## Clinical Presentation & Diagnosis **Key Point:** This patient presents with acute kidney injury (AKI) developing 3 days post-contrast administration, characterized by rising creatinine, oliguria, and muddy brown casts in the urine—pathognomonic for contrast-induced nephropathy (CIN). ## Pathophysiology of Contrast-Induced Nephropathy **High-Yield:** CIN is the third leading cause of hospital-acquired acute kidney injury. It occurs through two mechanisms: 1. **Direct tubular toxicity:** - Contrast media are hyperosmolar and directly damage proximal tubular epithelium - Causes acute tubular necrosis (ATN) → muddy brown casts in urine 2. **Renal vasoconstriction:** - Initial vasodilation followed by prolonged vasoconstriction - Reduces glomerular filtration rate (GFR) - Mediated by adenosine, endothelin, and prostaglandins ## Risk Factors for CIN | High-Risk Category | Specific Risk Factors | |---|---| | **Renal** | eGFR < 30 mL/min, diabetes mellitus, proteinuria | | **Metabolic** | Diabetes mellitus (especially uncontrolled), dehydration | | **Cardiac** | Heart failure, cardiogenic shock, hypotension | | **Medication** | ACE inhibitors/ARBs, NSAIDs, diuretics | | **Contrast-related** | High osmolality (HOCM > LOCM > IOCM), large volume | **Clinical Pearl:** This patient has **multiple risk factors**: eGFR 32 (stage 3b CKD), diabetes (HbA1c 8.2%), age > 70, and was on an ACE inhibitor. She is at very high risk for CIN. ## Prevention of Contrast-Induced Nephropathy ```mermaid flowchart TD A[Patient requiring contrast]:::outcome --> B{Risk assessment}:::decision B -->|Low risk| C[Standard precautions]:::action B -->|High risk: eGFR < 60 or DM| D[Aggressive hydration]:::action D --> E[IV isotonic saline 1-1.5 L/hr]:::action E --> F[Start 4-12 hrs before, continue 4-6 hrs after]:::action B -->|Very high risk: eGFR < 30| G[Consider alternative imaging]:::urgent G --> H[MRI without gadolinium, ultrasound, non-contrast CT]:::action D --> I[Use LOCM or IOCM]:::action I --> J[Minimize contrast volume]:::action J --> K[Avoid nephrotoxic drugs]:::action ``` ## Evidence-Based Prevention Strategies | Strategy | Evidence Level | Details | |---|---|---| | **IV isotonic saline** | Gold standard | 0.9% NaCl at 1–1.5 mL/kg/hr for 4–12 hrs before and 4–6 hrs after | | **Oral hydration** | Inferior to IV | Can be used in low-risk patients with normal renal function | | **LOCM/IOCM** | Standard | Non-ionic, low-osmolality agents reduce CIN risk vs. HOCM | | **Minimize volume** | Essential | Contrast volume ≤ eGFR ratio (e.g., if eGFR = 30, use ≤ 30 mL) | | **Avoid NSAIDs** | Critical | Discontinue 48 hrs before and after contrast | | **ACE-I/ARB** | Controversial | Some guidelines recommend holding; others allow continuation with hydration | | **Metformin** | Conditional | Hold for 48 hrs post-contrast if CIN develops (risk of lactic acidosis) | | **N-acetylcysteine** | Not recommended | No proven benefit in recent trials | | **Theophylline** | Not recommended | No proven benefit | **Key Point:** Intravenous isotonic saline hydration is the **most effective and evidence-based** intervention for preventing CIN. It should be started 4–12 hours before contrast administration and continued for 4–6 hours after. **Mnemonic: CONTRAST Prevention (High-Risk Patients)** - **C**hoose LOCM/IOCM (avoid HOCM) - **O**ptimize hydration (IV saline 1–1.5 mL/kg/hr) - **N**ephrotoxic drugs: avoid NSAIDs, minimize ACE-I/ARB - **T**ime: start hydration 4–12 hrs before - **R**educe contrast volume (≤ eGFR) - **A**ssess renal function (baseline Cr, eGFR) - **S**ubstitute alternative imaging if eGFR < 30 - **T**herapy: monitor Cr at 48–72 hrs post-contrast ## Why This Patient Developed CIN This patient had **multiple preventable risk factors** and likely did not receive adequate prehydration: - eGFR 32 (stage 3b CKD) - Uncontrolled diabetes (HbA1c 8.2%) - Age 72 years - On ACE inhibitor (lisinopril) - Received 80 mL of contrast (may exceed safe volume) ## Clinical Outcome & Management **High-Yield:** Most cases of CIN are self-limited and resolve within 5–7 days with supportive care: - Discontinue nephrotoxic drugs (NSAIDs, ACE-I/ARB if possible) - Continue IV hydration - Monitor renal function daily - Avoid repeat contrast for 48–72 hours if possible - Consider renal replacement therapy if oliguria or hyperkalemia develops [cite:Harrison 21e Ch 297; Robbins 10e Ch 3] 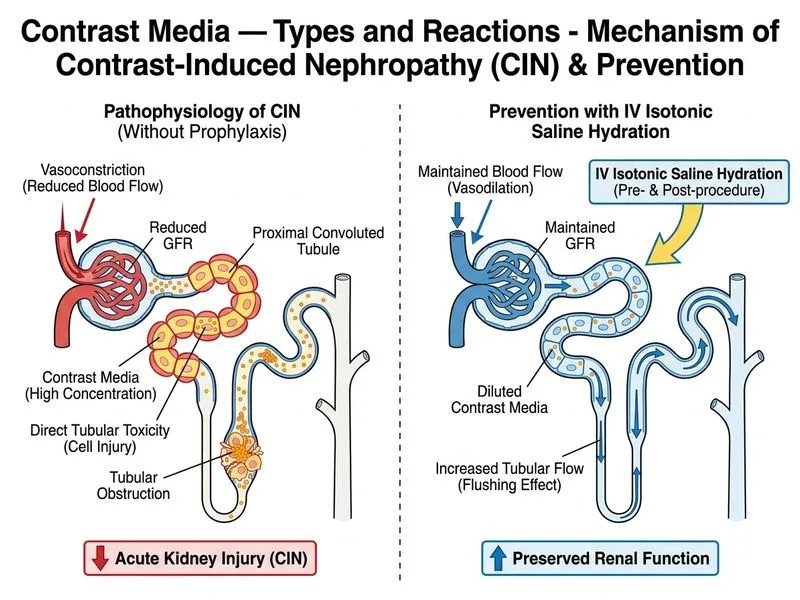
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.