## Clinical Context: Sepsis-Induced DIC This patient has **DIC secondary to septic shock**, the most common cause of DIC in adult ICUs. The pathophysiology involves endotoxin-mediated activation of tissue factor (TF) on monocytes and endothelial cells. ### Diagnostic Criteria Met (ISTH DIC Score) | Parameter | Finding | Interpretation | |-----------|---------|----------------| | Platelet count | 65,000/µL | Moderate thrombocytopenia | | D-dimer/FDP | 8.5 µg/mL (markedly ↑) | Massive fibrin formation | | PT prolongation | 22 sec | Clotting factor consumption | | Fibrinogen | 110 mg/dL | Mild-moderate hypofibrinogenemia | | Schistocytes | Present | Microangiopathic hemolytic anemia | **High-Yield:** ISTH DIC score ≥5 = overt DIC. This patient scores ≥5 and requires immediate management. ### Pathophysiology of Sepsis-DIC ```mermaid flowchart TD A[Gram-negative sepsis]:::outcome --> B[Endotoxin release]:::action B --> C[TF expression on monocytes/endothelium]:::action C --> D[Extrinsic pathway activation]:::action D --> E[Thrombin generation]:::action E --> F[Platelet consumption + fibrin deposition]:::action F --> G[Microvascular thrombosis]:::urgent F --> H[Secondary fibrinolysis]:::action H --> I[Bleeding + organ failure]:::urgent J[Antibiotic + fluid + vasopressor]:::action --> K[Control infection source]:::action K --> L[TF expression ↓]:::action L --> M[DIC resolution]:::outcome ``` ### Why This Answer Is Correct **Key Point:** The cornerstone of sepsis-DIC management is **treatment of the underlying infection and hemodynamic support**, NOT anticoagulation. 1. **Antibiotics:** Broad-spectrum coverage (e.g., piperacillin-tazobactam + fluoroquinolone or carbapenem) to control bacteremia and reduce endotoxin release. 2. **Fluid resuscitation + vasopressors:** Restore perfusion pressure and prevent organ failure (SOFA score reduction). 3. **Supportive transfusion:** FFP for clotting factor replacement, cryoprecipitate for fibrinogen (target >100 mg/dL in bleeding), platelets if <50,000/µL or <100,000/µL with active bleeding, RBCs for anemia. 4. **Why NOT anticoagulation:** Heparin does not improve outcomes in sepsis-DIC and increases bleeding risk. DIC resolves when infection is controlled. **Clinical Pearl:** Sepsis-DIC is a **prothrombotic state masquerading as bleeding disorder**. The primary pathology is microvascular thrombosis (schistocytes, organ failure), not consumption coagulopathy. Anticoagulation worsens bleeding without improving survival. **High-Yield:** The PROWESS trial and subsequent sepsis guidelines (Surviving Sepsis Campaign) recommend **against routine anticoagulation in sepsis-DIC**. Focus on source control and supportive care. [cite:Harrison 21e Ch 325; Surviving Sepsis Campaign Guidelines 2021] 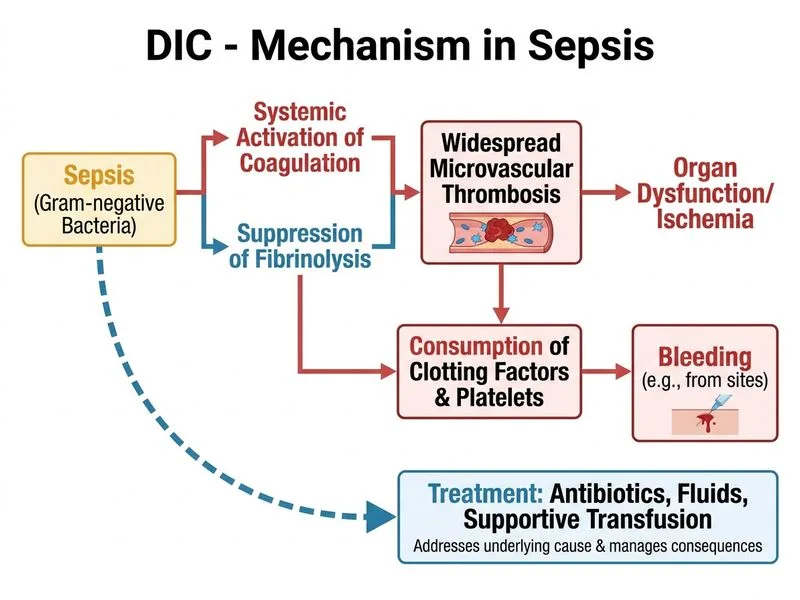
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.