## Investigation of Choice for Crohn Disease Assessment **Key Point:** MR enterography is the gold standard for assessing the full extent of small bowel and colonic involvement in suspected Crohn disease, particularly when transmural disease and complications (fistulas, strictures, abscesses) need to be evaluated. ### Why MR Enterography is Superior **High-Yield:** MR enterography provides: - Non-ionizing radiation (important for young patients requiring serial imaging) - Excellent visualization of transmural inflammation and bowel wall thickening - Superior soft-tissue contrast for detecting fistulas, abscesses, and mesenteric fat stranding - Assessment of small bowel disease (which colonoscopy cannot reach) - Functional information (cine sequences showing reduced motility) ### Clinical Context in This Case The patient's presentation is classic for Crohn disease: - Patchy inflammation with skip lesions on colonoscopy (pathognomonic for Crohn) - Perianal manifestations (skin tags, fistula) — occur in ~30% of Crohn patients - Weight loss and chronic diarrhea MR enterography will: 1. Confirm transmural inflammation (diagnostic hallmark of Crohn) 2. Assess for small bowel involvement (present in ~75% of Crohn cases) 3. Detect fistulizing disease and guide surgical planning 4. Establish baseline for monitoring disease progression ### Comparison with Other Modalities | Investigation | Strength | Limitation | |---|---|---| | **MR enterography** | Transmural disease, fistulas, small bowel, no radiation | Contraindicated if metallic implants | | Barium enema | Mucosal detail | Poor soft-tissue contrast, radiation, cannot assess transmural disease | | CT colonography | Fast, good for strictures | Radiation exposure, less soft-tissue detail than MR | | Fecal calprotectin | Biomarker of inflammation | Non-specific, cannot define anatomy or complications | **Clinical Pearl:** Perianal fistulas in a young patient with skip lesions on colonoscopy should raise suspicion for Crohn disease. MR imaging is essential to map fistula tracts and plan surgical intervention. **Warning:** Do not confuse fecal calprotectin (useful for screening and monitoring activity) with anatomical imaging — it cannot diagnose or assess structural complications. 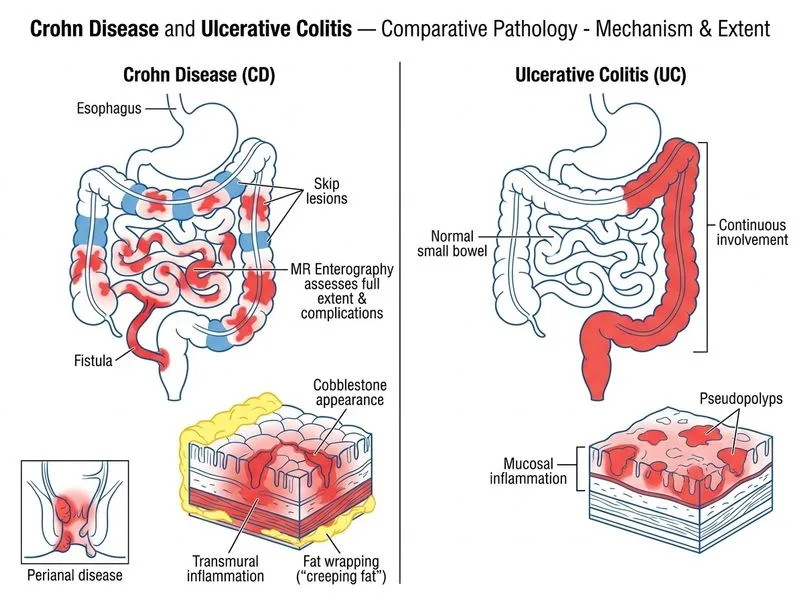
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.