## Management of Acute Anaphylactic Contrast Reaction ### Clinical Recognition This patient is experiencing **acute anaphylaxis** (not a mild allergic reaction) triggered by contrast medium. Key diagnostic features: - **Rapid onset**: Within 3 minutes of IV contrast (immediate hypersensitivity) - **Systemic symptoms**: Dyspnea, angioedema, urticaria - **Hemodynamic instability**: Hypotension (95/60), tachycardia (118/min) - **Risk factor**: Shellfish allergy (cross-reactivity with iodine-containing contrast) ### Immediate Management Algorithm ```mermaid flowchart TD A[Acute contrast reaction]:::outcome --> B{Severity?}:::decision B -->|Mild: urticaria, pruritus| C[Observe, antihistamine]:::action B -->|Moderate: dyspnea, angioedema| D[Stop contrast, IV access, antihistamine + corticosteroid]:::action B -->|Severe: anaphylaxis with hypotension| E[STOP contrast immediately]:::urgent E --> F[IM Epinephrine 0.3-0.5 mg 1:1000]:::urgent F --> G[IV access, fluids, elevate legs]:::action G --> H[Prepare airway, monitor vitals]:::action H --> I[Consider H1/H2 blockers + corticosteroids]:::action I --> J[Admit, observe 4-6 hours minimum]:::outcome ``` **Key Point:** Anaphylaxis is a **medical emergency** requiring immediate epinephrine. Delay in administration increases mortality risk. ### Epinephrine Administration **High-Yield:** Epinephrine is the ONLY first-line drug for anaphylaxis. It must be given **intramuscularly** (IM) in the anterolateral thigh, NOT IV (unless cardiac arrest). | Parameter | Details | |---|---| | **Drug** | Epinephrine (adrenaline) 1:1000 aqueous solution | | **Dose** | 0.3–0.5 mg IM (0.3–0.5 mL of 1:1000) | | **Route** | Intramuscular (anterolateral thigh) — fastest absorption | | **Timing** | Immediately, do not delay for IV access | | **Repeat** | Every 5–15 minutes if symptoms persist | | **Mechanism** | α-adrenergic (vasoconstriction) + β-adrenergic (bronchodilation, ↑ HR, ↑ contractility) | ### Supportive Measures (After Epinephrine) 1. **IV access**: Establish large-bore IV (18G or larger) for fluid resuscitation. 2. **Fluids**: Normal saline 500 mL rapid bolus; repeat as needed for hypotension. 3. **Positioning**: Elevate lower extremities (Trendelenburg) to maintain cerebral perfusion. 4. **Airway**: Prepare for intubation; have suction, airway adjuncts, and emergency medications ready. 5. **Monitoring**: Continuous pulse oximetry, BP, ECG. 6. **Adjunctive agents** (after epinephrine): - H1 blocker: IV diphenhydramine 50 mg or IV cetirizine 10 mg - H2 blocker: IV ranitidine 50 mg (optional) - Corticosteroid: IV methylprednisolone 125 mg or IV dexamethasone 10 mg (prevents biphasic reaction) **Clinical Pearl:** Do NOT substitute antihistamines or corticosteroids for epinephrine. These agents are **adjunctive only** and have no role in acute anaphylaxis management without epinephrine. ### Why Not the Other Options? - **Option 1 (Antihistamine alone)**: Diphenhydramine is a **second-line** agent for mild–moderate reactions. In anaphylaxis with hemodynamic instability, it is ineffective and delays definitive treatment. Observation without epinephrine risks cardiovascular collapse and death. - **Option 2 (Switch to LOCM)**: Continuing contrast administration (even with a different agent) is contraindicated in active anaphylaxis. The reaction is already occurring; further contrast exposure worsens angioedema and bronchospasm. The scan is not a priority; patient survival is. - **Option 3 (Corticosteroid alone)**: Methylprednisolone has a delayed onset (30–60 minutes) and is NOT effective for acute anaphylaxis. It is used to prevent biphasic reactions (recurrence 1–72 hours later) but must be given **after** epinephrine and supportive care, not instead of them. **Mnemonic: STOP-EPIPEN** — **S**top contrast, **T**reat immediately, **O**pen airway, **P**repare for intubation, **E**pINephrine IM, **P**erfusion (fluids), **I**V access, **N**itrogen (oxygen), **E**levate legs, **N**otify ICU. ### Post-Reaction Management - **Admission**: Admit to ICU or high-dependency unit for 4–6 hours minimum (risk of biphasic anaphylaxis). - **Premedication for future contrast**: If contrast is essential, premedicate with corticosteroids (methylprednisolone 32 mg PO 12 and 2 hours before) + antihistamine (diphenhydramine 50 mg 1 hour before). - **Alternative imaging**: Consider non-contrast modalities (V/Q scan for PE, echocardiography) or gadolinium (if renal function permits) for future studies. [cite:Harrison 21e Ch 317; American Academy of Allergy, Asthma & Immunology (AAAAI) Anaphylaxis Guidelines] 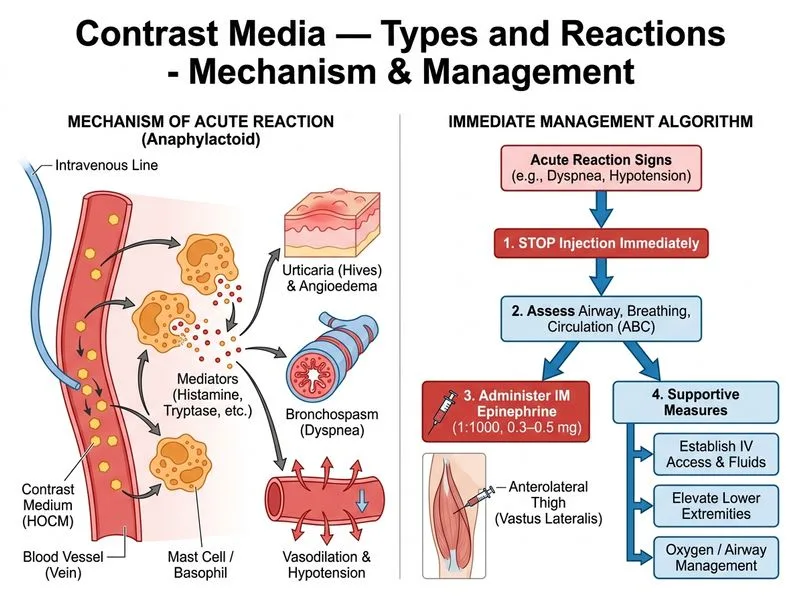
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.