## Contrast Media Selection in Severe Renal Impairment **Key Point:** In patients with severe renal dysfunction (eGFR <30 mL/min/1.73m²), both **low-osmolar contrast media (LOCM)** and **iso-osmolar contrast media (IOCM)** are acceptable choices; however, **LOCM (e.g., iopamidol)** is the most widely recommended first-line agent in clinical practice due to its superior evidence base, widespread availability, and cost-effectiveness. ### Osmolality and Nephrotoxicity Risk | Contrast Type | Osmolality (mOsm/kg) | Nephrotoxicity Risk | Use in CKD | |---|---|---|---| | HOCM (ionic) | 1,400–1,900 | **High** | **Avoid** | | LOCM (non-ionic) | 600–850 | **Low** | **First-line preferred** | | IOCM (non-ionic) | ~290 | **Very Low** | Acceptable (second-line) | | GBCA | N/A (MRI only) | Risk of NSF | **Contraindicated** in eGFR <30 | ### Why LOCM Over IOCM? While IOCM (iodixanol, osmolality ~290 mOsm/kg) has the theoretical advantage of being iso-osmolar with plasma, **multiple randomized controlled trials and meta-analyses (including NEPHRIC trial re-analyses) have not demonstrated a consistent, clinically significant superiority of IOCM over LOCM** in preventing contrast-induced acute kidney injury (CI-AKI) when modern non-ionic LOCM agents (iopamidol, iohexol, ioversol) are used: 1. **Evidence base:** ACR Manual on Contrast Media (2023) and European Society of Urogenital Radiology (ESUR) guidelines list LOCM as the **standard of care** for patients with CKD undergoing CT; IOCM is listed as an alternative. 2. **Cost and availability:** LOCM agents are significantly less expensive and universally available in most radiology departments. 3. **Practical guideline alignment:** Most institutional protocols default to LOCM for CT contrast in CKD; IOCM is reserved for specific high-risk scenarios (e.g., intra-arterial injection with pre-existing severe CKD). **High-Yield:** The key distinction is that **HOCM must be avoided** in CKD (high nephrotoxicity), **GBCA is contraindicated** (NSF risk), and between LOCM and IOCM, **LOCM is the standard first-line CT contrast agent** per ACR/ESUR guidelines. ### Pathophysiology of Contrast-Induced AKI 1. **Osmotic diuresis** → renal medullary hypoxia 2. **Direct tubular toxicity** from high osmolality 3. **Vasoconstriction** → reduced renal perfusion 4. **Oxidative stress** → tubular injury HOCM agents (osmolality >1,400 mOsm/kg) exacerbate all four mechanisms; LOCM agents significantly reduce risk. **Clinical Pearl:** Even with LOCM, **IV hydration with 0.9% saline** (1–1.5 mL/kg/hr for 3–4 hours pre- and 4–6 hours post-procedure) and **renal function monitoring at 48–72 hours** post-contrast are mandatory in this patient (eGFR 18 mL/min/1.73m²). **Warning:** Gadolinium-based contrast agents are **contraindicated** in eGFR <30 mL/min/1.73m² due to the risk of **nephrogenic systemic fibrosis (NSF)**. Additionally, gadolinium is an MRI contrast agent — it has no role in CT imaging. ### Mnemonic: "LOCM First in CKD-CT" - **L**ow-osmolar, **N**on-ionic = **First-line for CT in CKD** - **I**OCM = Acceptable alternative (not superior in CT) - **H**OCM = **H**azardous — avoid - **G**BCA = **G**one (contraindicated in severe CKD) *(References: ACR Manual on Contrast Media v2023; ESUR Guidelines on Contrast Agents v10.0; KD Tripathi Essentials of Medical Pharmacology, 8th ed.)* 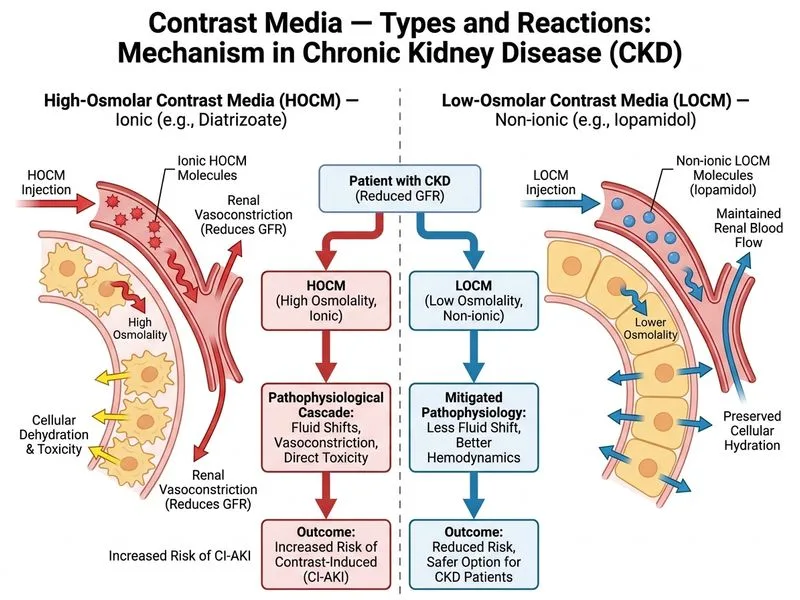
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.