## Clinical Context This patient has **nonproliferative diabetic retinopathy (NPDR)** with **diabetic macular edema (DME)** features (hard exudates in circinate pattern, microaneurysms). Vision is preserved (6/9), and there is no evidence of proliferative disease (no neovascularization, no vitreous hemorrhage). ## Management Algorithm for NPDR **Key Point:** The primary intervention in NPDR without vision-threatening macular edema is **optimization of systemic factors** — glycemic control, blood pressure management, and lipid control — combined with regular ophthalmologic surveillance. **High-Yield:** Pan-retinal photocoagulation (PRP) is reserved for **proliferative diabetic retinopathy (PDR)** or severe NPDR with high risk of progression. This patient does not meet those criteria. **Clinical Pearl:** Hard exudates in a circinate pattern around the macula suggest **clinically significant macular edema (CSME)**, but the patient's preserved vision (6/9) and absence of central involvement mean observation with tight control is the first step. If OCT shows central foveal thickening >250 μm or exudates within 500 μm of the foveal center, anti-VEGF or laser would be indicated. ## Why This Approach? 1. **Glycemic control** (target HbA1c <7%) slows DR progression by ~76% (DCCT/EDIC). 2. **Blood pressure control** (target <130/80 mmHg) reduces DR progression by ~35%. 3. **Statin therapy** reduces hard exudates and vision loss. 4. **Regular follow-up** (every 4 weeks initially for NPDR with exudates) detects progression early. **Mnemonic:** **NPDR Management = CONTROL** - **C**ontrol glucose (HbA1c <7%) - **O**ptimize blood pressure (<130/80) - **N**iperfidil or other agents (if hypertension) - **T**reat lipids (statin) - **R**etinal imaging (OCT, fundus photography) - **O**bserve regularly (4-weekly) - **L**aser only if CSME with foveal involvement or PDR ## When to Escalate | Finding | Next Step | |---------|----------| | NPDR + preserved vision + no CSME | Systemic control + observe | | NPDR + CSME with foveal involvement | Anti-VEGF or laser | | Severe NPDR (4-2-1 rule) | PRP | | PDR (neovascularization present) | PRP or anti-VEGF | | Vitreous hemorrhage | Vitrectomy (if dense/persistent) | [cite:Kanski Clinical Ophthalmology 9e Ch 12] 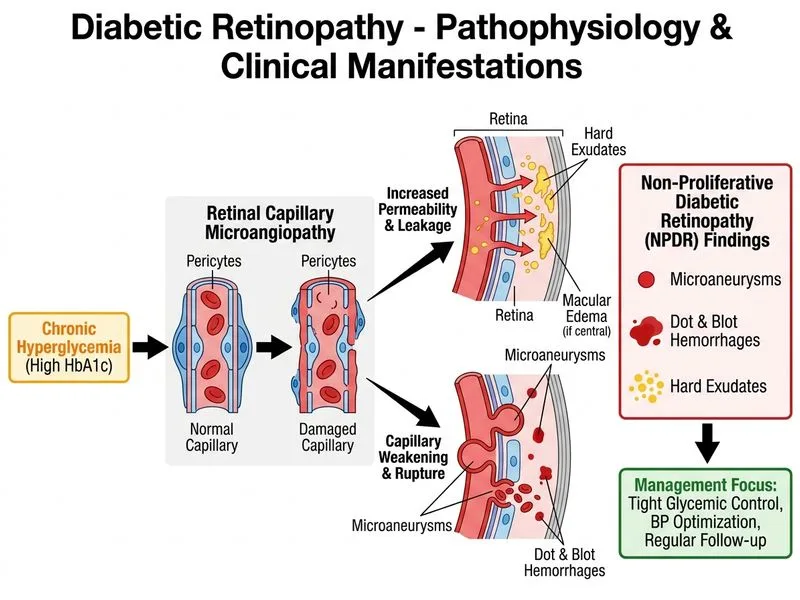
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.