## Clinical Diagnosis: Crohn Disease This patient has **Crohn disease (CD)** confirmed by: - Skip lesions (patchy inflammation with normal intervening mucosa) - Transmural inflammation (extends through all bowel wall layers) - Non-caseating granulomas (pathognomonic for CD) - Perianal fistulae (CD-specific complication) - Ileocaecal involvement (most common site) ## Key Management Principle: Steroid-Dependent Disease **High-Yield:** The patient is **steroid-dependent** (requires prednisolone to maintain remission after a 6-week course). This is the critical trigger for escalation to **biologic therapy** (TNF-α inhibitor). **Key Point:** Steroid-dependent Crohn disease requires immunosuppression or biologic therapy to: 1. Induce and maintain remission 2. Reduce steroid requirement and toxicity 3. Prevent complications (fistulae progression, strictures) ## Management Algorithm for Steroid-Dependent Crohn Disease ```mermaid flowchart TD A[Crohn Disease]:::outcome --> B{Response to induction steroids?}:::decision B -->|Yes, remission| C[Assess steroid-dependence]:::decision C -->|Steroid-independent| D[5-ASA or mesalamine maintenance]:::action C -->|Steroid-dependent| E[Escalate to immunosuppression]:::action E --> F{Fistulizing disease?}:::decision F -->|Yes| G[TNF-inhibitor: Infliximab]:::action F -->|No| H[Azathioprine or TNF-inhibitor]:::action B -->|Steroid-refractory| I[TNF-inhibitor or surgery]:::action G --> J[Taper prednisolone]:::action H --> K[Taper prednisolone]:::action ``` ## Why Infliximab Is Correct | Criterion | Azathioprine | Infliximab | |-----------|--------------|------------| | **Onset** | 8–12 weeks | 2–4 weeks | | **Steroid-dependent CD** | Second-line option | **First-line** | | **Fistulizing CD** | Not effective | **Highly effective** | | **Transmural disease** | Moderate efficacy | **Superior efficacy** | | **Remission induction** | No | **Yes** | **Clinical Pearl:** Infliximab is particularly indicated in this patient because: 1. She has **fistulizing disease** (perianal fistulae) — TNF-α inhibitors are the only agents proven to close fistulae in CD 2. She is **steroid-dependent** — requires biologic therapy to allow steroid withdrawal 3. She has **transmural inflammation** — TNF-α inhibitors penetrate all layers and reduce transmural complications ## Infliximab Induction Protocol - **Dose:** 5 mg/kg IV infusion - **Schedule:** Weeks 0, 2, and 6 (induction phase) - **Maintenance:** 5 mg/kg every 8 weeks (after week 14) - **Concurrent therapy:** Continue mesalamine; taper prednisolone by 5 mg every 1–2 weeks **Mnemonic:** **FIST** = **F**istulizing disease, **I**mmune-mediated complications, **S**teroid-dependent, **T**ransmural → TNF-inhibitor ## Why Not the Other Options? **Option 1 (Increase prednisolone):** Increasing steroid dose in steroid-dependent disease is counterproductive: - Increases toxicity (osteoporosis, infections, hyperglycaemia) - Does not address underlying pathology - Prolongs steroid dependence - Guideline-discordant **Option 2 (Azathioprine monotherapy):** While azathioprine can be used for steroid-dependent CD, it: - Takes 8–12 weeks to work (slow onset) - Is less effective than TNF-inhibitors for fistulizing disease - Does not induce remission as rapidly - Is typically second-line after TNF-inhibitor failure or in combination with TNF-inhibitors **Option 4 (Surgery):** Ileocaecal resection is curative for localized disease but: - Is not first-line for steroid-dependent disease - Should be reserved for complications (strictures, perforation, intractable disease despite medical therapy) - This patient has not yet failed biologic therapy 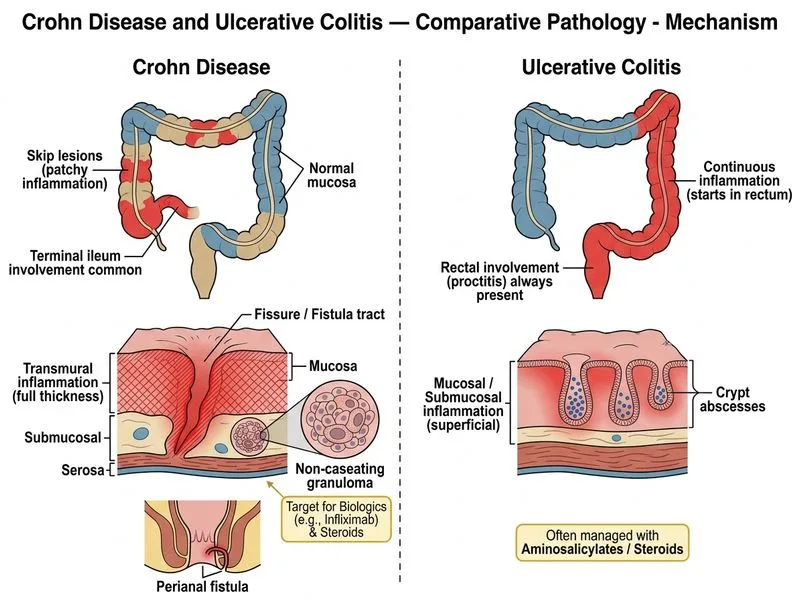
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.