## Diagnosis: Contrast-Induced Acute Kidney Injury (CI-AKI) ### Clinical Presentation The patient presents with the classic temporal and clinical profile of CI-AKI: - **Timing:** Serum creatinine elevation within 6 hours of contrast administration (peak at 48–72 hours) - **Magnitude:** Rise of ≥0.5 mg/dL or ≥25% from baseline - **Preserved urine output:** Rules out severe prerenal or obstructive causes ### Risk Factors Present | Risk Factor | Status | | --- | --- | | Diabetes mellitus | Present (type 2) | | Chronic kidney disease | Present (eGFR 35) | | Contrast volume | 80 mL (moderate) | | Contrast osmolality | Low-osmolar (better than high-osmolar, but still risk) | | Age | 58 years (moderate) | **Key Point:** CI-AKI is defined as an acute rise in serum creatinine (≥0.5 mg/dL absolute or ≥25% relative increase) occurring within 48 hours of intravascular contrast administration, without alternative explanation. ### Pathophysiology 1. **Direct tubular toxicity:** Contrast media are hyperosmolar and directly injure proximal tubular epithelium 2. **Renal vasoconstriction:** Initial vasodilation followed by sustained vasoconstriction reduces glomerular filtration rate 3. **Oxidative stress:** Generation of reactive oxygen species in the renal medulla 4. **Viscosity effect:** Increased blood viscosity impairs renal perfusion **High-Yield:** Patients with pre-existing renal impairment (eGFR <60) and diabetes are at highest risk; CI-AKI incidence rises to 10–15% in this population. ### Prevention Strategies - **Hydration:** Isotonic saline 1 mL/kg/hr for 12 hours before and after procedure (most effective) - **Contrast selection:** Non-ionic, low-osmolar agents preferred over ionic, high-osmolar agents - **Volume minimization:** Use lowest volume necessary (contrast volume ÷ eGFR ratio <3.7) - **Drug optimization:** Consider metformin hold (lactic acidosis risk if renal failure develops); N-acetylcysteine (controversial but often used) **Clinical Pearl:** Adequate hydration reduces CI-AKI risk by ~50% in high-risk patients; it is the single most important preventive measure. **Mnemonic — Risk Stratification (ABCDE):** - **A** — Age >70 - **B** — Baseline renal dysfunction (eGFR <60) - **C** — Contrast volume >5 mL/kg - **D** — Diabetes mellitus - **E** — Ejection fraction <40% (heart failure) ### Management - **Supportive care:** Maintain hydration, monitor urine output and electrolytes - **Nephrology consultation:** If creatinine continues to rise or oliguria develops - **Avoid further nephrotoxins:** NSAIDs, ACE inhibitors (temporarily), aminoglycosides - **Prognosis:** Most cases resolve within 5–7 days; dialysis required in <1% of CI-AKI cases **Warning:** Do not confuse CI-AKI with acute tubular necrosis (ATN) from sepsis — ATN typically shows muddy brown casts, fractional excretion of sodium >2%, and is not temporally linked to contrast administration. 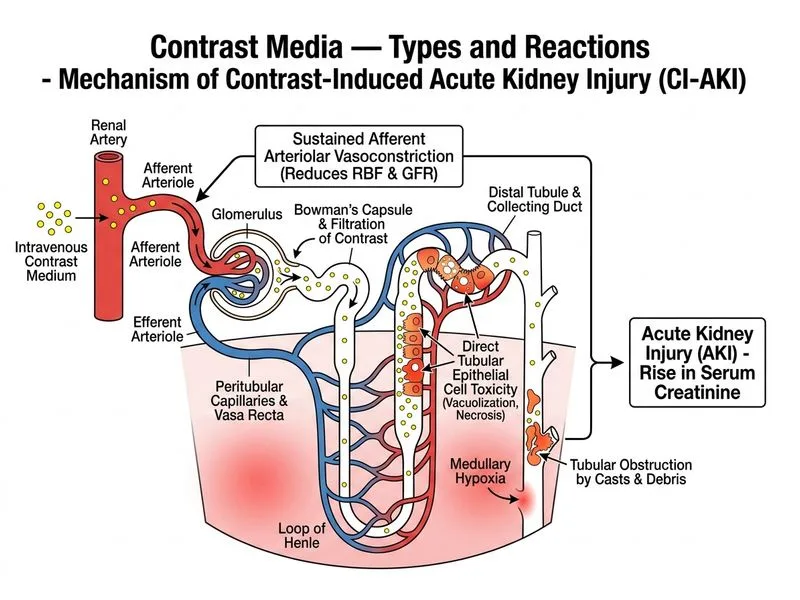
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.