## Clinical Context: Hepatic Hydrothorax and Diaphragmatic Defects This patient presents with cirrhosis complicated by pleural effusion (hepatic hydrothorax). The pathophysiology involves: - Portal hypertension → increased splanchnic pressure - Ascitic fluid transudation through diaphragmatic defects (small fenestrations in the diaphragm, particularly in the right hemidiaphragm near the IVC) - Negative intrathoracic pressure draws fluid into the pleural space ### Anatomical Basis **Key Point:** The diaphragm has natural defects and fenestrations, particularly in the right hemidiaphragm adjacent to the inferior vena cava. These allow bidirectional fluid transfer between the peritoneal and pleural spaces when there is a pressure gradient. **High-Yield:** Hepatic hydrothorax occurs in 5–12% of cirrhotic patients with ascites. The right hemidiaphragm is affected in 80% of cases because: - Larger diaphragmatic defects on the right - IVC passes through the caval opening (T8 level) - Higher ascitic pressure on the right side ### Management Algorithm ```mermaid flowchart TD A[Suspected hepatic hydrothorax]:::outcome --> B{Confirm diagnosis}:::decision B -->|Diagnostic thoracentesis| C[Transudative effusion<br/>Albumin gradient >1.1]:::action C --> D{Rule out other causes}:::decision D -->|Exclude SBP, malignancy, PE| E[Confirm hepatic hydrothorax]:::outcome E --> F{Ascites controlled?}:::decision F -->|Yes| G[Medical management<br/>Diuretics + salt restriction]:::action F -->|No| H[Escalate therapy<br/>TIPS or liver transplant]:::action ``` ### Why Diagnostic Thoracentesis First? 1. **Diagnostic confirmation:** Pleural fluid analysis shows: - Transudative pattern (protein <3 g/dL, LDH <200 IU/L) - Serum-ascites albumin gradient (SAAG) >1.1 g/dL (indicates portal hypertension) - Negative bacterial culture (rules out spontaneous bacterial empyema) 2. **Rule out complications:** - Spontaneous bacterial empyema (SBE): PMN >250 cells/μL in pleural fluid - Malignancy (hepatocellular carcinoma) - Pulmonary embolism - Pneumonia 3. **Therapeutic benefit:** Removal of 1–2 L fluid may provide symptomatic relief **Clinical Pearl:** Hepatic hydrothorax can occur even with minimal ascites; conversely, large ascites may not always cause pleural effusion. The key is the pressure gradient across the diaphragmatic defects. ### Why Not the Other Options? - **Immediate diuretics without diagnosis:** Risks missing serious complications (SBE, malignancy, PE). Also, diuretics are less effective for hepatic hydrothorax than for ascites because fluid continues to transude through diaphragmatic defects. - **TIPS placement:** Indicated only after medical management failure (diuretics + salt restriction + albumin infusion). Premature referral skips the diagnostic step and first-line therapy. - **Chest tube insertion:** Contraindicated in uncomplicated hepatic hydrothorax. High risk of: - Rapid reaccumulation (fluid continues to transude) - Infection (empyema) - Protein loss - Electrolyte derangement - Reserved only for tension hydrothorax or SBE with loculation. **Mnemonic: DIAPHRAGM Defects in Cirrhosis — "I.V.C. Route"** - **I**nferior vena cava opening (T8) has fenestrations - **V**alve-like defects allow ascites → pleural fluid transfer - **C**irrhosis → portal hypertension → pressure gradient - **Route:** Right > Left (80% right-sided) 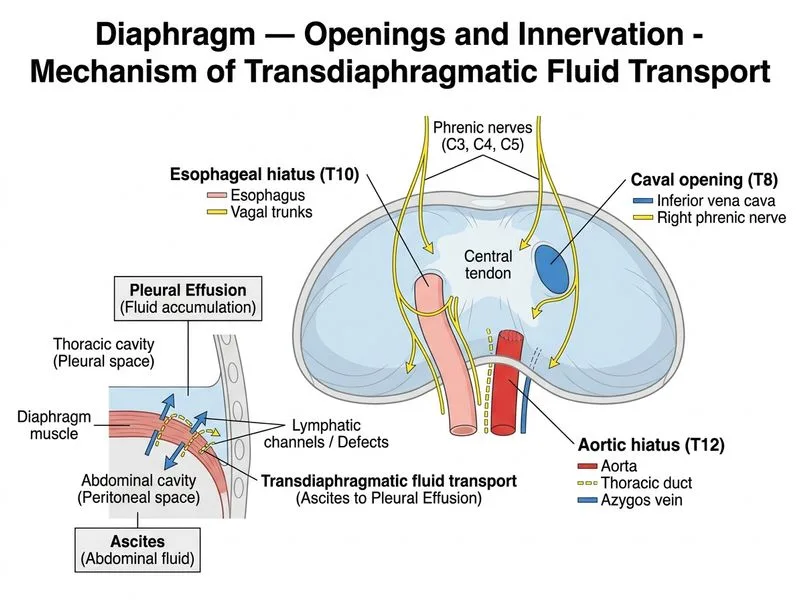
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.