## Clinical Presentation and Diagnosis **Key Point:** DIC in APL is a medical emergency characterized by simultaneous activation of coagulation and fibrinolysis, leading to consumption of platelets, fibrinogen, and clotting factors. ### Why This Patient Has DIC This patient exhibits the classic pentad of DIC: | Finding | Value | Significance | |---------|-------|---------------| | Thrombocytopenia | 15,000/µL | Platelet consumption | | Prolonged PT/aPTT | 18 s / 45 s | Factor consumption | | Hypofibrinogenemia | 85 mg/dL | Fibrinogen consumption + fibrinolysis | | Elevated D-dimer | 8.5 µg/mL | Fibrin formation and degradation | | Clinical bleeding | Epistaxis, petechiae | Microthrombi + factor depletion | **High-Yield:** APL (t(15;17), PML-RARA fusion) is the **most common malignancy associated with DIC** at presentation. The leukemic promyelocytes release tissue factor (TF) and cancer procoagulant, triggering the extrinsic pathway. ### Pathophysiology of DIC in APL ```mermaid flowchart TD A[APL promyelocytes]:::outcome --> B[Release Tissue Factor + Cancer Procoagulant]:::action B --> C[Extrinsic pathway activation]:::action C --> D[Thrombin generation]:::outcome D --> E[Platelet consumption]:::urgent D --> F[Fibrinogen → Fibrin]:::urgent D --> G[Factor V, VIII, II consumption]:::urgent F --> H[Plasmin activation]:::action H --> I[Fibrin degradation]:::action I --> J[Elevated D-dimer & FDPs]:::outcome E --> K[Bleeding + Microthrombi]:::urgent ``` **Clinical Pearl:** The combination of **prolonged PT/aPTT + thrombocytopenia + hypofibrinogenemia + elevated D-dimer** in a patient with APL is pathognomonic for DIC. The Auer rods on smear confirm the APL diagnosis. ### ISTH Scoring for DIC This patient meets criteria for **overt DIC**: - Platelet count <100,000: 1 point - D-dimer/FDP elevation (markedly): 3 points - PT prolongation: 1 point - Fibrinogen <100 mg/dL: 1 point - **Total ≥5 points = compatible with overt DIC** **Mnemonic:** **COAGULATION** — Consumption Of All clotting factors, Organ dysfunction, Activation of coagulation, Granulocytes (leukemia), Urokinase/plasmin (fibrinolysis), Low platelets, Abnormal PT/aPTT, Tissue factor release, Increased D-dimer, Organ bleeding, Necrosis of tissues. ### Management Priority 1. **Immediate:** Fresh frozen plasma (FFP) + cryoprecipitate for factor/fibrinogen replacement 2. **Concurrent:** ATRA (all-trans retinoic acid) + chemotherapy to treat the underlying APL 3. **Avoid:** Heparin is controversial in APL-DIC (risk of hemorrhage > benefit) 4. **Monitor:** Serial PT, aPTT, fibrinogen, platelet count, D-dimer q6–12h **Warning:** Do NOT give platelet transfusions prophylactically in DIC — they may fuel thrombosis. Transfuse only if active bleeding and platelets <10,000/µL or <20,000/µL with fever/infection. [cite:Robbins 10e Ch 13] 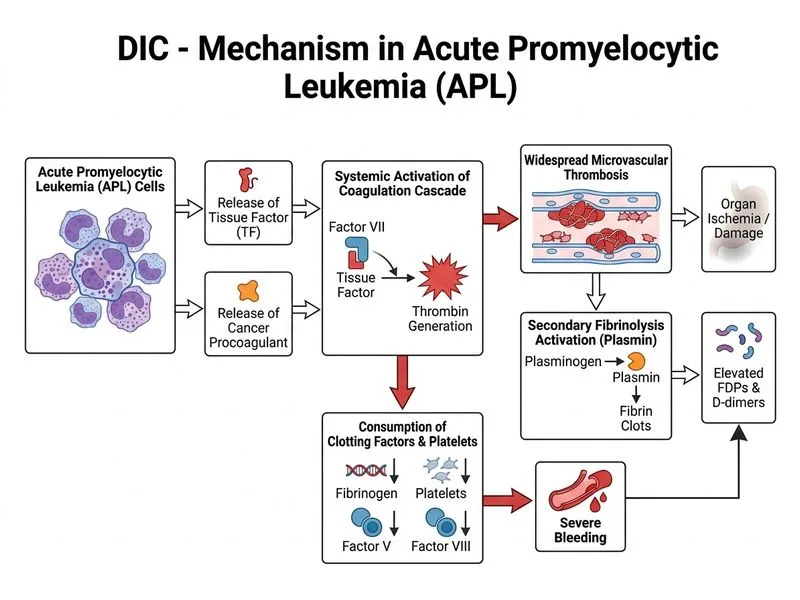
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.