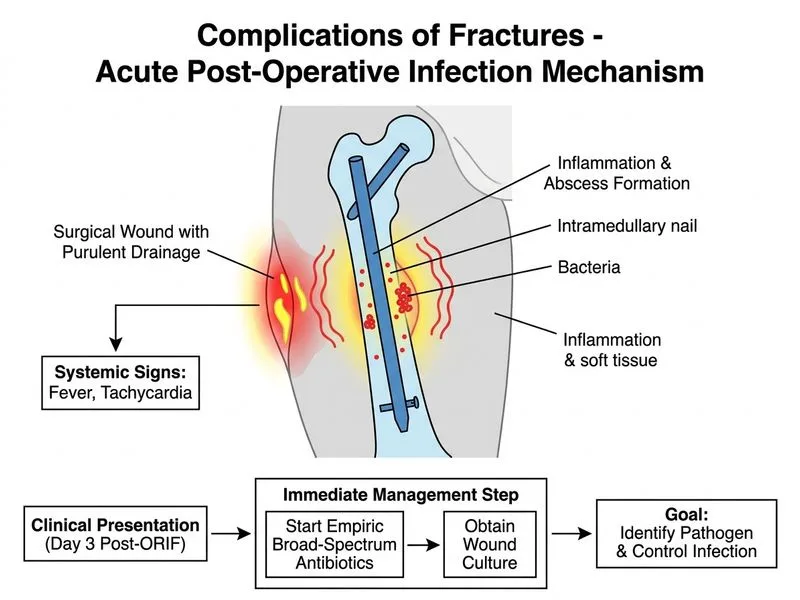
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.