## Diagnosis and Context This clinical presentation is consistent with **cutaneous squamous cell carcinoma (cSCC)**, specifically a high-risk variant. The key features include: - Rapid growth on sun-exposed area (dorsum of hand) - Indurated nodule with central ulceration and rolled edges (classic SCC morphology) - Histologic findings: infiltrative growth, perineural invasion, desmoplasia (all high-risk features) ## Prognostic Factors in Cutaneous SCC | Factor | Significance | Impact on Management | |--------|-------------|----------------------| | **Depth of invasion (Breslow equivalent)** | Tumors >4 mm or Clark level IV–V have significantly higher recurrence and metastasis rates | Requires wider margins (≥6 mm) and consideration of sentinel lymph node biopsy | | **Perineural invasion (PNI)** | Present in 5–15% of cSCC; associated with 5-year recurrence rates of 47% vs. 5% without PNI | Mandates adjuvant radiotherapy; increases risk of local, regional, and distant recurrence | | Ulceration | Marker of aggressive behavior; associated with worse prognosis | Influences margin width but not as strongly as depth + PNI | | Differentiation & mitotic rate | Moderate prognostic value; well-differentiated tumors have better outcomes | Secondary to depth and PNI in risk stratification | | Clark level | More relevant in melanoma; less predictive in cSCC than Breslow-equivalent depth | Not the primary determinant in cSCC prognosis | ## Why Depth + Perineural Invasion is Most Important **Key Point:** The combination of **depth of invasion (Breslow thickness equivalent) and perineural invasion** is the single most powerful predictor of recurrence, metastasis, and mortality in cSCC. **High-Yield:** According to NCCN and AJCC guidelines, cSCC with any of the following are considered "high-risk": - Depth >4 mm or Clark level IV–V - Perineural invasion - Poor differentiation - Immunosuppression **Clinical Pearl:** Perineural invasion is particularly ominous because it allows tumor cells to travel along nerve sheaths, bypassing normal lymphatic drainage and enabling skip metastases. This is why adjuvant radiotherapy (not just wider excision) is recommended. ## Management Implications 1. **Surgical margins:** High-risk cSCC requires 6–10 mm margins (vs. 4–6 mm for low-risk) 2. **Adjuvant therapy:** PNI warrants consideration of postoperative radiotherapy 3. **Lymph node assessment:** Depth >4 mm may warrant sentinel lymph node biopsy 4. **Follow-up:** Intensive surveillance for recurrence and metastasis [cite:NCCN Guidelines Squamous Cell Carcinoma of the Skin 2023] 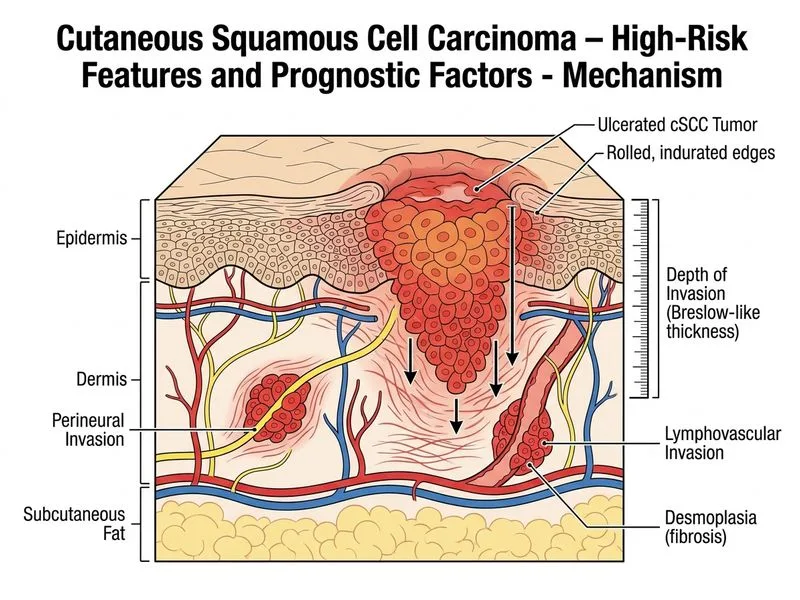
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.