## Clinical Presentation & Imaging Pattern This patient presents with **longitudinally extensive transverse myelitis (LETM)** — a hallmark of **neuromyelitis optica spectrum disorder (NMOSD)**. The key diagnostic features are: 1. **Extensive cord involvement** (≥3 vertebral segments, here T2–T8) 2. **No gadolinium enhancement** (does not exclude acute demyelination) 3. **Normal brain MRI** (typical for NMOSD; MS usually has brain lesions) 4. **Spastic paraparesis** (motor-predominant myelitis) ## LETM: Distinguishing NMOSD from MS **High-Yield:** LETM (≥3 vertebral segments) is the **hallmark of NMOSD**, whereas MS typically causes short-segment myelitis (≤2 segments). | Feature | NMOSD | MS | Acute Transverse Myelitis | |---------|-------|----|--------------------------| | **Cord length** | ≥3 segments (LETM) | ≤2 segments | Variable, often short | | **Brain lesions** | Absent or atypical | Present (>90%) | Absent | | **Optic neuritis** | Severe, bilateral possible | Unilateral, mild | Rare | | **Gadolinium enhancement** | Variable (may be absent) | Usually present | Often present | | **CSF oligoclonal bands** | Absent (90%) | Present (95%) | Variable | | **Serology** | AQP4-IgG or MOG-IgG positive | Seronegative | Seronegative | | **Recurrence** | Frequent | Unpredictable | Rare | **Key Point:** The **absence of gadolinium enhancement does NOT exclude acute demyelination**. Enhancement indicates acute BBB disruption, but its absence does not rule out demyelinating disease, especially in NMOSD where enhancement may be patchy or absent. ## Why NMOSD, Not MS? 1. **LETM pattern** — ≥3 vertebral segments is characteristic of NMOSD and rare in MS 2. **Normal brain MRI** — MS typically shows multiple brain lesions; NMOSD brain involvement is uncommon 3. **Absence of oligoclonal bands** — typical for NMOSD (90% seronegative for CSF OCB) 4. **Severe myelitis** — NMOSD causes more severe cord involvement and worse outcomes than MS **Clinical Pearl:** **Aquaporin-4 (AQP4) antibodies** are present in ~60–70% of NMOSD patients (AQP4-IgG seropositive). **MOG-IgG** is positive in ~10–15% of seronegative cases. Serology testing is essential for diagnosis. ## Why Not MS? MS with LETM is rare; MS typically causes **short-segment myelitis** (≤2 vertebral segments). The normal brain MRI further argues against MS, as >90% of MS patients have brain lesions at presentation. The extensive cord involvement is atypical for MS. ## Why Not Acute Transverse Myelitis (ATM)? ATM is a clinical diagnosis of acute myelitis without a defined etiology. While this patient could have ATM, the **LETM pattern and normal brain MRI** strongly suggest NMOSD rather than idiopathic ATM. NMOSD is now recognized as a spectrum of autoimmune demyelinating diseases and should be suspected in any patient with LETM. ## Why Not Spinal Cord Compression? Spinal cord compression from disc herniation would show: - Mechanical compression (cord displaced, canal narrowed) - Focal cord edema (usually short segment) - No demyelinating pattern - Imaging would show the compressive lesion (disc, tumor, etc.) The extensive T2 hyperintensity spanning multiple segments without a compressive lesion is consistent with demyelination, not mechanical compression. [cite:Harrison 21e Ch 380; Wingerchuk et al. International consensus diagnostic criteria for neuromyelitis optica spectrum disorder. Neurology. 2015.] 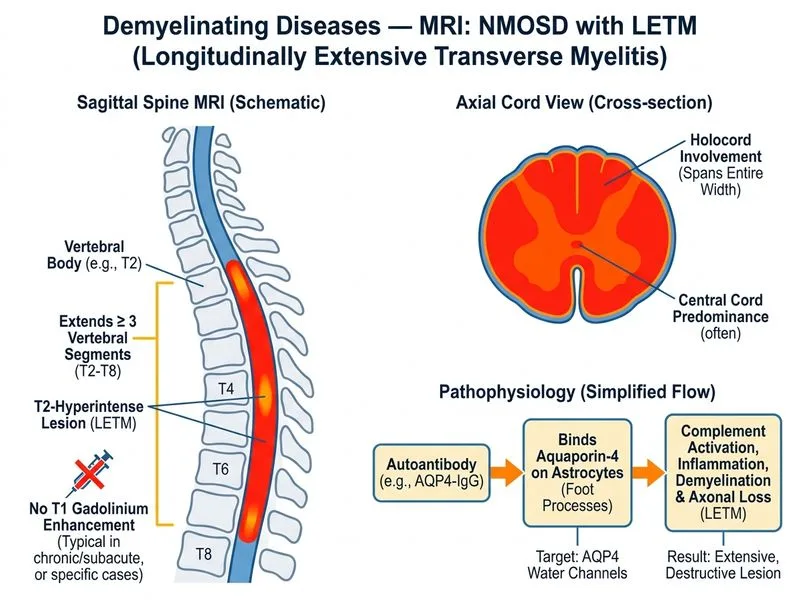
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.