## Diagnosis: Crohn Disease ### Key Clinical and Pathological Features **Key Point:** The combination of **skip lesions** (patchy discontinuous inflammation), **transmural inflammation**, **non-caseating granulomas**, and **perianal complications** (skin tags, fistula) is diagnostic of Crohn disease. ### Distinguishing Histopathology and Clinical Features | Feature | Crohn Disease | Ulcerative Colitis | |---------|---------------|-------------------| | **Distribution** | Skip lesions (patchy, discontinuous) | Continuous from rectum | | **Depth** | Transmural (all layers) | Mucosa + submucosa only | | **Granulomas** | Non-caseating in 50–60% | Absent | | **Perianal disease** | Present in ~30% (fistulas, skin tags, abscesses) | Absent | | **Terminal ileum involvement** | Common | Never | | **Fissuring ulcers** | Yes (cobblestone appearance) | No | | **Diarrhoea type** | Non-bloody (unless severe) | Bloody (hallmark) | **High-Yield:** The **skip lesions + transmural inflammation + granulomas + perianal fistula** triad is pathognomonic for Crohn disease. Terminal ileum involvement is virtually diagnostic. ### Pathological Hallmarks of Crohn Disease 1. **Skip lesions**: Areas of inflamed mucosa separated by normal segments 2. **Transmural inflammation**: Extends through all bowel wall layers → risk of fistulas and strictures 3. **Non-caseating granulomas**: Found in ~50–60% of cases (not tuberculous) 4. **Fissuring ulcers**: Deep ulcers that may penetrate transmurally 5. **Cobblestone appearance**: Due to transmural inflammation and fibrosis **Clinical Pearl:** Perianal disease (fistulas, skin tags, abscesses) occurs in ~30% of Crohn patients and is virtually **never** seen in UC. This patient's draining fistula is a red flag for Crohn disease. ### Why This Is NOT Ulcerative Colitis UC would show: - **Continuous** inflammation starting from rectum (not skip lesions) - **Mucosal-and-submucosal** involvement only (not transmural) - **No granulomas** - **No perianal disease** or fistulas - **Bloody diarrhoea** (hallmark) — this patient has non-bloody diarrhoea ### Why This Is NOT Behçet Disease Behçet disease with GI involvement: - Presents with oral and genital ulcers (not present here) - Causes recurrent oral aphthous ulcers - GI lesions are typically in the ileocaecal region but lack granulomas - Diagnosis requires ocular involvement (uveitis) or genital ulcers ### Why This Is NOT Tuberculosis of the Colon TB colitis would show: - **Caseating granulomas** (not non-caseating) - **Acid-fast bacilli** (AFB) on Ziehl-Neelsen stain (absent in Crohn) - **Transverse ulcers** (vs. fissuring in Crohn) - **Strictures** at the ileocaecal junction - Systemic TB signs (fever, night sweats, TB contact history) This patient has **non-caseating granulomas**, which exclude TB. ### Diagnostic Algorithm ```mermaid flowchart TD A[IBD suspected]:::outcome --> B{Skip lesions?}:::decision B -->|No, continuous| C{Mucosal-only?}:::decision B -->|Yes, patchy| D{Transmural?}:::decision C -->|Yes| E[Ulcerative Colitis]:::action C -->|No| F[Consider other dx] D -->|Yes| G{Granulomas?}:::decision D -->|No| H[Consider other dx] G -->|Yes, non-caseating| I[Crohn Disease]:::action G -->|Yes, caseating| J[TB colitis]:::urgent I --> K{Perianal disease?}:::decision K -->|Yes| L[Confirms Crohn]:::outcome ``` **Mnemonic — Crohn Disease Features:** **"FISTULA CROHN"** - **F**issuring ulcers - **I**leal involvement - **S**kip lesions - **T**ransmural - **U**lceration (deep) - **L**ocal complications (fistulas, abscesses) - **A**ll layers involved - **C**obblestone - **R**ectal sparing - **O**ral ulcers (aphthous) - **H**ealth complications (perianal) - **N**on-caseating granulomas 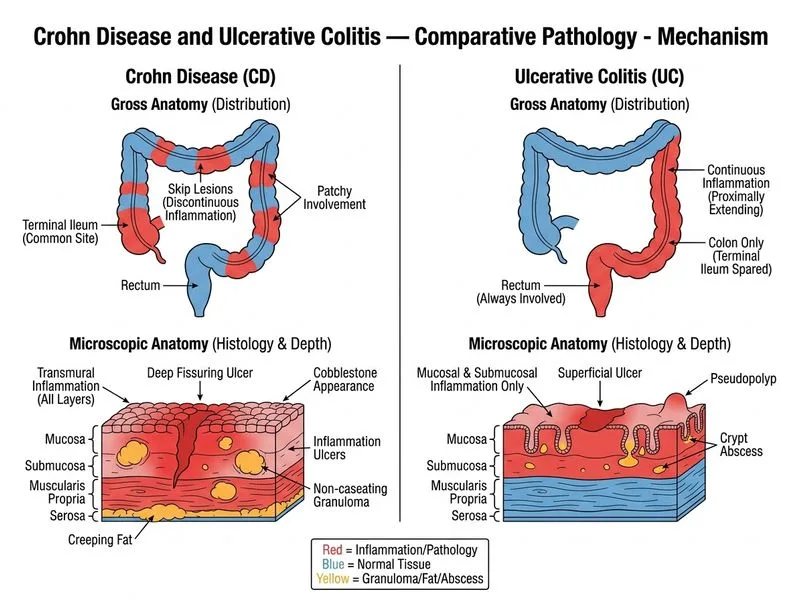
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.