## Management of Acute Gadolinium Contrast Reaction ### Classification of Contrast Reactions | Reaction Type | Onset | Severity | Mechanism | Examples | | --- | --- | --- | --- | --- | | **Mild** | 1–20 min | Localized | Non-IgE mediated | Flushing, nausea, urticaria (localized) | | **Moderate** | 1–20 min | Systemic but stable | IgE-mediated or complement | Urticaria (generalized), mild bronchospasm, angioedema | | **Severe** | Seconds to min | Life-threatening | IgE-mediated anaphylaxis | Anaphylaxis, severe bronchospasm, hypotension, laryngeal edema | ### Case Classification: **Moderate Anaphylactoid Reaction** This patient exhibits: - **Urticaria** (generalized) - **Angioedema** (facial edema) - **Bronchospasm** (mild, SpO₂ still 94%) - **Hemodynamic stability** (BP 115/70) - **Rapid onset** (within 2 minutes of contrast injection) **Key Point:** Any combination of urticaria + angioedema + respiratory symptoms = **moderate-to-severe reaction requiring epinephrine**, regardless of hemodynamic stability. Do not wait for hypotension to develop. ### Immediate Management Algorithm ```mermaid flowchart TD A[Contrast reaction suspected]:::outcome --> B{Severity assessment}:::decision B -->|Mild: urticaria only| C[Observe, antihistamines]:::action B -->|Moderate: urticaria + angioedema ± bronchospasm| D[IM epinephrine 0.3 mg]:::urgent B -->|Severe: anaphylaxis, hypotension, stridor| E[IM epinephrine 0.3 mg immediately]:::urgent D --> F[Establish IV access]:::action E --> F F --> G[IV antihistamines + corticosteroids]:::action G --> H[Observe 4-6 hours]:::action H --> I[Discharge with EpiPen, allergy referral]:::outcome ``` **High-Yield:** Epinephrine is the first-line agent for moderate-to-severe reactions. Antihistamines and corticosteroids are **adjunctive**, not primary therapy. Delaying epinephrine in moderate reactions increases risk of biphasic anaphylaxis (10–15% of cases). ### Epinephrine Dosing and Administration **Intramuscular (preferred in acute setting):** - **Dose:** 0.3–0.5 mg of 1:1000 solution (0.3–0.5 mL) - **Site:** Anterolateral thigh (faster absorption than arm) - **Onset:** 5–15 minutes - **Repeat:** Every 5–15 minutes if symptoms persist or recur **Intravenous (only if IV access already established and patient in shock):** - **Dose:** 0.1 mg of 1:10,000 solution IV slowly over 5–10 minutes - **Risk:** Arrhythmias, myocardial infarction if given too rapidly **Clinical Pearl:** IM epinephrine is safer and more effective than IV in the acute setting because it avoids the risk of rapid IV bolus complications and provides sustained absorption from muscle depot. ### Adjunctive Medications (After Epinephrine) | Agent | Dose | Rationale | | --- | --- | --- | | **Antihistamine (H1-blocker)** | Diphenhydramine 25–50 mg IV/IM | Blocks histamine-mediated symptoms; slower onset than epinephrine | | **Antihistamine (H2-blocker)** | Famotidine 20 mg IV | Synergistic with H1-blocker; reduces gastric acid | | **Corticosteroid** | Methylprednisolone 125 mg IV or hydrocortisone 100 mg IV | Prevents biphasic reaction; takes 4–6 hours to work | | **Beta-2 agonist** | Albuterol nebulized | For persistent bronchospasm | **Mnemonic — Post-Epinephrine Management (ABC):** - **A** — Antihistamines (H1 + H2 blockers) - **B** — Beta-2 agonists (if bronchospasm persists) - **C** — Corticosteroids (IV preferred) ### Risk Factors for Contrast Reactions **Major risk factors in this patient:** - **Shellfish allergy** (associated with gadolinium reactions; cross-reactivity with iodine-based contrast) - **Asthma** (increases risk of bronchospasm) - **Female sex** (2× higher risk than males) - **Age 40–50** (peak incidence) **Warning:** Do NOT confuse gadolinium reactions with iodine-based contrast reactions. Gadolinium is used in MRI and has a lower overall reaction rate (~0.1%) than iodine-based contrast (~0.4%), but reactions are equally severe when they occur. ### Prevention for Future Procedures 1. **Premedication regimen (if contrast essential):** - Methylprednisolone 32 mg PO 12 and 2 hours before procedure - Diphenhydramine 50 mg PO 1 hour before procedure - Ranitidine 150 mg PO 1 hour before procedure 2. **Alternative imaging:** Consider non-contrast MRI sequences or CT without contrast if feasible 3. **Allergy referral:** Skin testing and graded challenge testing may identify safe alternatives **High-Yield:** Premedication reduces reaction risk by ~50% but does NOT eliminate it; always have epinephrine available. 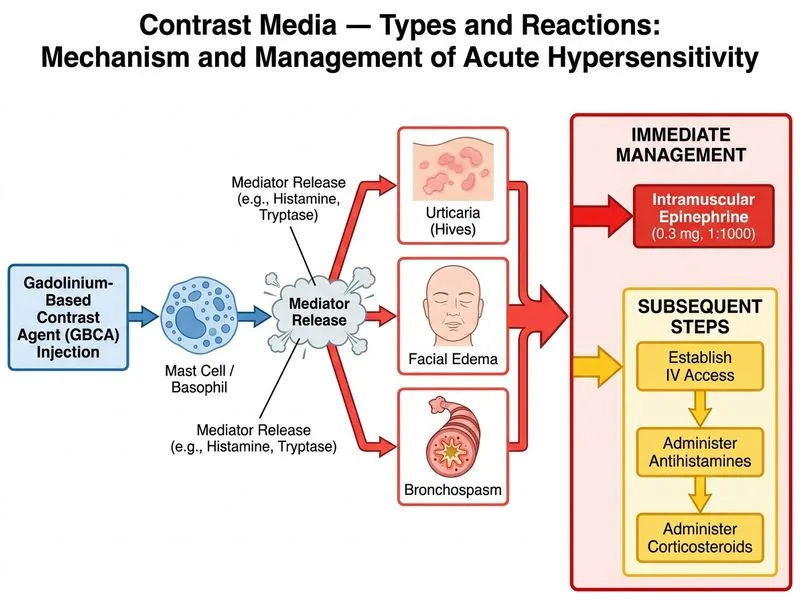
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.