## Tetralogy of Fallot — Acute Deterioration and Cyanotic Crisis ### Clinical Context Analysis **Key Point:** The history of prolonged crying → acute severe cyanosis, loss of consciousness, and convulsions is classic for an acute cyanotic spell in TOF, not a separate complication. ### Pathophysiology of Acute Deterioration in TOF During crying or exertion, several factors converge: 1. **Increased RVOT obstruction** — Catecholamine surge causes infundibular muscle spasm and increased dynamic obstruction 2. **Decreased systemic vascular resistance** — Crying/exertion causes peripheral vasodilation 3. **Increased right-to-left shunting** — Blood preferentially bypasses the lungs via the VSD 4. **Severe hypoxemia** — PaO₂ drops precipitously (38 mmHg in this case) 5. **Metabolic acidosis** — Tissue hypoxia → anaerobic metabolism → ↓ pH, ↓ HCO₃⁻ ### Mechanism of Syncope and Seizures ```mermaid flowchart TD A[Crying / Exertion]:::action --> B[↑ RVOT obstruction<br/>↓ SVR]:::action B --> C[↑ Right-to-left shunt]:::outcome C --> D[Severe hypoxemia<br/>PaO₂ < 40 mmHg]:::urgent D --> E[Cerebral hypoxia]:::urgent E --> F[Loss of consciousness]:::urgent E --> G[Seizures]:::urgent D --> H[Metabolic acidosis]:::urgent ``` ### Why NOT the Other Options | Option | Why Wrong | |---|---| | **Infective endocarditis** | No fever, no new murmur, no predisposing risk (acute onset). IE is a chronic complication, not an acute spell trigger. | | **Pulmonary edema / LV failure** | TOF is a right-to-left shunt; pulmonary blood flow is REDUCED, not increased. Pulmonary edema does not occur in uncomplicated TOF. | | **Ductal thrombosis** | TOF does not depend on ductal patency (unlike PDA-dependent lesions). The ductus is usually closed by age 2 years anyway. | **Clinical Pearl:** The **convulsions** in this case are due to **cerebral hypoxia**, not primary seizure disorder. Once oxygenation improves with emergency spell management, seizures typically resolve. ### Emergency Management Priorities 1. **Oxygen** — High-flow O₂ (100% if needed) 2. **Morphine** — 0.1 mg/kg IV (sedation + RVOT relief) 3. **Beta-blockers** — Propranolol 0.01–0.1 mg/kg IV (reduce infundibular obstruction) 4. **Knee-chest position** — If conscious enough 5. **Fluids** — IV access, cautious fluid bolus (maintain preload) 6. **Sodium bicarbonate** — If pH < 7.2 (correct acidosis) 7. **Consider ICU admission** — For mechanical ventilation if no response **High-Yield:** The ABG pattern — **low pH, low HCO₃⁻, low PaO₂** — is the signature of a cyanotic spell with **combined respiratory and metabolic acidosis**. **Mnemonic:** **"KBOM + ABG"** — Knee-chest, Beta-blockers, Oxygen, Morphine, plus correction of Acidosis, Blood gas monitoring, and Glucose/electrolyte support. [cite:Park 26e Ch 12; Ghai Essential Pediatrics 9e Ch 14] 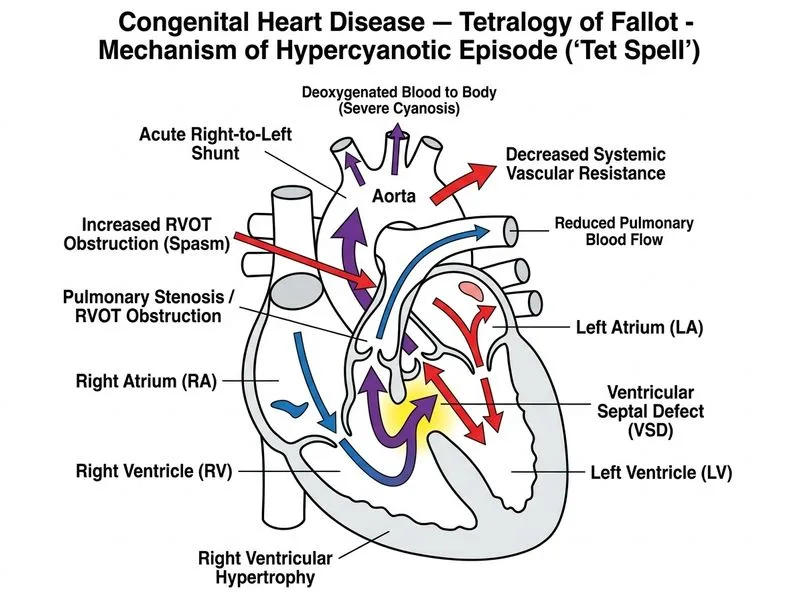
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.