## Gadolinium vs Iodinated Contrast: Renal Safety Discrimination ### Clinical Context: CKD and Contrast Selection In a patient with **eGFR 35 mL/min/1.73m²** (Stage 3b CKD), both contrast types carry renal risk, but via **different mechanisms and thresholds**. This is a critical discriminator for exam and practice. ### Comparison Table | Feature | Gadolinium-Based Contrast (GBCA) | Iodinated Contrast Media | | --- | --- | --- | | **Primary Renal Toxicity** | Nephrogenic Systemic Fibrosis (NSF) | Contrast-Induced Nephropathy (CIN) | | **Risk Threshold** | eGFR <30 mL/min/1.73m² (especially <15) | eGFR <30 mL/min/1.73m² (risk increases <15) | | **Mechanism** | Gadolinium dissociation → free Gd³⁺ → fibroblast activation → systemic fibrosis | Osmotic diuresis → medullary hypoxia; direct tubular epithelial toxicity | | **Reversibility** | NSF is **irreversible** | CIN may recover if renal function preserved | | **Incidence (eGFR <30)** | 1–7% with linear GBCA; <0.1% with macrocyclic GBCA | 10–30% (higher with volume depletion, diabetes) | | **Modality** | MRI | CT, angiography, IVP | | **Preventive Strategy** | Avoid linear GBCA; use macrocyclic or avoid GBCA <30; dialyze if possible | Hydration, N-acetylcysteine (controversial), minimize volume | ### Pathophysiology: Why Each Contrast Causes Different Injury **Gadolinium (GBCA):** 1. Gadolinium is a lanthanide chelated to prevent toxicity 2. In acidic, protein-rich environment (plasma, tissue), **chelate dissociates** → free Gd³⁺ 3. Free gadolinium deposits in skin, bone, brain → **fibroblast activation** → systemic fibrosis (NSF) 4. Risk is **highest with linear chelates** (less stable); **macrocyclic chelates** (more stable) have lower NSF risk 5. Renal excretion is impaired when eGFR <30, prolonging tissue exposure **Iodinated Contrast:** 1. Hyperosmolar (HOCM) or iso-osmolar (IOCM) solutions 2. Osmotic diuresis → volume depletion of renal medulla 3. Medullary hypoxia + direct tubular epithelial toxicity 4. Risk increases with **dehydration, diabetes, eGFR <30**, and **large contrast volumes** 5. CIN typically peaks 48–72 hours post-injection; may recover ### High-Yield: Renal Thresholds **Key Point:** - **eGFR 30–60:** Both GBCA and iodinated contrast carry risk; use with caution and hydration. - **eGFR <30:** GBCA is contraindicated (NSF risk); iodinated contrast can be used with aggressive hydration, but CIN risk is substantial. - **eGFR <15:** Both are high-risk; consider alternative imaging or dialysis post-procedure. ### Clinical Pearl **Warning:** NSF is **irreversible and progressive**. Once gadolinium deposits in tissue (especially with linear GBCA in eGFR <30), fibrosis develops over weeks to months and can be disabling (skin hardening, joint stiffness, organ fibrosis). This is why **linear GBCA is now contraindicated in eGFR <30**; macrocyclic GBCA is preferred if GBCA is essential. In contrast, **CIN is often reversible** if renal function is preserved and hydration is maintained. ### Mnemonic **NSF = No Safe Gadolinium (in CKD)**; **CIN = Contrast-Induced Nephropathy (osmotic injury)**. 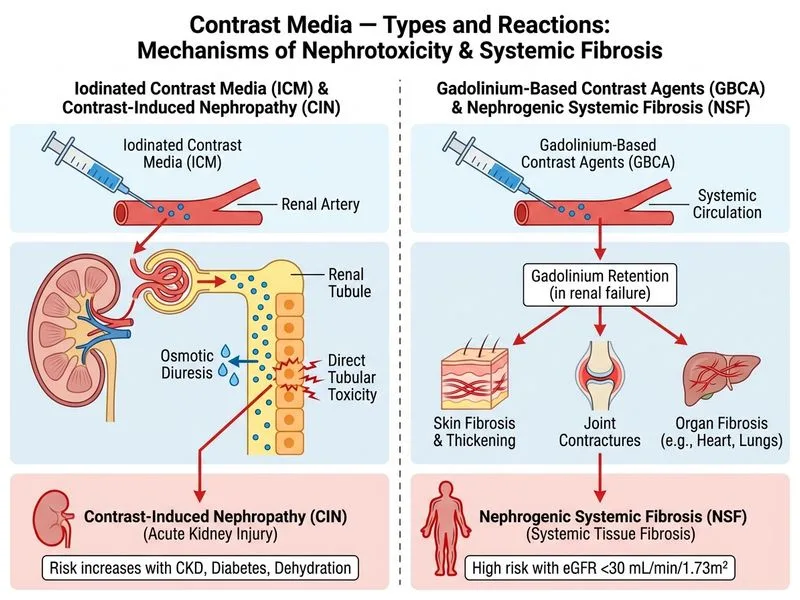
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.