## Organism Identification **Key Point:** The combination of: - Gram-negative rod - Mucoid, non-lactose-fermenting colony on MacConkey agar - Greenish tinge to the ulcer - Rapid progression (3 days) with stromal infiltration and hypopyon ...is pathognomonic for **_Pseudomonas aeruginosa_**, the most common Gram-negative cause of bacterial corneal ulcer in India. **High-Yield:** *Pseudomonas* characteristics: - Aerobic, motile, Gram-negative rod - Produces pyoverdine (greenish pigment) and pyocyanin (blue pigment) - Non-lactose-fermenting on MacConkey (appears as clear/colorless colonies) - Mucoid phenotype indicates biofilm production (virulence factor) - Produces proteolytic enzymes → rapid stromal melting and perforation risk ## Differential Diagnosis of Gram-Negative Corneal Ulcers | Organism | Gram Stain | MacConkey | Pigment | Clinical Features | Topical Agent | | --- | --- | --- | --- | --- | --- | | *Pseudomonas aeruginosa* | GNR | NLF, mucoid | Green/blue | Rapid, stromal melt, hypopyon | Gentamicin, fluoroquinolone | | *Neisseria gonorrhoeae* | GDC | NLF, oxidase+ | None | Purulent discharge, rapid | Ceftriaxone, spectinomycin | | *Vibrio cholerae* | GNR, comma | NLF, oxidase+ | None | Rare in eye; diarrhea history | Chloramphenicol, tetracycline | | *Klebsiella pneumoniae* | GNR | LF, mucoid | None | Slower progression | Cephalosporin, fluoroquinolone | **Legend:** GNR = Gram-negative rod; GDC = Gram-negative diplococcus; NLF = non-lactose-fermenting; LF = lactose-fermenting. ## Treatment Algorithm ```mermaid flowchart TD A[Bacterial corneal ulcer suspected]:::outcome --> B[Gram stain + culture]:::action B --> C{Gram-negative rod?}:::decision C -->|Yes| D{Mucoid, NLF on MacConkey?}:::decision D -->|Yes| E[Pseudomonas aeruginosa]:::outcome D -->|No| F[Klebsiella or other GNR]:::outcome E --> G[Topical gentamicin 0.3% or fluoroquinolone hourly]:::action F --> H[Topical cephalosporin or fluoroquinolone]:::action G --> I[Add systemic fluoroquinolone if severe]:::action I --> J[Monitor for perforation daily]:::outcome ``` **Key Point:** Topical gentamicin (aminoglycoside) or fluoroquinolone (e.g., ofloxacin, moxifloxacin) are the preferred agents for *Pseudomonas* corneal ulcer because: 1. High corneal penetration and bactericidal activity 2. Broad spectrum covers other Gram-negative and Gram-positive organisms 3. Fluoroquinolones have superior corneal bioavailability **Clinical Pearl:** *Pseudomonas* is an **obligate aerobe** and produces proteolytic enzymes that can cause rapid stromal melting and perforation within 24–48 hours. Aggressive topical therapy (hourly instillation) and close monitoring are essential. Systemic fluoroquinolone (e.g., ciprofloxacin 500 mg BD) should be added for severe cases. **Warning:** Avoid topical steroids in *Pseudomonas* ulcer — they accelerate stromal melting and perforation. Do NOT use topical penicillins or cephalosporins alone; aminoglycosides or fluoroquinolones are superior. 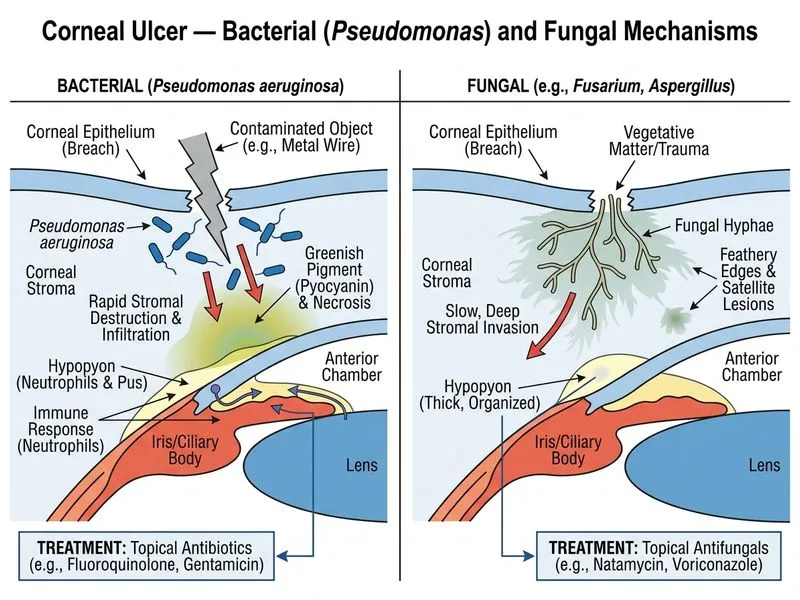
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.