## Hypercyanotic Spell in Tetralogy of Fallot **Key Point:** A hypercyanotic (or "Tet") spell is an acute, life-threatening episode of severe cyanosis caused by a sudden increase in right-to-left shunting through the VSD. This is a medical emergency requiring immediate intervention. ## Pathophysiology of Hypercyanotic Spells 1. **Trigger:** Increased right ventricular outflow tract obstruction (infundibular spasm) or decreased systemic vascular resistance 2. **Mechanism:** Increased right-to-left shunt → severe hypoxemia → syncope, seizures, or sudden death 3. **Timing:** Often occur in early morning, during crying, feeding, or defecation 4. **Frequency:** Indicate worsening disease and need for urgent surgical repair ## Immediate Management Algorithm ```mermaid flowchart TD A[Hypercyanotic Spell Suspected]:::urgent --> B[Place in Knee-Chest Position]:::action B --> C[High-Flow Oxygen]:::action C --> D[Morphine 0.1-0.2 mg/kg IV/IM]:::action D --> E{SpO₂ Improving?}:::decision E -->|Yes| F[Continue Monitoring]:::action E -->|No| G[Sodium Bicarbonate 1 mEq/kg IV]:::action G --> H{SpO₂ Improving?}:::decision H -->|Yes| I[Propranolol 0.1 mg/kg IV]:::action H -->|No| J[Prepare for Intubation/Sedation]:::urgent I --> K[Arrange Urgent Surgical Repair]:::action J --> K ``` ## Step-by-Step Management ### 1. **Knee-Chest Position** (First-Line) - Increases systemic vascular resistance - Reduces right-to-left shunt - Can be done immediately by parents or caregivers - Often resolves mild spells ### 2. **High-Flow Oxygen** - Increases PaO₂ and reduces hypoxic pulmonary vasoconstriction - Improves oxygenation of blood entering systemic circulation ### 3. **Morphine 0.1–0.2 mg/kg IV or IM** - **Mechanism:** Reduces infundibular spasm, decreases catecholamine surge, reduces anxiety - **Effect:** Decreases right-to-left shunt - **Onset:** 5–10 minutes ### 4. **Sodium Bicarbonate 1 mEq/kg IV** (if not responding) - Corrects metabolic acidosis (which worsens pulmonary vasoconstriction) - Improves systemic vascular resistance ### 5. **Propranolol 0.1 mg/kg IV** (if still not responding) - Beta-blocker that reduces infundibular contractility - Decreases heart rate and contractility - Reduces right-to-left shunt - **Caution:** Use only after hypoxemia is partially corrected **Warning:** Do NOT give propranolol as first-line; it can worsen hypoxemia if given before oxygenation is improved. ## When to Intubate - Persistent SpO₂ <60% despite above measures - Loss of consciousness or seizures - Respiratory muscle fatigue - **Sedation strategy:** Avoid agents that cause histamine release (atracurium, mivacurium); use propofol or etomidate ## Definitive Management **High-Yield:** Recurrent hypercyanotic spells indicate **urgent need for surgical repair**. Do not delay surgery waiting for medical optimization. | Intervention | Timing | Goal | |---|---|---| | Medical management (morphine, beta-blockers) | Acute spell | Stabilize, increase systemic resistance | | Surgical repair | Urgent (within days) | Definitive correction of RVOT obstruction | **Clinical Pearl:** The increasing frequency of squatting over the past week suggests worsening disease and impending spells. This is a sign that surgery should not be delayed. ## Do NOT Do - ~~Furosemide~~ — worsens dehydration and increases blood viscosity, making shunt worse - ~~Head-up positioning~~ — decreases systemic vascular resistance, worsens shunt - ~~Balloon atrial septostomy~~ — not indicated in TOF; used for TGA - ~~Immediate intubation~~ — only if medical measures fail; avoid if possible 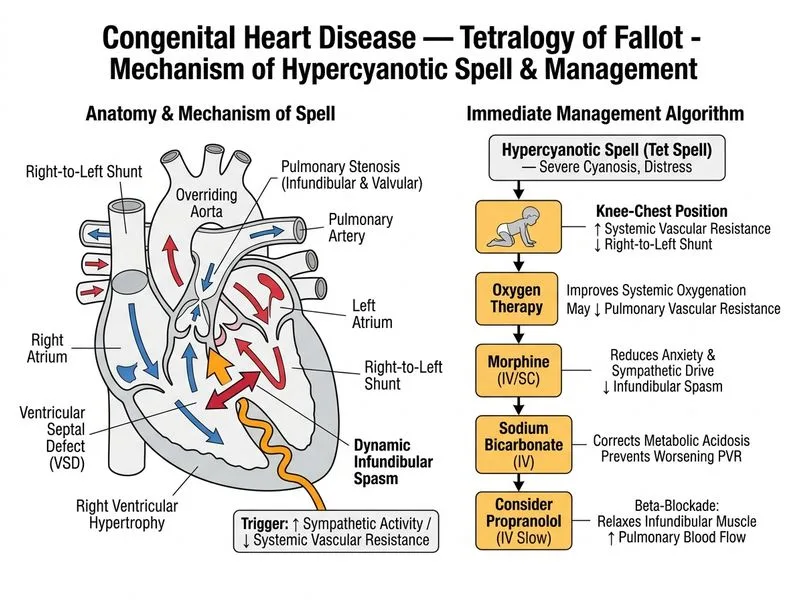
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.