## Distinguishing Phrenic Nerve Injury from Vagal Nerve Injury ### Functional Anatomy of the Phrenic Nerve **Key Point:** The phrenic nerve (C3, C4, C5) is a **somatic nerve** with two critical functions: 1. **Motor:** Sole motor innervation of the ipsilateral hemidiaphragm 2. **Sensory (visceral afferent):** Carries sensory fibers from the parietal pleura, pericardium, and central diaphragmatic peritoneum — these afferents travel back to C3–C5 spinal levels, producing **referred pain/sensation to the shoulder and lateral chest wall** (C3–C5 dermatome territory) > ⚠️ **Correction:** The phrenic nerve does **NOT** carry sympathetic fibers to thoracic or abdominal organs. It is a purely somatic nerve (motor + sensory). Sympathetic innervation of thoracic viscera travels via the thoracic sympathetic chain (T1–T5), not the phrenic nerve. --- ### The Discriminating Feature: Referred Sensory Loss (Option C) **High-Yield:** Phrenic nerve injury causes **referred sensation loss (or referred pain) over the ipsilateral shoulder and lateral chest wall**. This occurs because visceral afferents from the pericardium and parietal pleura travel with the phrenic nerve and converge on C3–C5 dorsal horn neurons that also receive input from the shoulder/chest skin — classic viscerosomatic referral. This finding is **specific to phrenic nerve injury** and does **not** occur with vagal nerve injury. --- ### Comparative Table: Phrenic vs. Vagal Nerve Injury | Feature | Phrenic Nerve Injury | Vagal Nerve Injury | |---------|----------------------|--------------------| | **Hemidiaphragm motor** | Paralyzed (elevated, paradoxical) | **Normal** (vagus does NOT innervate diaphragm) | | **Shoulder/lateral chest sensation** | **Lost / referred pain** (C3–C5 viscerosomatic referral) | Normal | | **Esophageal peristalsis** | Normal | Impaired/absent | | **Laryngeal/vocal cord function** | Normal | Hoarseness, cord paralysis | | **Parasympathetic to thoracic viscera** | Not affected | Impaired | --- ### Why Option D Is Incorrect as the Distinguishing Feature Option D ("inability to elevate the left hemidiaphragm during inspiration") describes **diaphragmatic paralysis**, which is the **shared consequence** of phrenic nerve injury. However, it does **not** distinguish phrenic from vagal injury — because vagal nerve injury also does **not** impair diaphragmatic elevation (the vagus has no motor input to the diaphragm). Both injuries result in the same diaphragmatic status (paralysis from phrenic injury; normal diaphragm from vagal injury), making Option D a feature of phrenic injury but **not a distinguishing comparison point** between the two nerves. --- ### Why Option C Is the Best Distinguishing Feature **Clinical Pearl:** Referred shoulder pain or sensory loss in a patient with hemidiaphragm paralysis points specifically to **phrenic nerve** involvement. A vagal nerve injury would produce hoarseness, dysphagia, and loss of parasympathetic tone — but **never** shoulder/lateral chest sensory changes. This is the classic exam discriminator. ### Mnemonic: "Phrenic = C3-4-5, Shoulder Stays Alive (with referred pain)" Phrenic nerve origin at **C3, C4, C5** → visceral afferents refer sensation to shoulder/lateral chest when the nerve is injured. *(Reference: Gray's Anatomy, 41st ed.; Moore's Clinically Oriented Anatomy, 8th ed.; Snell's Clinical Anatomy)* 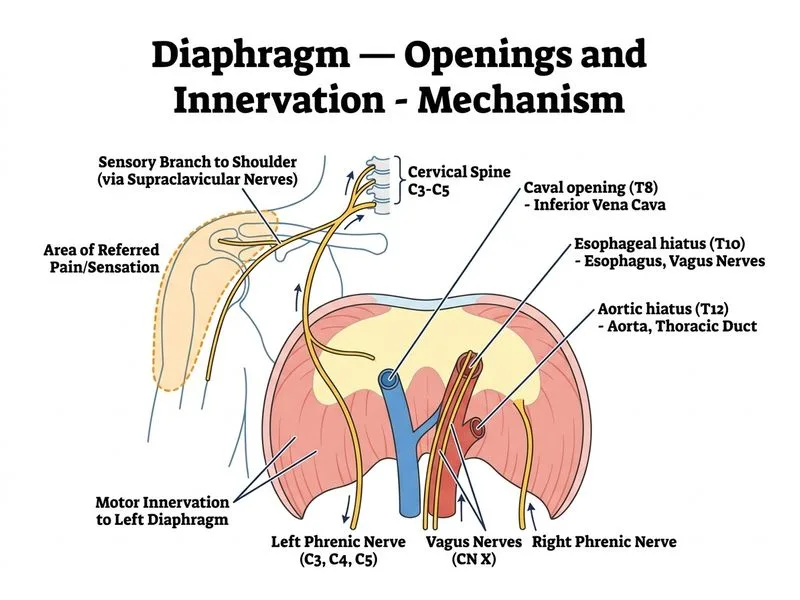
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.