## Tetralogy of Fallot (TOF): Classic Presentation **Key Point:** Tetralogy of Fallot is the most common cyanotic congenital heart disease beyond the neonatal period. It is defined by four anatomic features, all stemming from anterior and superior displacement of the infundibular septum. ### The Four Components of TOF | Feature | Pathophysiology | Clinical Consequence | |---------|-----------------|----------------------| | **1. Ventricular Septal Defect (VSD)** | Large, non-restrictive | Right-to-left shunt | | **2. Right Ventricular Outflow Tract (RVOT) Obstruction** | Infundibular and/or valvular stenosis | Increased RV pressure; forces deoxygenated blood rightward | | **3. Right Ventricular Hypertrophy** | Chronic RV pressure overload | RV heave on palpation | | **4. Overriding Aorta** | Aorta positioned over VSD (receives blood from both ventricles) | Receives deoxygenated blood from RV | **High-Yield:** The degree of cyanosis depends on the severity of RVOT obstruction, not the VSD size. Mild obstruction → acyanotic; severe obstruction → deeply cyanotic. ### Classic Clinical Features ```mermaid flowchart TD A[TOF pathophysiology]:::outcome --> B[RVOT obstruction severity]:::decision B -->|Mild| C[Acyanotic or pink TOF]:::outcome B -->|Moderate| D[Mild cyanosis, exercise intolerance]:::outcome B -->|Severe| E[Severe cyanosis from infancy]:::outcome E --> F[Clubbing, squatting posture]:::action F --> G[Tet spells: sudden cyanotic episodes]:::urgent G --> H[RV outflow obstruction worsens transiently]:::outcome ``` **Clinical Pearl:** Squatting posture (child assumes knee-chest position during cyanotic spells) increases systemic vascular resistance, reducing right-to-left shunt and improving oxygenation. This is pathognomonic for TOF. **Mnemonic: TOF = RVOT (Right Ventricular Outflow Tract obstruction is KEY)** - **V**entricular **S**eptal **D**efect - **R**ight **V**entricular hypertrophy - **O**verriding **A**orta - (Plus RVOT obstruction — the primary driver of cyanosis) ### Diagnostic Findings **Chest X-ray: Boot-shaped heart ('coeur en sabot')** - Upturned apex due to RV hypertrophy - Decreased pulmonary vascular markings (reduced pulmonary blood flow) - Right aortic arch in ~25% of cases **Echocardiography:** - Large VSD with rightward deviation of septum - RVOT obstruction (infundibular and/or valvular) - Overriding aorta (>50% over VSD) - RV hypertrophy **ECG:** - Right axis deviation - RV hypertrophy pattern (tall R in V1–V2) ### Management **Medical (Temporary stabilization during Tet spells):** - Oxygen, morphine, beta-blockers (propranolol) - Knee-chest position - Avoid dehydration (increases viscosity, worsens shunt) **Surgical (Definitive):** - **Corrective surgery:** VSD closure + RVOT obstruction relief (valve repair/conduit placement) - Timing: typically 3–6 months of age - Outcomes: excellent, with >95% long-term survival **Palliative (if surgery delayed):** - Prostaglandin E1 to keep ductus arteriosus patent - Blalock-Taussig shunt (systemic-to-pulmonary artery anastomosis) — rarely needed now [cite:Park 26e Ch 12] 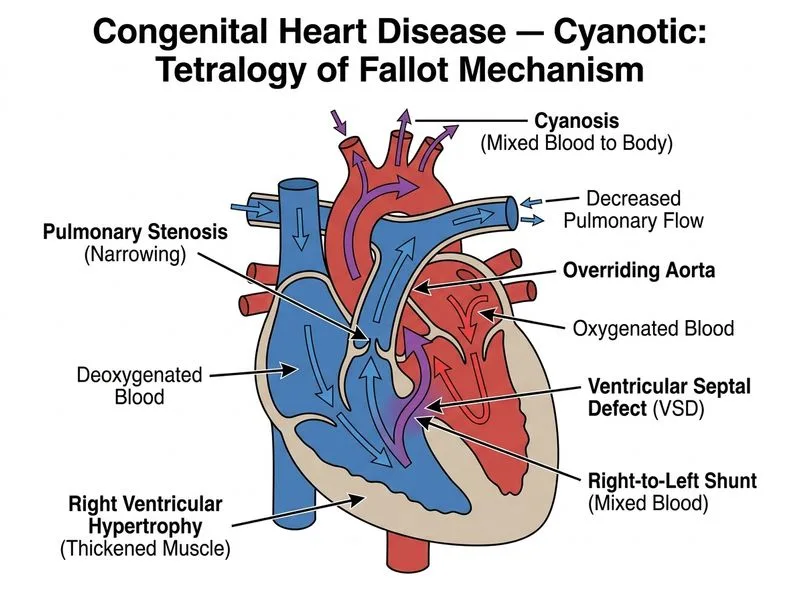
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.