## Management of Severe NPDR with Vitreous Hemorrhage **Key Point:** Severe NPDR with vitreous hemorrhage requires a staged approach: first stabilize the retinal disease with panretinal photocoagulation (PRP), then address the hemorrhage with vitrectomy if it does not clear spontaneously. ### Staging and Severity Assessment This patient has **severe nonproliferative diabetic retinopathy (NPDR)** based on: - Extensive hemorrhages (dot-blot and flame-shaped) - Venous beading - Cotton-wool spots - Prominent IRMA - Absence of neovascularization (not yet proliferative) **High-Yield:** The **Early Treatment Diabetic Retinopathy Study (ETDRS)** established that PRP is indicated for severe NPDR even in the absence of neovascularization, because the risk of progression to proliferative DR within 1 year is >50%. ### Management Algorithm for Severe NPDR + Vitreous Hemorrhage ```mermaid flowchart TD A[Severe NPDR + Vitreous Hemorrhage]:::outcome --> B{Can retina be visualized?}:::decision B -->|Yes| C[Perform PRP immediately]:::action B -->|No| D[Perform PRP with indirect laser or trans-pars plana approach]:::action C --> E[Review in 3 months]:::action D --> E E --> F{Hemorrhage cleared?}:::decision F -->|Yes| G[Continue observation, manage glycemia]:::action F -->|No| H[Vitrectomy]:::action H --> I[Post-vitrectomy PRP if not done]:::action ``` ### Why PRP First? 1. **Prevents progression to PDR** — PRP reduces the risk of neovascularization by destroying ischemic peripheral retina that produces VEGF. 2. **Improves visualization** — Regression of hemorrhages is more likely after PRP because the underlying ischemic drive is eliminated. 3. **ETDRS evidence** — PRP for severe NPDR reduces the risk of severe vision loss by ~50% [cite:ETDRS Report 10]. **Clinical Pearl:** In cases where the retina cannot be visualized due to dense vitreous hemorrhage, PRP can still be performed using **trans-pars plana approaches** or **indirect laser delivery**, or vitrectomy can be performed first to clear the hemorrhage and allow better visualization for subsequent PRP. ### Timing of Vitrectomy - **Immediate vitrectomy** is NOT indicated unless: - Dense hemorrhage persists >3 months - Traction retinal detachment threatens the macula - Neovascularization is actively bleeding and cannot be controlled with PRP - **Wait 3 months** for spontaneous clearance in most cases, as many vitreous hemorrhages reabsorb naturally. **Mnemonic for Severe NPDR Management:** **P-then-V** = **Panretinal photocoagulation first**, then **Vitrectomy** if hemorrhage persists. ### Why Not the Other Options? **Immediate vitrectomy (Option A):** Premature. Vitreous hemorrhage often clears spontaneously within 3 months. PRP must be done first to prevent progression to PDR. **Anti-VEGF alone (Option C):** While anti-VEGF agents are useful in PDR and diabetic macular edema, they are not first-line for severe NPDR. PRP remains the gold standard for severe NPDR. **Focal laser (Option D):** Focal laser is used for diabetic macular edema (hard exudates threatening the macula), not for severe NPDR. This patient's hemorrhage is extensive and not localized to the macula. 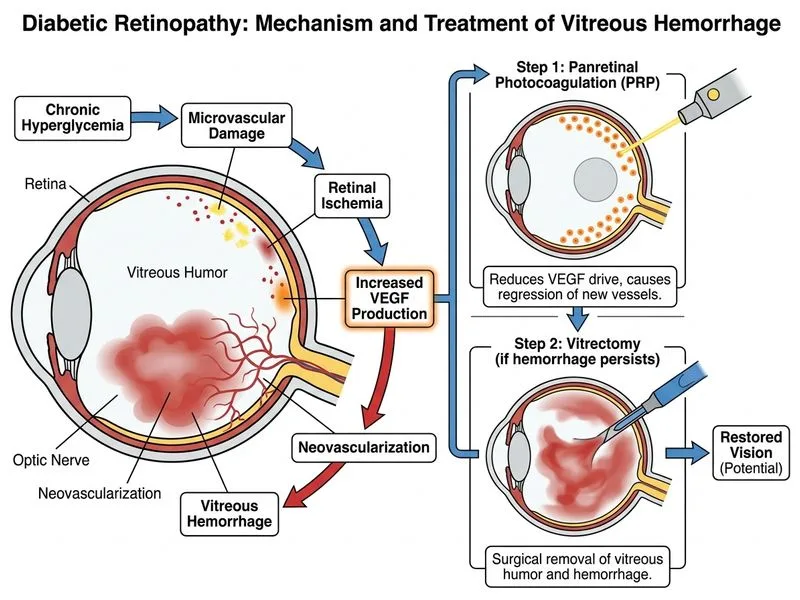
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.