## Clinical Diagnosis This patient has **proliferative diabetic retinopathy (PDR) with vitreous hemorrhage**, evidenced by: - Extensive retinal hemorrhages, cotton-wool spots, venous beading, and IRMA (signs of severe NPDR/PDR) - Sudden floaters and visual loss - Hazy optic disc view due to vitreous hemorrhage - No visible retinal detachment on current exam ## Management of PDR with Vitreous Hemorrhage **Key Point:** Vitreous hemorrhage in the setting of PDR is a surgical emergency. When the view is too obscured to perform pan-retinal photocoagulation (PRP) safely, vitrectomy is the definitive treatment. **High-Yield:** The **DRVS (Diabetic Retinopathy Vitrectomy Study)** established that early vitrectomy (within 6 months of onset) in PDR with vitreous hemorrhage improves visual outcomes, especially in type 1 diabetes. Waiting for spontaneous clearance risks further neovascularization and tractional retinal detachment. ### Decision Algorithm for PDR with Vitreous Hemorrhage ```mermaid flowchart TD A[PDR with vitreous hemorrhage]:::outcome --> B{Can optic disc be visualized?}:::decision B -->|Yes, clear view| C[Pan-retinal photocoagulation]:::action B -->|No, hazy/obscured| D[Vitrectomy]:::action D --> E[Intraoperative PRP + endolaser]:::action E --> F[Improved visual prognosis]:::outcome C --> G[Regression of neovascularization]:::outcome ``` **Clinical Pearl:** In PDR with vitreous hemorrhage, the inability to visualize the optic disc and perform adequate PRP makes vitrectomy the standard of care. The procedure allows simultaneous removal of hemorrhage, intraoperative endolaser treatment, and management of any tractional component. ## Why Not Alternatives? | Option | Rationale | |--------|----------| | **Anti-VEGF injection** | While useful as adjunctive therapy, it cannot clear vitreous hemorrhage or replace PRP. Used pre-operatively to reduce neovascularization burden, not as monotherapy for hemorrhage. | | **PRP under indirect ophthalmoscopy** | Impossible to perform safely when the view is obscured by vitreous hemorrhage. Attempting PRP blindly risks iatrogenic retinal breaks and further hemorrhage. | | **Anticoagulation** | Contraindicated; anticoagulation worsens hemorrhage and delays clotting. | **Tip:** The DRVS study showed that early vitrectomy (within 6 months, ideally within 2–3 weeks) yields better visual outcomes than waiting for spontaneous clearance, particularly in type 1 diabetes where neovascularization is aggressive. [cite:Parson's Diseases of the Eye 22e Ch 11; DRVS Study, Ophthalmology 1997] 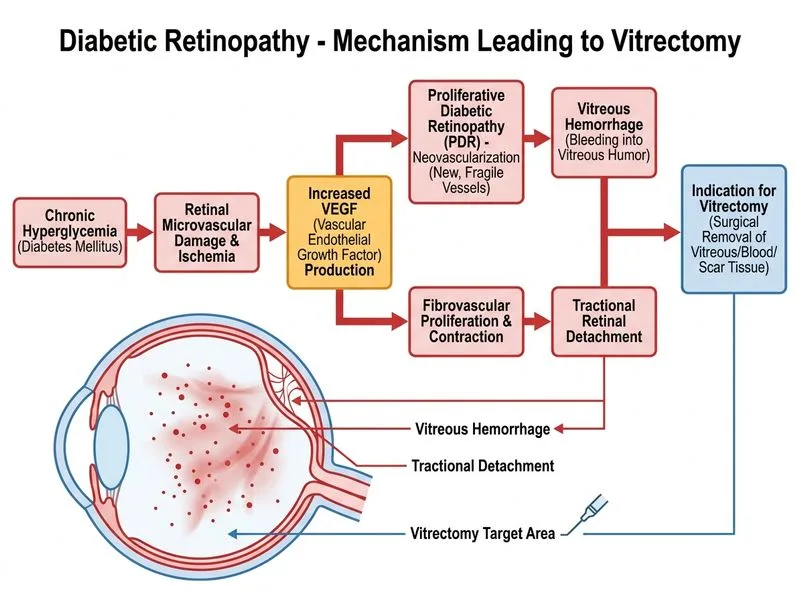
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.