## Contrast-Induced Nephropathy (CIN): Mechanism and Pathophysiology **Key Point:** CIN is a non-allergic, osmotic and ischemic injury to the renal tubules, not an immune-mediated reaction. It occurs within 24–72 hours of contrast exposure and is reversible in most cases. ### Pathophysiologic Mechanism of CIN ```mermaid flowchart TD A[Iodinated Contrast Administration]:::action --> B[Osmotic Load in Renal Tubules]:::outcome B --> C[Fluid Shift into Tubular Lumen]:::outcome C --> D[Renal Medullary Hypoxia]:::outcome A --> E[Renal Vasoconstriction<br/>Adenosine + Endothelin Release]:::outcome E --> D D --> F[Tubular Epithelial Cell Injury]:::urgent F --> G[Acute Kidney Injury<br/>Reversible in 5-7 days]:::outcome ``` ### Two-Hit Mechanism **High-Yield:** CIN results from a **two-hit mechanism**: 1. **Osmotic toxicity:** High osmolality of contrast media (especially HOCM) causes: - Osmotic diuresis and intratubular fluid shift - Increased tubular fluid viscosity - Tubular obstruction and back-leak of filtrate 2. **Renal ischemia:** Contrast-induced vasoconstriction causes: - Initial renal vasodilation (mediated by prostaglandins and nitric oxide) - Followed by prolonged vasoconstriction (mediated by adenosine, endothelin, and angiotensin II) - Medullary hypoxia and oxidative stress - Release of reactive oxygen species (ROS) **Clinical Pearl:** CIN is characterized by: - Serum creatinine rise ≥0.5 mg/dL or ≥25% within 48–72 hours of contrast exposure - Usually reversible within 5–7 days (unlike allergic reactions which are immediate) - More common in patients with pre-existing renal disease, diabetes, dehydration, and advanced age ### Risk Factors for CIN | High-Risk Factors | Mechanism | |---|---| | Pre-existing renal disease (eGFR <30) | Reduced renal reserve; impaired autoregulation | | Diabetes mellitus | Endothelial dysfunction; impaired vasodilation | | Dehydration / volume depletion | Reduced renal perfusion; increased contrast concentration | | Advanced age (>70 years) | Reduced GFR; impaired renal autoregulation | | Congestive heart failure | Reduced renal perfusion | | Nephrotoxic drugs (NSAIDs, ACE-I) | Impaired renal hemodynamics | **Mnemonic:** **CIN = Osmotic + Ischemic** — remember the two-hit mechanism: osmolality causes tubular damage, and vasoconstriction causes medullary hypoxia. ### Prevention Strategies 1. **Volume expansion:** IV hydration with normal saline (most effective preventive measure) 2. **Use LOCM/IOCM agents:** Lower osmolality reduces osmotic injury 3. **Minimize contrast volume:** Dose ≤5 mL/kg body weight 4. **Hold nephrotoxic drugs:** Discontinue NSAIDs, ACE inhibitors, metformin 48 hours before and after contrast 5. **Avoid repeat contrast:** Space procedures ≥48 hours apart if possible **Warning:** Do not confuse CIN with allergic contrast reactions — they have different mechanisms, timelines, and management. Allergic reactions occur within minutes; CIN develops over 24–72 hours. 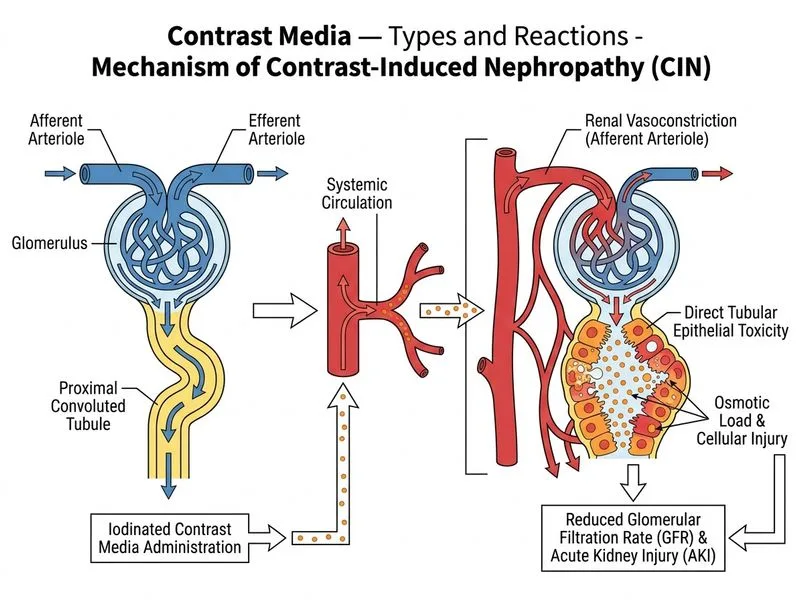
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.