## Clinical Diagnosis This patient has **nonproliferative diabetic retinopathy (NPDR)** with **diabetic macular edema (DME)** — evidenced by hard exudates in a circinate pattern around the macula, dot-blot hemorrhages, and microaneurysms without neovascularization. ## Management Strategy for NPDR with DME **Key Point:** The cornerstone of management in NPDR is **medical optimization** (glycemic and blood pressure control) combined with regular monitoring. Laser and anti-VEGF are reserved for specific indications. ### Why Option 1 (Tight Control + Follow-up) is Correct 1. **Glycemic control** is the primary intervention — HbA1c >9% indicates suboptimal diabetes management, which directly accelerates retinopathy progression. 2. **Blood pressure control** reduces microvascular leakage and exudation (his BP 138/88 is above target for diabetics). 3. **Regular ophthalmology review** (3–6 months) allows detection of progression to PDR or worsening DME requiring intervention. 4. **No neovascularization** means panretinal photocoagulation is not yet indicated. ### When Interventions Are Indicated | Intervention | Indication | | --- | --- | | **Panretinal photocoagulation (PRP)** | Proliferative DR (neovascularization of disc/elsewhere) or severe NPDR at high risk of progression | | **Anti-VEGF (intravitreal)** | DME with central involvement + vision loss; also for PDR if PRP contraindicated | | **Vitrectomy** | Vitreous hemorrhage obscuring view, tractional retinal detachment, or epiretinal membrane | **Clinical Pearl:** The presence of hard exudates and microaneurysms without neovascularization defines NPDR. Tight metabolic control can halt or reverse early NPDR; laser is not first-line. **High-Yield:** NPDR management is **medical, not surgical** — optimize glucose and BP, then monitor. Only escalate to laser/anti-VEGF if progression or DME with vision loss occurs. [cite:Parson's Diseases of the Eye 22e Ch 11] 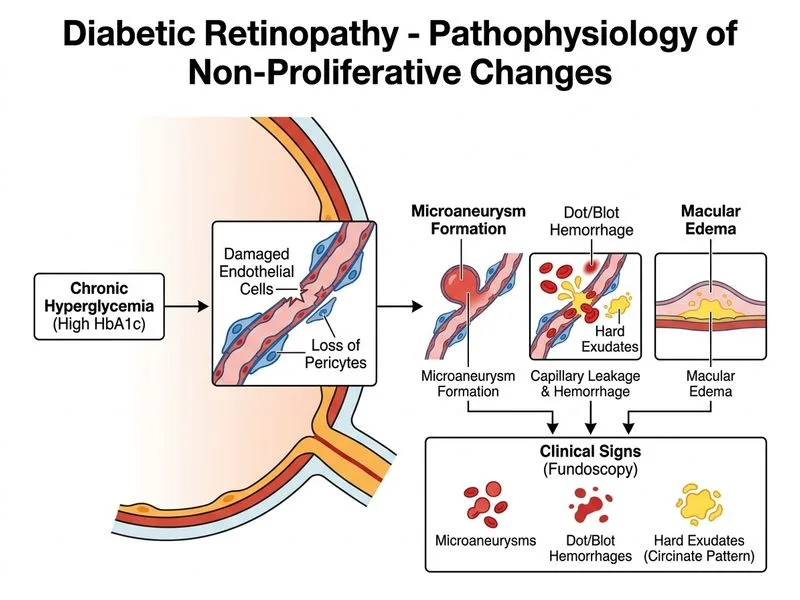
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.