## Clinical Diagnosis: Tinea Capitis (Scalp Ringworm) ### Key Clinical Features **Key Point:** Tinea capitis is a dermatophyte infection of the scalp and hair shaft, most common in children but can occur in adults, especially in tropical regions like India. The clinical presentation strongly suggests tinea capitis: - **Well-demarcated patch of alopecia** with scaling and erythema - **Broken hairs** (not pulled out at the root) — characteristic of dermatophyte invasion of the hair shaft - **Black dot ringworm** — broken hairs that appear as black dots on the scalp; indicates endothrix infection (fungus within the hair shaft) - Progressive course over 2 months - Rural setting (higher exposure to infected animals or contaminated fomites) ### Culture Findings: Trichophyton rubrum **High-Yield:** The culture description is classic for *T. rubrum*: - **Slow-growing** colony (2–3 weeks on Sabouraud dextrose agar) - **Buff or cream-coloured** on the obverse (top) surface - **Red/reddish-brown pigment on the reverse** (bottom) side — this is pathognomonic for *T. rubrum* **Clinical Pearl:** The red pigment on the reverse is due to production of a diffusible pigment (likely a quinone derivative) and is the single most useful colony characteristic for identifying *T. rubrum* in culture. ### Dermatophytes Causing Tinea Capitis: Comparison | Organism | Type | Prevalence in India | Culture Features | Clinical Pattern | |----------|------|-------------------|------------------|------------------| | **Trichophyton rubrum** | Endothrix | Most common (>50%) | Slow; buff obverse; **red reverse** | Black dot ringworm; non-inflammatory | | Microsporum canis | Ectothrix | Rare in India | Fast; white/grey; no red reverse | Inflammatory; zoophilic (animals) | | Trichophyton mentagrophytes | Ectothrix | Moderate | Fast; white; no red reverse | Inflammatory; can be zoophilic | | Microsporum audouinii | Ectothrix | Rare; declining | Slow; grey-white | Non-inflammatory; anthropophilic | **Mnemonic:** **RED REVERSE = T. RUBRUM** — the red pigment on the reverse side of the colony is the diagnostic hallmark. ### Endothrix vs. Ectothrix Infection | Feature | Endothrix (T. rubrum) | Ectothrix (M. canis, T. mentagrophytes) | |---------|----------------------|----------------------------------------| | Fungus location | **Inside** the hair shaft | **Outside** the hair shaft | | Hair appearance | Black dots (broken hairs) | Halo of spores around hair | | Inflammation | Usually mild | Often more inflammatory | | Wood's lamp | Usually negative | May show blue-green fluorescence (M. canis) | | Culture growth | Slow | Fast | **Key Point:** Black dot ringworm is pathognomonic for endothrix infection, and *T. rubrum* is the most common endothrix dermatophyte in India. ### Pathophysiology of Hair Invasion ```mermaid flowchart TD A[Dermatophyte spores contact scalp]:::outcome --> B[Fungus invades stratum corneum]:::action B --> C{Infection pattern?}:::decision C -->|Endothrix| D[Fungus grows inside hair shaft]:::action C -->|Ectothrix| E[Fungus grows outside hair shaft]:::action D --> F[Hair becomes brittle & breaks]:::action E --> G[Spore sheath around hair]:::action F --> H[Black dot appearance on scalp]:::outcome E --> I[Halo of inflammation around hair]:::outcome H --> J[Diagnosis: Tinea capitis endothrix]:::outcome I --> K[Diagnosis: Tinea capitis ectothrix]:::outcome ``` ### Microscopy and Culture - **KOH mount:** Shows hyphae and spores within/around hair shaft (depending on endothrix vs. ectothrix) - **Culture on Sabouraud dextrose agar:** Incubate at 25–28°C for 2–4 weeks - *T. rubrum*: Slow growth, buff obverse, **red reverse** (diagnostic) - *M. canis*: Fast growth, white/grey, no red reverse; may fluoresce blue-green under Wood's lamp - **Wood's lamp:** Usually negative for *T. rubrum*; may be positive for *M. canis* ### Treatment **High-Yield:** Tinea capitis requires **systemic antifungal therapy** because topical agents cannot penetrate the hair shaft effectively. - **First-line:** Griseofulvin 20–25 mg/kg/day for 6–8 weeks (microsize formulation) - **Alternative:** Terbinafine 125–250 mg daily for 4–6 weeks (faster; preferred in some guidelines) - **Adjunct:** Antifungal shampoo (ketoconazole, selenium sulfide) 2–3 times weekly to reduce spore shedding **Clinical Pearl:** Griseofulvin is still widely used in India due to cost and established efficacy, though terbinafine is faster and equally effective. 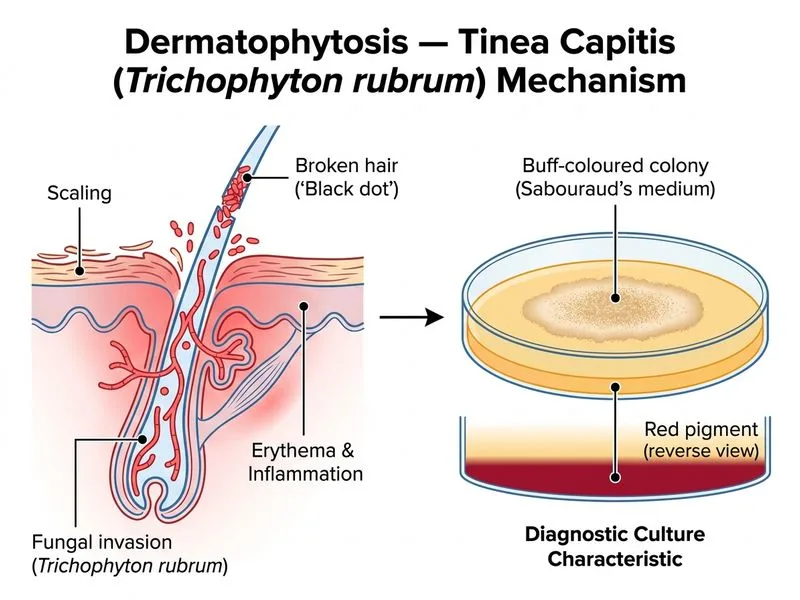
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.