## Risk Assessment and Management of Contrast Reactions in Atopic Patients ### Clinical Context This patient has a history of anaphylaxis (shellfish allergy), which increases the risk of contrast reaction. The question asks for the appropriate investigation/approach to assess risk and guide contrast choice. ### Why Clinical History and Risk Stratification is Optimal **Key Point:** There is NO reliable in vivo or in vitro test that can predict contrast reaction in individual patients. Management relies on: 1. Detailed allergy history and risk stratification 2. Selection of appropriate contrast type (low-osmolar or iso-osmolar) 3. Premedication protocols for high-risk patients 4. Consideration of non-contrast alternatives **High-Yield:** Contrast reaction risk factors include: - Prior contrast reaction (strongest predictor) - Atopy (asthma, eczema, allergic rhinitis) - Food/drug allergies (shellfish, NSAIDs) - Renal impairment - Diabetes mellitus - Dehydration **Warning:** The myth that "shellfish allergy = iodine allergy" is INCORRECT. Shellfish allergy is to tropomyosin protein, NOT iodine. However, patients with atopy (including shellfish allergy) have a 2–3× higher risk of contrast reaction independent of iodine content. ### Management Algorithm for High-Risk Patients ```mermaid flowchart TD A[Patient with atopy/prior reaction]:::outcome --> B{Contrast study essential?}:::decision B -->|No| C[Use non-contrast imaging or alternative modality]:::action B -->|Yes| D[Use low-osmolar or iso-osmolar contrast]:::action D --> E[Premedicate: Corticosteroid + Antihistamine]:::action E --> F[Consider H2-blocker]:::action F --> G[Administer contrast with monitoring]:::action G --> H[Observe for 30 min post-procedure]:::action H --> I[Document reaction type if occurs]:::outcome ``` ### Why Each Test is Inappropriate | Test | Why Inappropriate | |------|-------------------| | **Skin prick test** | Not standardized; poor predictive value; risk of anaphylaxis during testing | | **Serum tryptase** | Baseline tryptase does not predict contrast reaction; only elevated acutely during/after anaphylaxis | | **Intradermal test** | Dangerous in atopic patients; risk of systemic reaction; poor sensitivity/specificity | **Clinical Pearl:** Premedication with corticosteroids (e.g., methylprednisolone 32 mg PO 12 and 2 hrs before contrast) + antihistamine (diphenhydramine 50 mg) reduces contrast reaction risk by ~50% in high-risk patients. ### Contrast Agent Selection **High-Yield:** For atopic patients: - **Preferred:** Low-osmolar contrast (LOCM, osmolality 600–800 mOsm/kg) or iso-osmolar contrast (IOCM, 290 mOsm/kg) - **Avoid:** High-osmolar contrast (HOCM, >1200 mOsm/kg) — higher reaction rates - **Note:** Osmolarity, not iodine content, is the main driver of contrast reactions [cite:Harrison 21e Ch 281; Robbins 10e Ch 20] 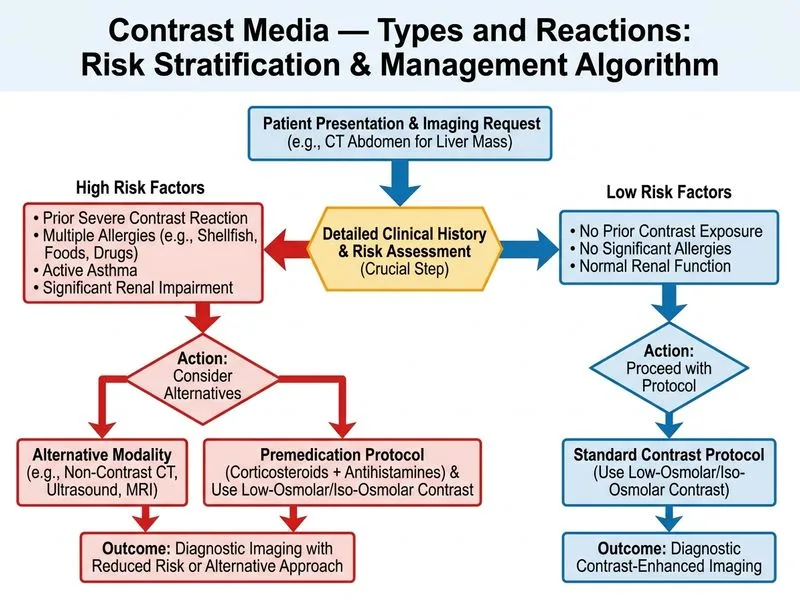
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.