## Histopathological Distinction Between Crohn Disease and Ulcerative Colitis **Key Point:** Non-caseating granulomas are the hallmark histological feature of Crohn disease, present in approximately 30–50% of surgical specimens and 15–30% of endoscopic biopsies. They are virtually absent in ulcerative colitis. ### Comparative Histology Table | Feature | Crohn Disease | Ulcerative Colitis | | --- | --- | --- | | **Non-caseating granulomas** | Present (30–50%) | Absent | | **Crypt abscess** | Yes | Yes | | **Surface ulceration** | Yes | Yes | | **Mucin depletion** | Yes | Yes | | **Transmural inflammation** | Yes (hallmark) | No (mucosa/submucosa only) | | **Skip lesions** | Yes | No | | **Fissuring ulcers** | Yes | No | **High-Yield:** When a granuloma is identified in a colonic biopsy, Crohn disease is the leading diagnosis. However, absence of granulomas does NOT exclude Crohn disease — the diagnosis rests on the full clinicopathological picture (transmural inflammation, skip lesions, fissuring ulcers). **Clinical Pearl:** The presence of granulomas in a patient with inflammatory bowel disease strongly favors Crohn disease over ulcerative colitis and may influence management decisions (e.g., consideration of methotrexate or biologics). **Mnemonic: "CRAG"** — **C**rohn has **R**andomous skip lesions, **A**ll layers (transmural), and **G**ranulomas. 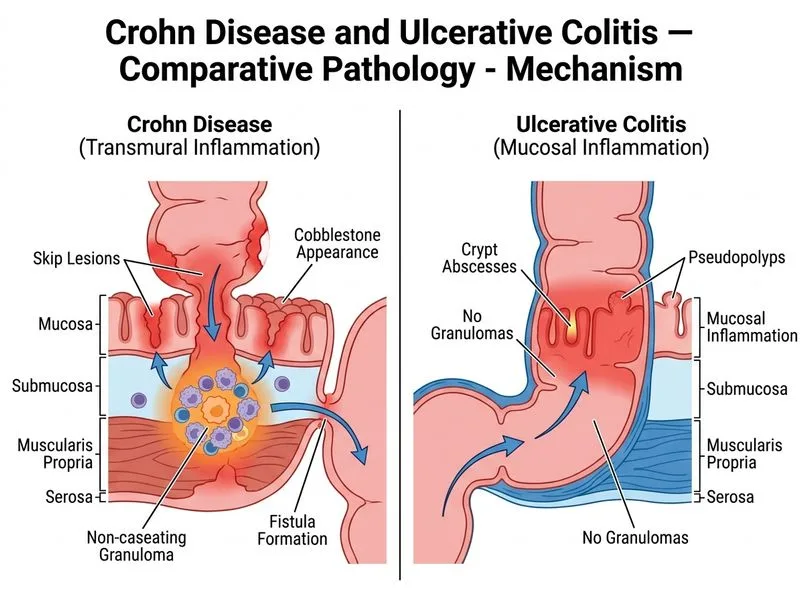
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.