## Diagnosis and Pathophysiology **Key Point:** This is a classic presentation of Tetralogy of Fallot (TOF), the most common cyanotic congenital heart defect beyond the neonatal period. The four anatomic components are: 1. Ventricular septal defect (VSD) 2. Right ventricular outflow tract obstruction (pulmonary stenosis) 3. Right ventricular hypertrophy (secondary to RVOT obstruction) 4. Overriding aorta (aorta positioned over the VSD) ## Clinical Features Confirming TOF | Feature | Significance | |---------|-------------| | Cyanosis at rest (SpO₂ 82%) | Indicates significant right-to-left shunt | | Squatting posture | Increases systemic vascular resistance, reduces right-to-left shunt | | Clubbing | Chronic hypoxemia | | Boot-shaped heart on CXR | Pathognomonic finding due to RV hypertrophy and small pulmonary artery | | Single loud S₂ | Pulmonary component diminished due to severe pulmonary stenosis | | Systolic ejection murmur at left upper sternal border | From pulmonary stenosis (RVOT obstruction) | ## Management Strategy **High-Yield:** At age 3 years with established TOF and significant cyanosis (SpO₂ 82%), the child is a candidate for **definitive surgical correction**. This is NOT a neonate with ductus-dependent pulmonary circulation. ### Surgical Timing in TOF - **Neonates with severe cyanosis (SpO₂ <75%):** Prostaglandin E₁ or Blalock–Taussig shunt as temporizing measure - **Infants/children with moderate cyanosis (SpO₂ 75–85%):** Preoperative optimization followed by **complete surgical repair** (closure of VSD + relief of RVOT obstruction) - **This 3-year-old:** Already has established disease; surgical repair is definitive and curative **Clinical Pearl:** The squatting posture is a compensatory mechanism the child has learned—it increases systemic vascular resistance and reduces the right-to-left shunt, temporarily improving oxygenation. This is a sign of severe disease and an indication for surgery. ### Preoperative Optimization - Iron supplementation (for polycythemia) - Hydration (to reduce blood viscosity) - Avoid dehydration and hypoxic spells - Antibiotic prophylaxis for infective endocarditis - Surgical repair is curative and should not be delayed ```mermaid flowchart TD A[Tetralogy of Fallot Diagnosis]:::outcome --> B{Age and Severity?}:::decision B -->|Neonate, SpO₂ < 75%| C[Prostaglandin E₁ or BT Shunt]:::action B -->|Infant/Child, SpO₂ 75-85%| D[Preoperative Optimization]:::action D --> E[Complete Surgical Repair]:::action E --> F[Closure of VSD + RVOT Relief]:::action F --> G[Curative]:::outcome B -->|Older child, stable| H[Elective Surgical Repair]:::action H --> G ``` **Key Point:** Surgical repair (not catheterization alone) is the definitive management for TOF in this age group. Catheterization may be done preoperatively for detailed anatomy if echocardiography is inconclusive, but it is not the primary next step. 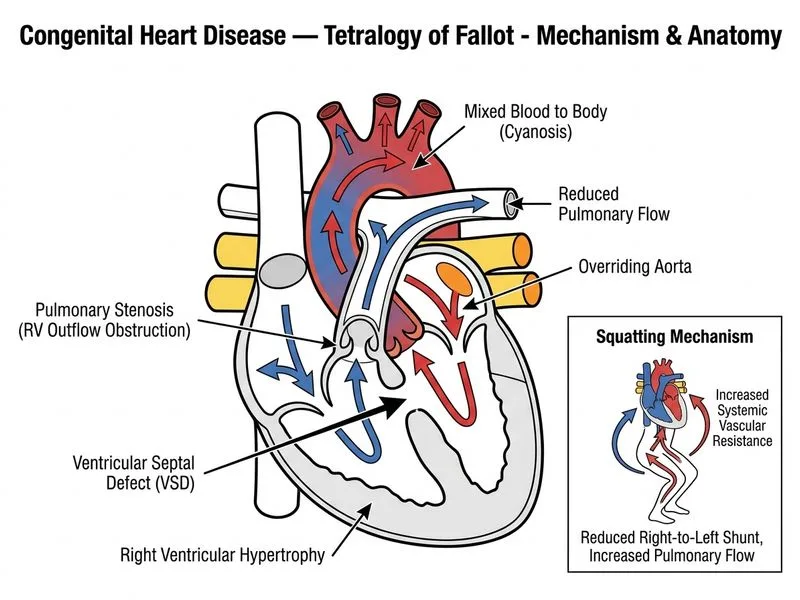
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.