## Clinical Presentation Analysis The clinical picture is highly suggestive of **Transposition of the Great Arteries (TGA)**: ### Key Clinical Features **Key Point:** TGA is the most common cyanotic congenital heart disease presenting in the first days of life with severe cyanosis that responds dramatically to prostaglandin E1 (PGE1). Maternal gestational diabetes is a well-recognized risk factor for TGA. ### Pathophysiology In TGA, the aorta arises from the right ventricle and the pulmonary artery from the left ventricle — creating two parallel, non-communicating circulations. Survival depends on mixing at one or more levels: - Patent foramen ovale (PFO) - Patent ductus arteriosus (PDA) - Atrial septal defect (ASD) PGE1 maintains ductal patency, allowing mixing of deoxygenated and oxygenated blood, which improves systemic oxygenation dramatically. ### The 'Machinery' Murmur — Important Clarification The continuous 'machinery' murmur heard at the left infraclavicular region in this case represents the **PDA itself**, not a structural murmur of TGA. TGA per se typically produces no murmur or only a soft murmur. The PDA is essential for survival in TGA and is the source of this auscultatory finding. This is consistent with Park's Pediatric Cardiology (26th ed.), which notes that TGA may present with a PDA murmur when ductal flow is significant. ### Diagnostic Clues in This Case | Feature | TGA | TOF | PA-IVS | |---------|-----|-----|--------| | **Age of presentation** | 0–3 days | 1–2 weeks | 0–3 days | | **Cyanosis severity** | Severe, "blue baby" | Moderate | Severe | | **Murmur** | Absent/soft (PDA murmur if present) | Loud systolic | Continuous (PDA) | | **CXR appearance** | "Egg on string," cardiomegaly | Boot-shaped heart | Cardiomegaly, decreased PBF | | **PGE1 response** | Dramatic improvement | Minimal | Improves (keeps PDA open) | | **Pulmonary vascularity** | Increased (pulmonary edema) | Decreased | Decreased | **High-Yield:** The combination of severe cyanosis in the first 72 hours, cardiomegaly with **pulmonary edema** (increased pulmonary blood flow), and dramatic improvement with PGE1 is characteristic of TGA. PA-IVS would show decreased pulmonary vascularity, not pulmonary edema, making it a less likely diagnosis here. ### Why Other Options Are Less Likely - **TOF (D):** Presents later (1–2 weeks), boot-shaped heart on CXR, decreased pulmonary vascularity, and does not respond dramatically to PGE1. - **PA-IVS (B):** Also ductal-dependent and presents early, but CXR shows decreased pulmonary vascularity (not pulmonary edema), and the heart may appear globular with a single S2. - **PDA in preterm (C):** PDA in isolation causes left-to-right shunting and does not cause cyanosis; it is not a cyanotic lesion. ### Management Timeline 1. **Immediate:** PGE1 infusion (0.05–0.1 μg/kg/min IV) to maintain ductal patency 2. **Stabilization:** Oxygen, correction of metabolic acidosis 3. **Bridge:** Balloon atrial septostomy (Rashkind procedure) 4. **Definitive:** Arterial switch operation (Jatene procedure) within first 2 weeks of life **Clinical Pearl:** In a severely cyanotic neonate with cardiomegaly, pulmonary edema, and dramatic PGE1 response, TGA must be the top diagnosis. The 'machinery' murmur reflects the life-sustaining PDA, not a primary structural defect of TGA itself. [cite: Park MK. Park's Pediatric Cardiology for Practitioners, 6th ed. Chapter on Cyanotic Congenital Heart Defects — Transposition of the Great Arteries] 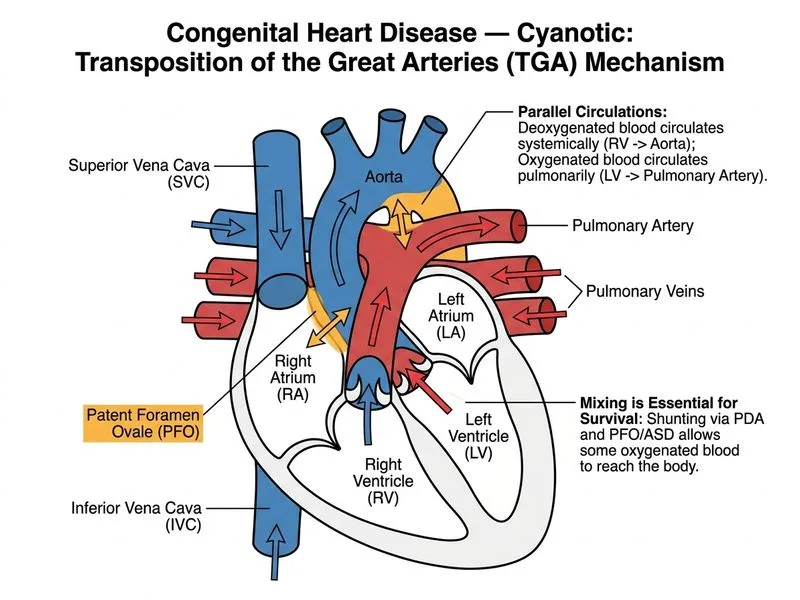
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.