## Acute COPD Exacerbation Management ### Critical Concept: Oxygen Titration in COPD **Key Point:** Patients with COPD are at risk of **hypercapnic respiratory failure** if oxygen is titrated too aggressively. The target SpO₂ in acute exacerbation is **88–92%**, NOT the standard 94–98% used in other respiratory conditions. This narrow range maintains adequate oxygenation while avoiding suppression of the hypoxic respiratory drive and CO₂ retention (GOLD Guidelines 2024; Harrison's Principles of Internal Medicine, 21st ed.). **High-Yield:** Uncontrolled oxygen supplementation in COPD exacerbation can precipitate acute hypercapnic respiratory failure requiring intubation. This is a **classic NEET PG trap**. ### Rationale for Correct Answer (Option A) The correct approach includes: 1. **Oxygen targeting 88–92%** — maintains oxygenation while preserving hypoxic drive. This is consistent with GOLD guidelines and BTS emergency oxygen guidelines. 2. **Salbutamol (SABA) nebulized** — short-acting beta-2 agonist is the **first-line bronchodilator** in acute COPD exacerbation due to rapid onset. While ipratropium can be added for synergy, salbutamol is the primary agent and is universally recommended as the initial bronchodilator. 3. **Systemic corticosteroids** — prednisolone 40 mg daily × 5 days reduces exacerbation duration, improves FEV₁ recovery, and decreases treatment failure rates (GOLD 2024). 4. **Empiric narrow-spectrum antibiotics** — indicated because sputum is purulent (Anthonisen criteria: increased dyspnea + increased sputum volume + purulent sputum = Type 1 exacerbation). For moderate exacerbations without risk factors for *Pseudomonas*, **narrow-spectrum agents** such as amoxicillin, doxycycline, or a macrolide are appropriate first-line empiric choices per GOLD guidelines. Broad-spectrum agents (e.g., fluoroquinolones, amoxicillin-clavulanate) are reserved for patients with risk factors for resistant organisms (frequent exacerbations, recent hospitalization, prior antibiotic use, severe COPD with FEV₁ <30%). ### Why Option A is Preferred Over Option D - Option D specifies **ipratropium** as the sole nebulized bronchodilator. While ipratropium is useful as an add-on, **salbutamol (SABA) is the primary first-line nebulized bronchodilator** in acute exacerbations per GOLD guidelines. - Option D also specifies **broad-spectrum antibiotics**, which are not the first-line empiric choice for a moderate exacerbation without documented risk factors for resistant organisms. Narrow-spectrum antibiotics are appropriate initial empiric therapy. - Option A correctly pairs salbutamol with narrow-spectrum antibiotics, reflecting guideline-concordant care for this clinical scenario. ### Why Other Options Are Incorrect | Option | Error | |--------|-------| | B | SpO₂ target >95% is dangerous in COPD; withholding antibiotics with purulent sputum is incorrect | | C | SpO₂ target 94–98% risks hypercapnic respiratory failure in COPD | | D | Ipratropium alone (without salbutamol) is suboptimal; broad-spectrum antibiotics not first-line for moderate exacerbation without risk factors | ### Anthonisen Criteria for Antibiotic Use in COPD Exacerbation - **Type 1** (all 3): Increased dyspnea + increased sputum + purulent sputum → **Antibiotics indicated** - **Type 2** (any 2 of 3): Antibiotics indicated if purulence is one criterion - **Type 3** (1 of 3): Antibiotics generally NOT indicated **Clinical Pearl:** Per GOLD 2024, empiric antibiotic choice should be guided by local resistance patterns. For patients without *Pseudomonas* risk factors, narrow-spectrum agents (amoxicillin, doxycycline, macrolide) are preferred. Broad-spectrum coverage is escalated based on culture results or risk stratification. **Mnemonic:** **SOCS** — **S**albutamol nebulized, **O**xygen (88–92%), **C**orticosteroids systemic, **S**mart (narrow-spectrum) antibiotics. 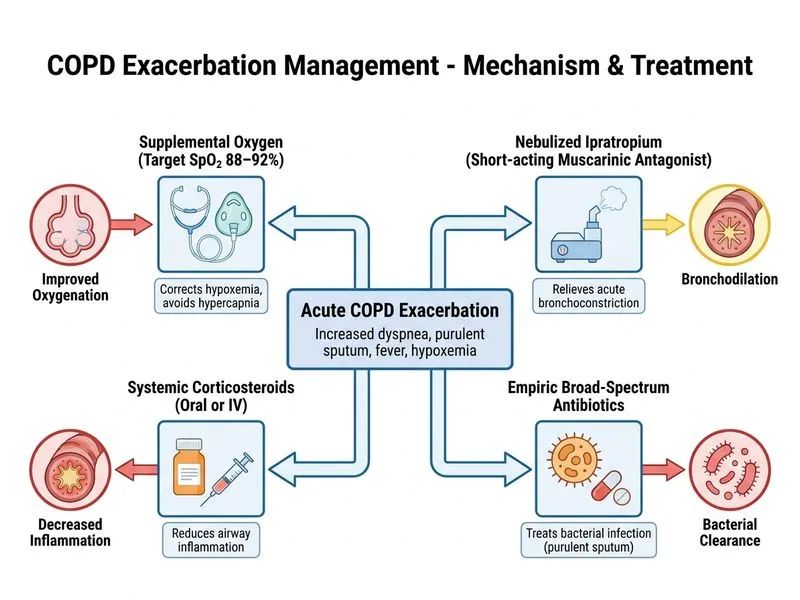
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.