## Epidemiology of Cushing Syndrome **Key Point:** Pituitary adenoma (Cushing disease) accounts for approximately 70–80% of all cases of Cushing syndrome, making it the most common cause worldwide. ### Distribution of Causes | Cause | Frequency | Pathophysiology | | --- | --- | --- | | **Pituitary adenoma (Cushing disease)** | **70–80%** | **ACTH-secreting microadenoma; ACTH-dependent** | | Adrenocortical carcinoma | 10–15% | Autonomous cortisol production; ACTH-independent | | Ectopic ACTH secretion | 10–15% | Non-pituitary tumour (lung, thymus, pancreas); ACTH-dependent | | Primary adrenal hyperplasia | <1% | Rare; ACTH-independent | **High-Yield:** In clinical practice, when a patient presents with Cushing syndrome, the first diagnostic step is to confirm hypercortisolism (24-hour urine free cortisol, late-night salivary cortisol, or dexamethasone suppression test). The next step is to measure plasma ACTH to differentiate ACTH-dependent (pituitary or ectopic) from ACTH-independent (adrenal) causes. Pituitary adenoma is by far the most likely diagnosis in an ACTH-dependent case. **Clinical Pearl:** Most pituitary adenomas in Cushing disease are microadenomas (<10 mm) and may not be visible on standard MRI; selective venous sampling of the inferior petrosal sinus may be needed for diagnosis. **Mnemonic:** **PACE** — Pituitary (most common), Adrenal, Carcinoma (ectopic), Ectopic ACTH. 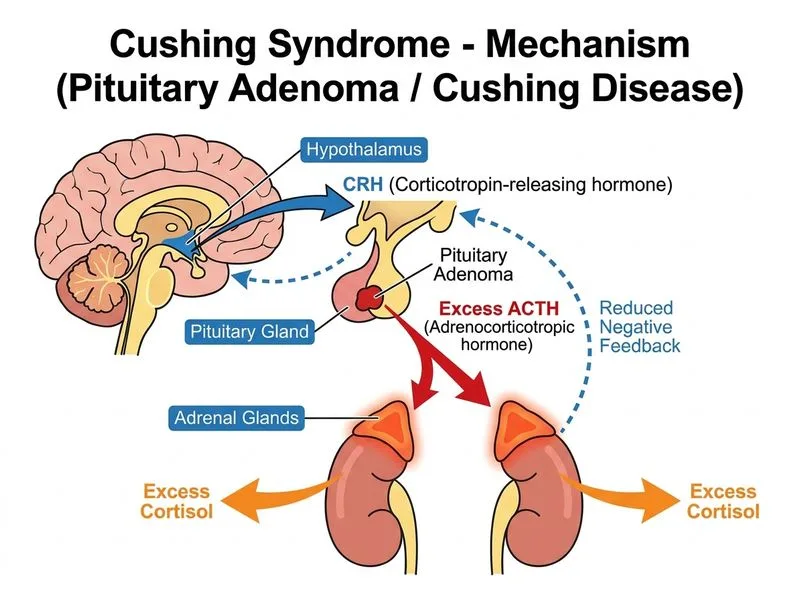
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.