## Clinical Context This patient has multiple risk factors for contrast-induced nephropathy (CIN) and contrast hypersensitivity: - Chronic kidney disease (eGFR 42) - Diabetes mellitus on metformin - Prior contrast reaction (urticaria) ## Contrast Agent Selection **Key Point:** Low-osmolar contrast media (LOCM) or iso-osmolar contrast media (IOCM) are preferred over high-osmolar contrast media (HOCM) in patients with renal impairment. LOCM has osmolality 600–800 mOsm/kg; HOCM >1200 mOsm/kg. **High-Yield:** In patients with prior non-anaphylactic contrast reaction, LOCM with pre-medication is the standard approach. Pre-medication reduces repeat reaction risk from ~17% (no pre-med) to ~1–2% (with pre-med). ## Pre-Medication Protocol for Prior Contrast Reaction | Element | Rationale | |---------|----------| | Corticosteroid (e.g., methylprednisolone 32 mg IV 12 & 2 hrs before contrast) | Reduces mast cell degranulation; reduces repeat reaction risk | | Antihistamine (e.g., diphenhydramine 50 mg IV 1 hr before contrast) | Blocks H1 and H2 receptors; synergistic with corticosteroid | | LOCM (not IOCM) | LOCM is more cost-effective and equally safe in this setting; IOCM reserved for severe renal disease or multiple risk factors | ## Metformin Management **Clinical Pearl:** Metformin must be held at the time of contrast administration and for 48 hours post-procedure (or until renal function confirmed stable) due to risk of lactic acidosis if contrast-induced acute kidney injury occurs. **Warning:** Continuing metformin through contrast administration is a common error and increases risk of metformin-associated lactic acidosis (MALA). ## Why This Answer - LOCM is the standard contrast agent for renal impairment and prior reaction - Dual pre-medication (corticosteroid + antihistamine) is guideline-recommended for prior non-anaphylactic reaction - Metformin discontinuation is mandatory pre-procedure [cite:Harrison 21e Ch 297] 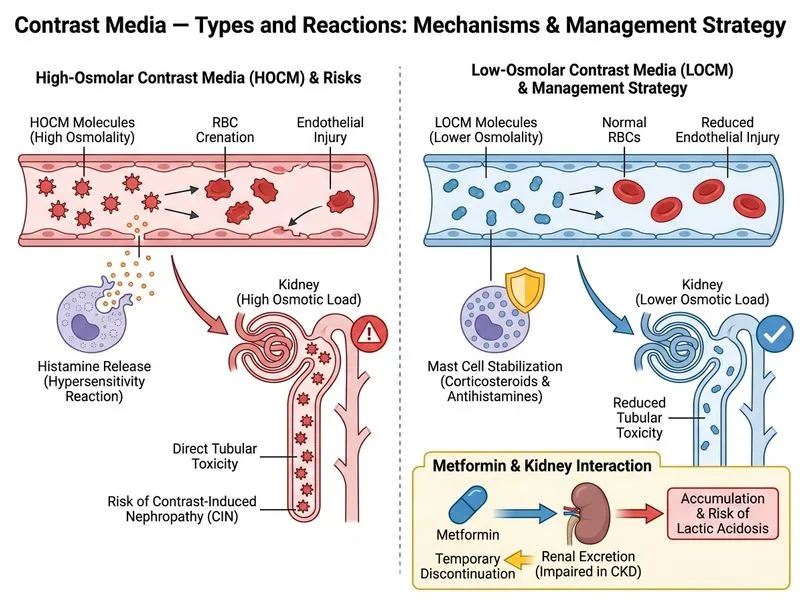
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.