## Clinical Scenario Analysis This patient has **Crohn disease (CD)** with the following classic features: - Skip lesions (discontinuous inflammation) - Cobblestone appearance and aphthous ulcers - **Transmural inflammation with non-caseating granulomas** (pathognomonic for CD) - Terminal ileal involvement (most common site in CD) - Extraintestinal manifestation: erythema nodosum - First presentation, steroid-naive, normal albumin (not severely malnourished) ## Why CT Enterography Is the Critical Next Step **Key Point:** Before initiating systemic therapy in CD, **imaging of the entire small bowel is essential** to: 1. Define the full extent of disease (CD is patchy; skip lesions may extend beyond colonoscopic reach) 2. Detect complications: fistulas, strictures, abscesses, perforation 3. Guide therapeutic strategy (medical vs. surgical) 4. Establish baseline for monitoring **High-Yield:** CT enterography is superior to colonoscopy alone because it visualizes the entire small bowel (colonoscopy reaches only to terminal ileum) and assesses transmural disease, mesenteric inflammation, and complications. ## Management Algorithm for CD Induction ```mermaid flowchart TD A[Confirmed CD diagnosis]:::outcome --> B[CT enterography]:::action B --> C{Complications present?}:::decision C -->|Fistula/abscess| D[Percutaneous drainage + antibiotics]:::action C -->|Stricture/obstruction| E[Consider surgery]:::action C -->|None| F{Disease severity?}:::decision F -->|Mild-moderate, no complications| G[Corticosteroids or 5-ASA]:::action F -->|Moderate-severe| H[Corticosteroids + azathioprine/biologics]:::action G --> I[Assess response at 4 weeks]:::decision H --> J[Assess response at 4 weeks]:::decision ``` ## Induction Therapy Hierarchy for CD | Disease Severity | First-Line Therapy | Rationale | |---|---|---| | Mild-moderate, no complications | Corticosteroids (prednisolone 40–60 mg/day tapering) OR 5-ASA | Rapid anti-inflammatory effect | | Moderate-severe | Corticosteroids + azathioprine/6-MP (start early) | Steroid-sparing; immunomodulation | | Severe/fulminant | IV methylprednisolone + infliximab (if no contraindications) | Rapid response; TNF inhibition | | Fistulizing CD | Infliximab ± azathioprine; percutaneous drainage if abscess | TNF inhibitors are DOC for fistulas | **Clinical Pearl:** Infliximab is NOT first-line for induction of remission in uncomplicated CD; it is reserved for: - Moderate-to-severe disease refractory to corticosteroids - Fistulizing disease - Steroid-dependent disease **Mnemonic:** **STEP-UP** — **S**mall bowel imaging first, **T**hen assess complications, **E**scalate therapy based on severity, **P**redict need for surgery, **U**se biologics for refractory/fistulizing disease, **P**erform monitoring. ## Why Corticosteroids Alone Is Premature While corticosteroids will be part of the induction regimen, **imaging must precede systemic therapy** to exclude complications that would change management (e.g., an abscess would require drainage before or alongside antibiotics and steroids; a stricture might warrant surgery). 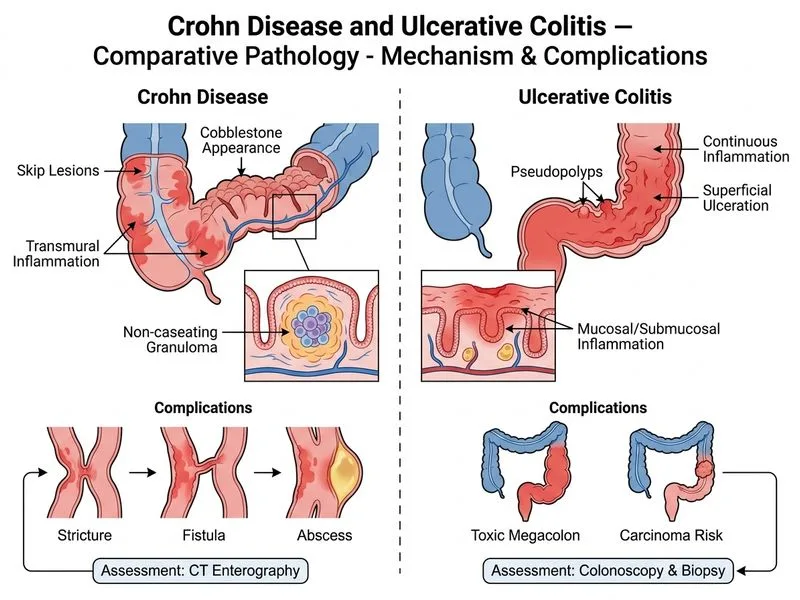
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.