## Acute COPD Exacerbation with Hypercapnic Respiratory Failure **Key Point:** This patient has **Type II respiratory failure** (hypercapnia: PaCO₂ 58 mmHg) with **mild acidemia** (pH 7.32). The triad of management is: **controlled oxygen**, **corticosteroids**, and **antibiotics**. ### ABG Interpretation | Parameter | Value | Interpretation | |---|---|---| | pH | 7.32 | Acidemia | | PaCO₂ | 58 mmHg | Hypercapnia (Type II RF) | | HCO₃⁻ | 28 mEq/L | Metabolic compensation (chronic) | | PaO₂ | 62 mmHg | Hypoxemia | | **Status** | — | **Acute-on-chronic hypercapnic RF** | **High-Yield:** In COPD, **uncontrolled high-flow oxygen is dangerous**—it can suppress hypoxic respiratory drive and worsen CO₂ retention. Target SpO₂ is **88–92%** (not >94%). ### Stepwise Management of Acute COPD Exacerbation ```mermaid flowchart TD A[Acute COPD Exacerbation]:::outcome --> B{Respiratory Failure?}:::decision B -->|Type I<br/>PaO2 <60| C[High-flow O2<br/>Target SpO2 >90%]:::action B -->|Type II<br/>PaCO2 >45| D[Controlled O2<br/>Target SpO2 88-92%]:::action D --> E[Assess for NIV]:::decision E -->|pH <7.25 or<br/>RR >30| F[Non-invasive Ventilation]:::action E -->|pH >7.25 &<br/>RR <30| G[Medical therapy alone]:::action G --> H[Corticosteroids<br/>Antibiotics<br/>Bronchodilators]:::action F --> H H --> I[Monitor ABG<br/>in 1-2 hours]:::action ``` ### Why Controlled Oxygen (88–92%) in This Case 1. **PaCO₂ 58 mmHg** indicates CO₂ retention; aggressive oxygenation will suppress respiratory drive. 2. **pH 7.32** is mild acidemia—not yet critical (pH <7.25 would prompt immediate NIV). 3. **RR not stated** but likely elevated; if <30, medical therapy is first-line. 4. **Controlled oxygen** maintains adequate oxygenation while preserving respiratory drive. ### Pharmacological Pillars **Corticosteroids:** - Dose: Prednisolone 30–40 mg daily (or IV methylprednisolone 125 mg 6-hourly) for 5–7 days. - Reduces inflammation, shortens hospital stay, improves FEV₁ recovery. **Antibiotics:** - Indicated if sputum purulence (present here) or fever. - First-line: Amoxicillin-clavulanate or fluoroquinolone (e.g., levofloxacin). - Covers *Haemophilus influenzae*, *Streptococcus pneumoniae*, *Moraxella catarrhalis*. **Bronchodilators:** - Nebulized salbutamol ± ipratropium (anticholinergic) for acute relief. **Clinical Pearl:** NIV is indicated if pH <7.25 or RR >30 despite medical therapy. This patient's pH is 7.32 and RR is not critically elevated, so medical therapy is the starting point. Reassess ABG in 1–2 hours; if worsening, escalate to NIV. **Warning:** ~~High-flow oxygen (target SpO₂ >94%)~~ is a common trap in COPD exacerbation—it worsens CO₂ retention and can precipitate respiratory acidosis requiring intubation. **Mnemonic: COPD Exacerbation ABC** — **A**irway (controlled O₂, 88–92%), **B**ronchodilators (nebulized), **C**orticosteroids + antibiotics. [cite:Harrison 21e Ch 254; GOLD 2023 Report] 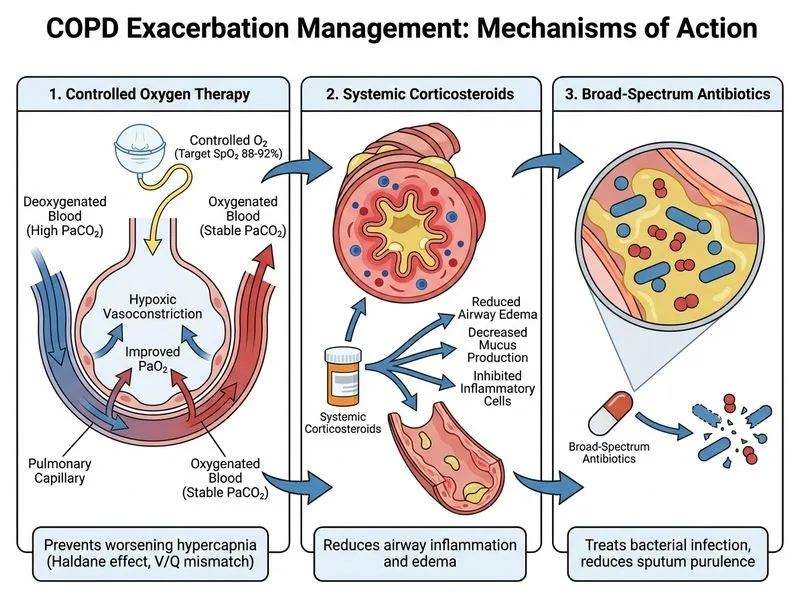
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.