## Clinical Presentation & Diagnosis This 18-month-old presents with: - **Waddling gait** and **positive Trendelenburg sign** → hip abductor weakness/instability - **Asymmetric skin folds** → classic DDH sign - **Positive Ortolani clunk** → femoral head reducible into acetabulum on examination - **Radiographic evidence** of **fixed dislocation** (femoral head displaced superolaterally) - **Risk factor**: Breech presentation **Key Point:** At 18 months, the hip is fixed in the dislocated position. The standard of care for DDH in the **6–18 month age group** is **closed reduction under general anesthesia followed by hip spica cast immobilization**. Traction prior to closed reduction was historically practiced but is no longer universally recommended as the primary approach; current evidence (Campbell's Operative Orthopaedics, Tachdjian's Pediatric Orthopaedics) supports proceeding directly to closed reduction under GA with arthrogram guidance, followed by spica casting. ## Age-Dependent Management Paradigm | Age | Presentation | Management | |-----|--------------|-------------| | <3 months | Unstable (positive Ortolani/Barlow) | Pavlik harness 6–8 weeks | | 3–6 months | Unstable or early fixed dislocation | Pavlik harness or early closed reduction | | **6–18 months** | **Fixed dislocation** | **Closed reduction under GA + hip spica cast** | | >18 months | Fixed dislocation ± contractures | Open reduction ± osteotomy | **High-Yield:** Pavlik harness is **ineffective after 6 months** because the hip is no longer freely reducible; soft tissues have contracted and the femoral head is held in the dislocated position. Observation with physiotherapy alone is never appropriate for a radiographically confirmed dislocation at this age. ## Rationale for Closed Reduction + Spica Cast **Why not Pavlik harness (Option C)?** - Pavlik harness is appropriate only up to ~6 months of age - At 18 months, soft tissue contractures prevent adequate reduction with a harness alone - Risk of "Pavlik harness disease" (posterior dislocation) if used inappropriately **Why not observation/physiotherapy (Option D)?** - Radiographically confirmed dislocation at 18 months will NOT resolve spontaneously - Delay leads to progressive acetabular dysplasia, femoral head deformity, and early osteoarthritis **Why closed reduction under GA (Option A)?** - General anesthesia allows complete muscle relaxation, facilitating gentle, atraumatic reduction - Arthrogram performed simultaneously confirms concentric reduction - Hip spica cast maintains reduction for 6–12 weeks - Success rate: ~70–80% in the 6–18 month age group (Campbell's Operative Orthopaedics, 13th ed., Ch. 32) **Regarding pre-reduction traction (Option B):** - Pre-reduction traction (2–3 weeks) was historically advocated to reduce AVN risk by gradually lowering the femoral head - However, **current evidence does not conclusively demonstrate that traction reduces AVN rates** compared to direct closed reduction under GA - Most contemporary pediatric orthopedic centers (per Tachdjian's Pediatric Orthopaedics, 5th ed.) proceed directly to closed reduction without routine pre-reduction traction - Traction adds hospital stay, cost, and patient discomfort without proven benefit in most series **Clinical Pearl:** The **standard first-line management for DDH at 6–18 months** is **closed reduction under general anesthesia + hip spica cast**. Pre-reduction traction is an adjunct used selectively at some institutions but is not the primary recommended step per current guidelines. [cite: Campbell's Operative Orthopaedics 13e Ch 32; Tachdjian's Pediatric Orthopaedics 5e Ch 20; Herring JA, Tachdjian's Pediatric Orthopaedics] 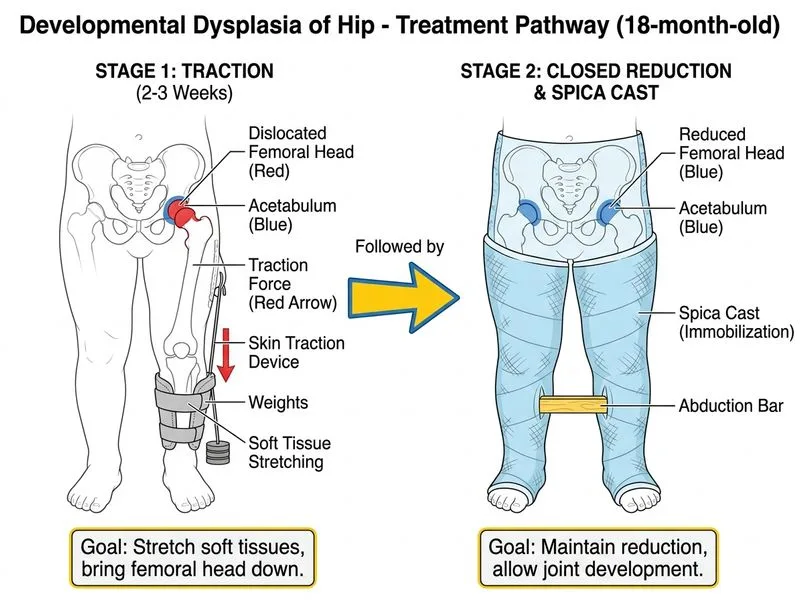
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.