## Clinical Scenario Analysis This patient has **severe nonproliferative diabetic retinopathy (SNPDR)** with high-risk features but **no macular edema and normal vision**. Key findings: - Cotton-wool spots (nerve fiber layer infarcts) - Intraretinal microvascular abnormalities (IRMA—precursor to neovascularization) - Venous beading (sign of retinal ischemia) - NO proliferative disease (no neovascularization) - NO macular edema (no exudates, normal vision) ## Management Pathway for Severe NPDR ```mermaid flowchart TD A[Severe NPDR]:::outcome --> B{Proliferative features present?}:::decision B -->|Yes: NVD, NVE, VH| C[Pan-retinal photocoagulation]:::urgent B -->|No: IRMA, beading, cotton-wool only| D[Risk stratification]:::decision D --> E{Macular edema?}:::decision E -->|Yes| F[Anti-VEGF + Laser]:::action E -->|No| G[Optimize glycemic control]:::action G --> H[Close follow-up in 2-4 weeks]:::action H --> I{Progression to PDR?}:::decision I -->|Yes| C I -->|No| J[Continue monitoring]:::action ``` ## Key Point: **Severe NPDR without macular edema or neovascularization does NOT require immediate laser or anti-VEGF.** The priority is glycemic optimization and close monitoring. PRP is deferred until neovascularization develops or high-risk features progress. ## High-Yield Facts: | Feature | Management Implication | |---------|------------------------| | **SNPDR + No macular edema + No NV** | Glycemic control + close follow-up (2–4 weeks) | | **SNPDR + Macular edema** | Anti-VEGF ± laser | | **Any PDR (NVD, NVE, VH)** | Urgent PRP (within 1 week) | | **SNPDR with high-risk features** | Consider PRP if patient unreliable for follow-up | **High-Yield:** Cotton-wool spots and IRMA are **warning signs** of ischemia but do NOT trigger immediate intervention unless accompanied by neovascularization or macular edema. ## Clinical Pearl: **Venous beading** is a marker of severe retinal ischemia and increases the risk of progression to PDR within 1 year. However, in the absence of neovascularization, close follow-up (not immediate PRP) is appropriate because: 1. Not all SNPDR progresses to PDR 2. Glycemic control can halt or slow progression 3. Premature PRP risks macular ischemia and vision loss ## Mnemonic: **SNPDR High-Risk Features (BEVCAN)** - **B**eading (venous) - **E**xtensive IRMA - **V**enous loops - **C**otton-wool spots - **A**rteriolar narrowing - **N**eovascularization (if present → PDR, not SNPDR) ## Tip: The question emphasizes **normal vision (6/6)** and **no macular involvement**. This is a strong signal that the patient does NOT need immediate laser or anti-VEGF. The focus shifts to **preventing progression** through glycemic optimization and **surveillance**. 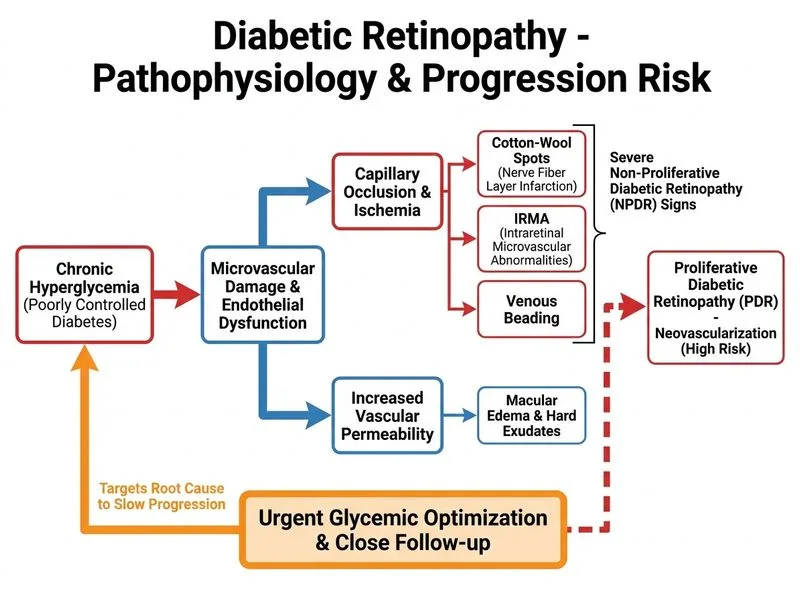
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.