## Clinical Diagnosis: Tinea Cruris ### Key Clinical Features **Key Point:** Tinea cruris (jock itch) is the most common dermatophytosis in tropical regions like India, affecting the groin, inner thighs, and buttocks. The clinical presentation in this case is classic: - Well-demarcated erythematous plaques with **active raised border** (hallmark of dermatophytosis) - Central clearing (creating an annular pattern) - **Sparing of the scrotum** — this is pathognomonic for dermatophytosis and helps distinguish it from candidiasis, which typically involves the scrotum - Pruritic and scaly - KOH mount positive for **septate hyphae** (confirms fungal infection) ### Causative Organisms in Tinea Cruris | Organism | Frequency | Geographic Pattern | Key Features | |----------|-----------|-------------------|---------------| | **Trichophyton rubrum** | 70–80% | Worldwide; most common in India | Anthropophilic; causes chronic infections; slow-growing | | Trichophyton mentagrophytes | 10–15% | Temperate regions | Zoophilic; faster growth; more inflammatory | | Epidermophyton floccosum | 5–10% | Tropical regions | Anthropophilic; less common in India | | Candida albicans | — | — | Causes candidiasis (not dermatophytosis); involves scrotum | **High-Yield:** *T. rubrum* is the most common dermatophyte worldwide and in India. It is slow-growing, anthropophilic (human-to-human transmission), and causes chronic, often asymptomatic infections. ### Why the Scrotum is Spared **Clinical Pearl:** Dermatophytes prefer cooler, drier areas. The scrotum is warm and moist, making it unsuitable for dermatophyte growth. Candida, by contrast, thrives in warm, moist environments and **always involves the scrotum** in candidal balanitis or candidal intertrigo. ### Microscopy and Culture - **KOH mount:** Shows septate hyphae (characteristic of dermatophytes) - **Culture:** *T. rubrum* grows slowly (2–3 weeks) on Sabouraud dextrose agar; colonies are buff to reddish-brown - **Wood's lamp:** Usually negative (unlike *M. furfur* in tinea versicolor, which shows yellow-green or copper-orange fluorescence) **Mnemonic:** **CREAM** — *Candida*, *Malassezia*, *Epidermophyton*, *Trichophyton*, *Microsporum* — but in tinea cruris, think **T. rubrum first**. ### Treatment Algorithm ```mermaid flowchart TD A[Tinea Cruris Diagnosed]:::outcome --> B{Extent & Severity?}:::decision B -->|Localized, mild| C[Topical azole or allylamine]:::action B -->|Extensive or refractory| D[Oral terbinafine or fluconazole]:::action C --> E[Duration: 2-4 weeks]:::action D --> F[Terbinafine: 250 mg daily × 2-4 weeks]:::action D --> G[Fluconazole: 150 mg weekly × 2-4 weeks]:::action E --> H[Cure & prevention]:::outcome F --> H G --> H ``` **Key Point:** Topical agents (azoles like clotrimazole, miconazole; allylamines like terbinafine) are first-line for localized tinea cruris. Oral therapy is reserved for extensive disease, immunocompromised patients, or treatment failure. 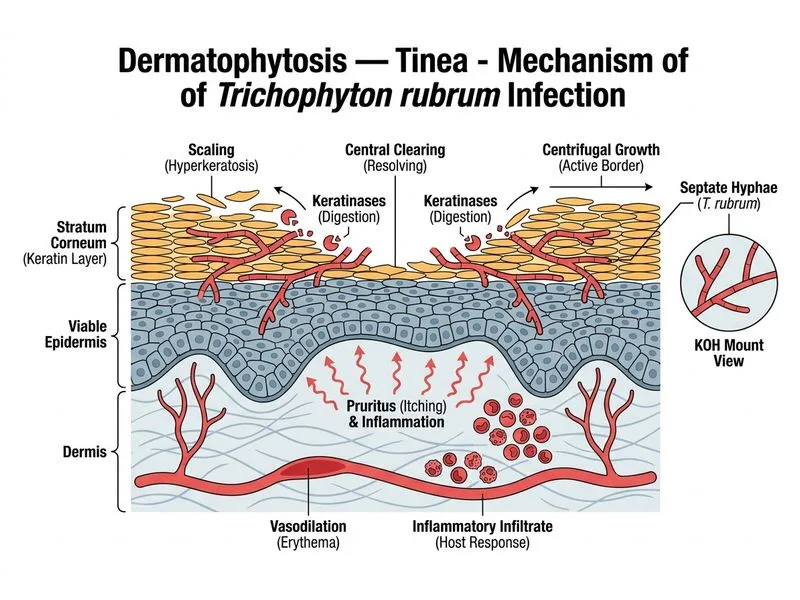
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.