## Contrast-Induced Acute Kidney Injury (CI-AKI) ### Pathophysiology **Key Point:** CI-AKI is a non-allergic, dose-dependent complication occurring within 24–72 hours of contrast administration, characterized by a rise in serum creatinine ≥0.5 mg/dL or ≥25% from baseline. The mechanism involves two primary pathways: 1. **Direct tubular toxicity**: Contrast medium accumulates in proximal tubular cells, causing osmotic stress and generation of reactive oxygen species (ROS). 2. **Renal hemodynamic compromise**: Initial vasodilation followed by sustained vasoconstriction, reducing renal blood flow and glomerular filtration rate (GFR). ### Risk Factors in This Case - **Pre-existing chronic kidney disease** (eGFR 32) — the single strongest risk factor - **Non-ionic, low-osmolality contrast** (iopamidol) — lower risk than high-osmolality agents, but still carries risk in advanced CKD - **Acute presentation** (oliguria, muddy brown casts) — consistent with acute tubular necrosis (ATN) pattern ### Clinical Features of CI-AKI | Feature | Details | |---------|----------| | **Onset** | 24–72 hours post-contrast | | **Peak creatinine** | 3–5 days | | **Urinalysis** | Muddy brown casts, proteinuria, granular casts (ATN pattern) | | **Oliguria** | Present in severe cases | | **Recovery** | Usually within 7–14 days if no permanent renal damage | **High-Yield:** The muddy brown casts are pathognomonic for acute tubular necrosis, confirming intrinsic renal injury rather than prerenal or allergic causes. ### Prevention and Management 1. **Hydration**: IV normal saline (0.9%) — 1 mL/kg/hr for 12 hours before and after contrast 2. **Contrast volume**: Keep osmolar load <3 mL per 1 mL of serum creatinine 3. **Metformin**: Hold for 48 hours post-contrast (risk of lactic acidosis if renal function deteriorates) 4. **Monitoring**: Serum creatinine at 48–72 hours post-procedure **Clinical Pearl:** In patients with eGFR <30, consider alternative imaging (ultrasound, MRI without gadolinium) or use of iso-osmolar contrast media (IOCM) if contrast is essential. ### Why Non-Ionic, Low-Osmolality Contrast? Although iopamidol is a safer choice than high-osmolality contrast (HOCM), it does NOT eliminate CI-AKI risk in advanced CKD. The osmolality gradient still drives fluid shifts and tubular damage. [cite:Harrison 21e Ch 279] ## Differential Diagnosis Ruled Out **Allergic interstitial nephritis** (Option 1): Would present with fever, rash, eosinophilia, and eosinophiluria — NOT muddy brown casts. Onset is typically 1–3 weeks, not 2 hours. **Acute glomerulonephritis** (Option 2): Would show RBC casts, dysmorphic RBCs, and active urinary sediment. No mention of hematuria or hypertension in this vignette. **Prerenal azotemia** (Option 3): Would improve with fluid resuscitation; CI-AKI is intrinsic renal injury and does not respond to fluids alone. 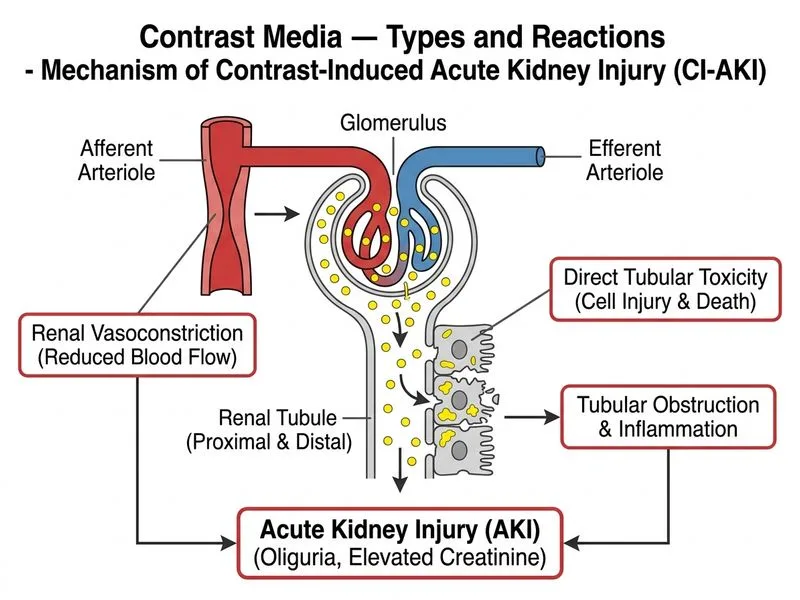
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.