## Clinical Diagnosis This patient has **proliferative diabetic retinopathy (PDR)** with **neovascularization of the disc (NVD)** and **neovascularization elsewhere (NVE)** — the hallmark findings of PDR. The sudden floaters and blurred vision likely reflect early vitreous hemorrhage or traction, but the retina is still visible (fundoscopy is possible), indicating relatively clear media. ## Why Panretinal Photocoagulation (PRP) Alone Is the Most Appropriate Immediate Management **Key Point:** **Panretinal photocoagulation (PRP) remains the definitive, evidence-based first-line treatment for PDR** and has been the standard of care for decades, with proven reduction in severe vision loss by ~50% (ETDRS Report 12). ### Mechanism of PRP 1. **Ablates ischemic peripheral retina** → reduces VEGF production at the source. 2. **Causes regression of neovascularization** within weeks to months. 3. **Prevents vitreous hemorrhage and tractional retinal detachment** — the two most common causes of severe vision loss in PDR. ### Timing of PRP | Finding | Urgency of PRP | | --- | --- | | **NVD (neovascularization of disc)** | **Urgent — within 1 week** | | **NVE (neovascularization elsewhere)** | Urgent if extensive; within 1–2 weeks | | **High-risk PDR** (NVD + vitreous hemorrhage or traction) | **Within 24–48 hours** | | **Severe NPDR** (approaching PDR) | Elective — 2–4 weeks | This patient has NVD + NVE with early vitreous symptoms but clear enough media for fundoscopy — **urgent PRP within 1 week is the standard immediate management** per Parson's Diseases of the Eye and ETDRS guidelines. ### Role of Anti-VEGF (Option A) **Clinical Pearl:** Anti-VEGF agents (bevacizumab, ranibizumab, aflibercept) cause rapid regression of neovascularization but do **not address the underlying retinal ischemia**. Neovascularization frequently recurs if anti-VEGF is used without PRP. The **DRCR.net Protocol S trial** showed that anti-VEGF (ranibizumab) was non-inferior to PRP at 2 years in some PDR patients, but this was in a closely monitored research setting with strict follow-up compliance. In standard clinical practice — especially in a patient with poor glycemic control (HbA1c 10.1%) and high risk of loss to follow-up — **PRP alone remains the preferred immediate intervention** because it provides durable, single-session treatment. Anti-VEGF + PRP combination is a reasonable adjunct in specific scenarios (e.g., PDR with concurrent diabetic macular edema), but is not the standard first-line for PDR without DME. ### Why Other Options Are Incorrect - **Option C (Immediate vitrectomy):** Vitrectomy is indicated for dense non-clearing vitreous hemorrhage (>3 months), tractional retinal detachment threatening the macula, or combined traction-rhegmatogenous detachment. The media here is clear enough for fundoscopy, so vitrectomy is premature. - **Option D (Observation alone):** Observation is never appropriate for PDR with NVD/NVE. Without treatment, the risk of severe vision loss from vitreous hemorrhage or tractional detachment is very high. ### Management Algorithm for PDR ``` PDR diagnosed ↓ High-risk features? (NVD ± hemorrhage/traction) ↓ Yes PRP urgently (within 1 week for NVD alone; 24–48 hrs if NVD + hemorrhage) ↓ DME present? ↓ Yes → Add intravitreal anti-VEGF ↓ No → Monitor at 4 weeks for neovascularization regression ``` **Mnemonic: PDR = PRP (Proliferative Diabetic Retinopathy = Panretinal PhotocoagulAtion)** **High-Yield:** The **ETDRS** established PRP as the gold standard for PDR. Anti-VEGF is increasingly used as adjunctive or alternative therapy in select, closely monitored patients, but **PRP alone performed urgently within 1 week is the most appropriate immediate management** for this clinical scenario. [cite: Parson's Diseases of the Eye 22e Ch 11; ETDRS Report 12; DRCR.net Protocol S, NEJM 2015] 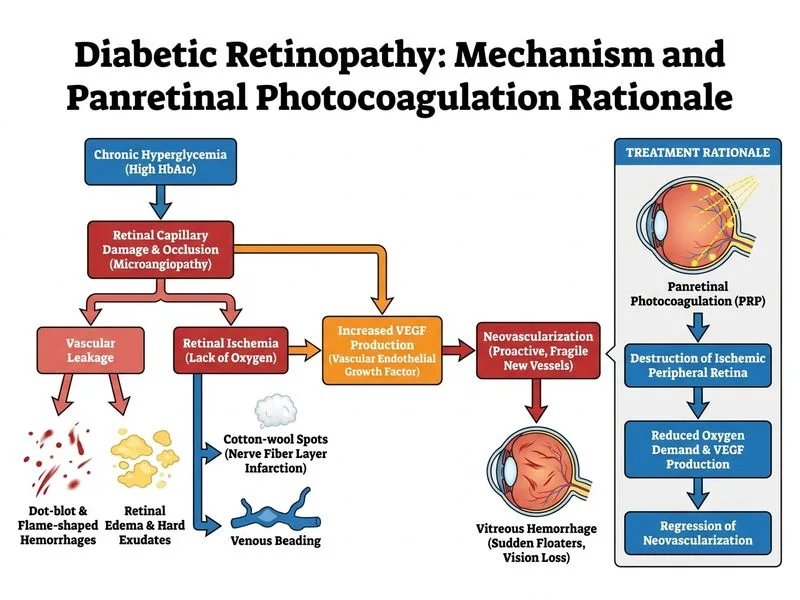
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.