## Clinical Scenario Analysis This patient has progressive neurological deficit (weakness across multiple myotomes: L1–L2, L3–L4, L4–L5) with imaging confirmation of compressive pathology and no cauda equina syndrome signs (bowel/bladder intact). ### Myotome Distribution and Clinical Significance | Myotome | Primary Muscles | Action | Reflex | |---------|-----------------|--------|--------| | **L1–L2** | Iliopsoas | Hip flexion | — | | **L3–L4** | Quadriceps, adductors | Knee extension, hip adduction | Patellar reflex | | **L4–L5** | Tibialis anterior, extensor hallucis longus | Ankle dorsiflexion, great toe extension | — | | **S1** | Gastrocnemius, soleus | Ankle plantarflexion | Achilles reflex | ### Clinical Reasoning **Key Point:** Progressive multi-level myotomal weakness with imaging evidence of nerve root compression (L4–L5 disc herniation) indicates **significant neurological compromise** requiring urgent intervention. **High-Yield:** The presence of progressive weakness (not static pain) across multiple levels with MRI confirmation of compression is an indication for urgent neurosurgery consultation. Corticosteroids reduce nerve root edema and inflammation, providing symptomatic relief while awaiting surgical evaluation. **Clinical Pearl:** Cauda equina syndrome (bowel/bladder involvement, bilateral leg weakness, saddle anesthesia) is NOT present here, but progressive unilateral multi-level weakness still warrants urgent surgical consultation because conservative management has failed (3-week progression despite presumed initial conservative care). **Warning:** Do NOT confuse "no cauda equina syndrome" with "no surgical indication." Progressive myotomal weakness with imaging correlation is a surgical red flag even without cauda equina features. ### Management Algorithm ```mermaid flowchart TD A[Disc herniation with nerve compression]:::outcome --> B{Progressive neurological deficit?}:::decision B -->|Yes| C[Urgent neurosurgery consultation]:::action C --> D[High-dose corticosteroids for edema reduction]:::action D --> E[Plan decompression if no improvement or worsening]:::action B -->|No, static pain only| F[Conservative management: NSAIDs, PT, reassess]:::action E --> G[Laminectomy/discectomy]:::action ``` ### Why This Approach 1. **Progressive weakness** over 3 weeks indicates the nerve root is being increasingly compromised. 2. **MRI confirmation** of L4–L5 compression with multi-level myotomal involvement justifies urgent surgical evaluation. 3. **High-dose corticosteroids** (e.g., methylprednisolone 1 g IV daily × 3–5 days) reduce perineural edema and inflammation, providing symptomatic relief and potentially preventing further neurological deterioration. 4. **Neurosurgery consultation** is urgent because conservative management alone has not halted progression. 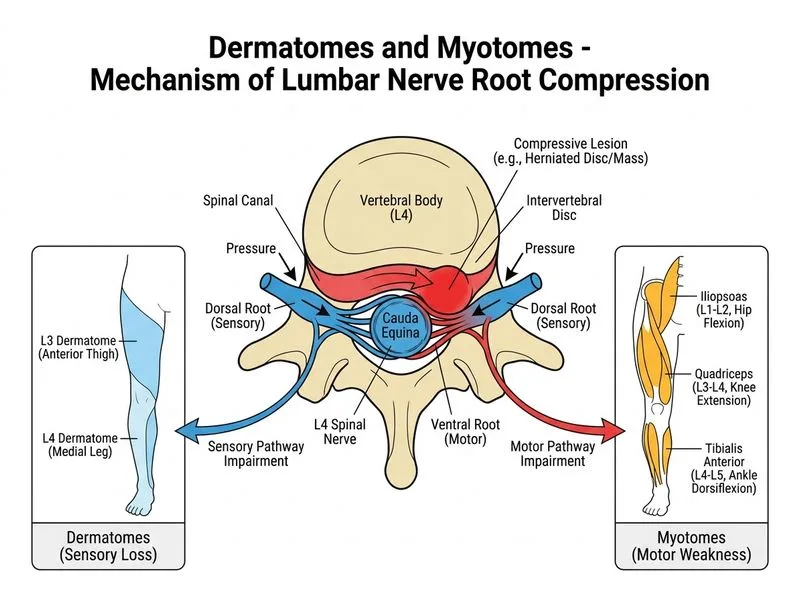
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.