## Why Vasa Recta Atrophy Abolishes Urine Concentration **Key Point:** The vasa recta is not responsible for *creating* the medullary osmotic gradient — the loop of Henle does that. However, the vasa recta is essential for *preserving* that gradient. Without functional vasa recta, the gradient is rapidly dissipated, and urine concentration fails. ### The Two-Step Process of Urine Concentration ```mermaid flowchart TD A[Loop of Henle: Active Na+ transport in TAL]:::action --> B[Creates medullary osmotic gradient<br/>Cortex ~300 mOsm/kg<br/>Medulla ~1200 mOsm/kg]:::outcome B --> C[Vasa Recta: Passive exchange]:::action C --> D[Preserves gradient by equilibrating<br/>solutes and water without washout]:::outcome D --> E[ADH acts on collecting duct<br/>Water reabsorption occurs<br/>Concentrated urine produced]:::action F[Vasa Recta atrophy<br/>Reduced medullary blood flow]:::urgent --> G[Gradient dissipates<br/>Medulla osmolality drops]:::urgent G --> H[Collecting duct cannot reabsorb water<br/>Dilute urine despite ADH]:::urgent ``` ### Role of Vasa Recta in Gradient Preservation **Why the vasa recta matters:** 1. **The problem:** The medullary interstitium is constantly being perfused by blood from the systemic circulation. If this blood were to simply wash away solutes, the gradient would collapse. 2. **The solution:** The vasa recta uses countercurrent exchange to equilibrate with the medullary osmolality WITHOUT dissipating the gradient: - Descending limb: water leaves, solutes enter → blood osmolality rises - Ascending limb: solutes leave, water enters → blood osmolality falls - Net result: blood leaving vasa recta has near-normal osmolality; gradient is preserved 3. **If vasa recta is damaged:** - Reduced blood flow → less efficient equilibration - Solutes are washed away faster than they can be replaced by the loop - Medullary osmolality drops (in this case, from ~1200 to ~250 mOsm/kg) - Even with intact loop and ADH, collecting duct cannot reabsorb water ### Why the Loop of Henle Alone Is Not Enough The loop of Henle continuously pumps solute into the medullary interstitium. However, this solute must be **removed by the vasa recta** and returned to the systemic circulation. If the vasa recta cannot do this efficiently: - Solute accumulates transiently, then is washed away by diffusion into surrounding tissue - The gradient equilibrates with the cortex - Urine osmolality approaches plasma osmolality (dilute urine) ### Clinical Correlation **High-Yield:** Patients with: - Sickle cell disease (vasa recta infarction) - Severe dehydration (reduced medullary blood flow) - Analgesic nephropathy (papillary necrosis → vasa recta loss) - Renal medullary cystic disease All present with **inability to concentrate urine despite normal ADH levels** — because the medullary gradient is lost. ### Comparison: Loop Dysfunction vs. Vasa Recta Dysfunction | Finding | Loop of Henle Damage | Vasa Recta Damage | | --- | --- | --- | | **Medullary gradient** | Reduced or absent | Initially present, then dissipates | | **Urine osmolality** | Dilute (< 300 mOsm/kg) | Dilute (< 300 mOsm/kg) | | **ADH response** | Poor (no gradient to work with) | Poor (no gradient to work with) | | **Loop of Henle histology** | Damaged/atrophic | **Intact** | | **Vasa recta histology** | Normal | **Atrophic/damaged** | | **Distinguishing feature** | Structural loop damage | Preserved loop, failed gradient preservation | **Clinical Pearl:** In this case, the **preserved loop of Henle architecture** rules out loop dysfunction. The **vasa recta atrophy** explains why the gradient cannot be maintained, even though the loop is trying to create it. This is a classic scenario in chronic kidney disease with medullary ischemia. 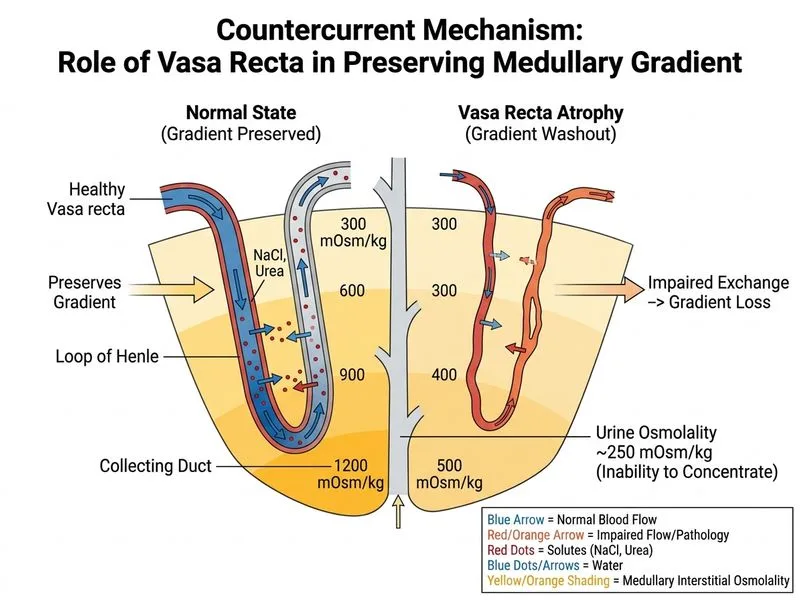
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.