## Distinguishing Ulcerative Colitis from Crohn Disease: Continuous Mucosal Inflammation ### The Gold Standard Discriminator **Key Point:** Continuous inflammation limited to the mucosa and submucosa, starting at the rectum and extending proximally **without skip lesions**, is the single most reliable histopathological feature distinguishing ulcerative colitis (UC) from Crohn disease (CD) in a colonic biopsy specimen. ### Comparative Pathology: Distribution Pattern | Aspect | Ulcerative Colitis | Crohn Disease | | --- | --- | --- | | **Pattern** | Continuous, uniform | Skip lesions (patchy, discontinuous) | | **Starting point** | Always rectum | Can start anywhere (mouth to anus) | | **Depth** | Mucosa + submucosa only | Transmural (all layers) | | **Skip lesions** | NEVER present | Characteristic feature | | **Granulomas** | Absent | Present in only ~30–50% of biopsies | | **Rectum involvement** | Always involved | May spare rectum | ### Why Option C Is Correct **High-Yield:** The continuous, rectum-based, non-transmural pattern of inflammation is present in **virtually 100% of UC cases** and is absent in CD. This makes it the most *reliable* (i.e., most sensitive and specific) single histopathological discriminator available on a colonic biopsy. Skip lesions, when present, exclude UC entirely. ### Why the Other Options Are Incorrect or Less Reliable - **Option A — Cobblestone appearance with intervening normal mucosa:** This is a **macroscopic/endoscopic** finding of Crohn disease, not a histopathological feature seen on biopsy. It reflects submucosal edema and linear ulceration but is not assessed microscopically. - **Option B — Non-caseating granulomas:** Although granulomas are **pathognomonic for CD when present**, they are found in only **30–50% of Crohn colonic biopsies** (Robbins 10e, Ch 17). Their absence does not exclude CD, making them an unreliable discriminator. A feature present in only half of cases cannot be the "most reliable" distinguishing feature. - **Option D — Transmural involvement with fissuring ulcers:** Transmural inflammation is characteristic of CD, but assessing transmural depth requires **full-thickness surgical specimens**, not routine mucosal biopsies. This feature is therefore not reliably assessable in a standard colonic biopsy. **Clinical Pearl:** If biopsies from multiple colonic segments show continuous mucosal inflammation beginning at the rectum with no intervening normal mucosa, UC is the diagnosis. If any segment shows normal mucosa between inflamed areas (skip lesion), UC is excluded and CD must be considered — even in the absence of granulomas. **Mnemonic: UC = CONTINUOUS** — **U**lcerative **C**olitis: **C**ontinuous, **O**nly mucosa/submucosa, **N**o skip lesions, **T**ypically rectum-based, **I**nflammation uniform, **N**ever transmural, **U**niform distribution, **O**nly colon, **U**nbroken, **S**tarts at rectum always. [cite: Robbins & Cotran Pathologic Basis of Disease, 10e, Ch 17; Kumar V et al., Robbins Basic Pathology, 10e] 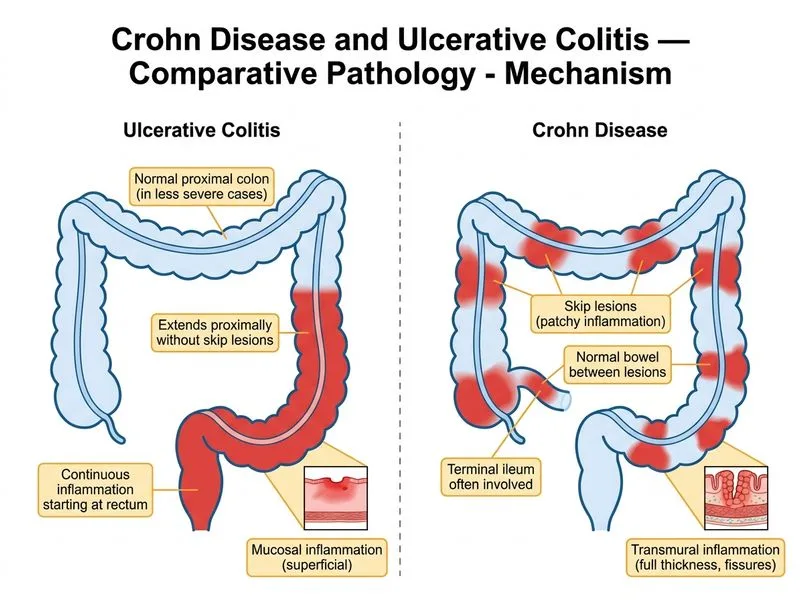
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.